The Development of an Empirical Model for Estimation of the Sensitivity to Heat Stress in the Outdoor Workers at Risk
- *Corresponding Author:
- Nassiri P
Department of Occupational Health, School of Public Health, Tehran University of Medical Sciences, Tehran, Iran.
Tel: 9802538854287
E-mail: nassiri@sina.tums.ac.ir
Citation: Asghari M, Nassiri P, Monazzam MR, Golbabaei F, Arabalibeik H, Shamsipour A. The Development of an Empirical Model for Estimation of the Sensitivity to Heat Stress in the Outdoor Workers at Risk. Ann Med Health Sci Res. 2017; 7:77-84
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.
Abstract
Background: Workers who work in hot environments may be at risk for heat stress. Exposure to heat can result in occupational illnesses, including heat stroke, heat cramps, and heat exhaustion. The risk of exposure to heat depends on individual, environmental, and occupational risk factors. Individual risk factors may decrease the individual’s tolerance to heat stress. Sensitivity as an intrinsic factor may predispose a person to heat stress. Aim: This study was aimed to determine the criteria for sensitivity parameter, specify their weights using the fuzzy Delphi-analytical hierarchy, and finally providing a model to estimate sensitivity. The significant of the study is presenting a model to estimate the sensitivity to heat stress. Materials and Methods: The expert’s opinions were used to extract the criteria in Delphi method. After determining the weight of each criterion, Fuzzy analytic hierarchy Process (FAHP), by mathematical principles matrix and triangular fuzzy numbers, was applied for the prioritization of criteria. Results: According to experts’ viewpoints and considering some exclusion, 10 of 36 criteria were selected. Among 10 selected criteria, age had the highest percentage of responses (90% (27/30)) and its relative weight was 0.063. After age, the highest percentages of response were assigned to the factors of preexisting disease (66.6% (20/30)), body mass index (56.6% (17/30)), work experience (53.3% (16/30)), and clothing (40% (16/30)), respectively. Other effective criteria on sensitivity were metabolic rate, daily water consumption, smoking habits, drugs that interfere with the thermoregulatory processes, and exposure to other harmful agents. Conclusions: Eventually, based on the criteria, a model for estimation of the workers’ sensitivity to heat stress was presented for the first time, by which the sensitivity is estimated in percent.
Keywords
Heat stress, Sensitivity, Personal factors, Fuzzy AHP
Introduction
Working environments include various risk factors such as physical, chemical, biological, and psychological ones. The worldwide growing of technology, in spite of its advantages, may cause the exposure of human to known or unknown harmful agents, resulting in adverse or pathogenic effects. One of the most common occupational health problems in the workplace is working in adverse weather conditions such as hot environments.[1] In addition to reducing the ability of workers, hot environments can cause numerous diseases. Heat stress can lead to different symptoms such as heat exhaustion, heat cramps, heat shock, confusion, fatigue, and loss of concentration, as well as imposing costs because of loss of production, loss of income and increasing of the social costs.[2]
Working in hot environments results in serious impacts on the work force. Exposure to excessive heat occurs in some workplaces such as foundries, glass industry, and metal smelting. [3] Moreover, outdoor work activities expose workers to heat stress. Farmers, construction workers, and open pit miners have to work in hot conditions like warm seasons and direct sunlight, resulting in overheating. The amount of workers’ internal heat depends on metabolic heat, workload, and physical activity. It is estimated that about 80% of the body’s heat load is gained from the physical activity and metabolism, and 20% of it is related to environment.[4]
Based on Australian Statistics, 485 work-related illnesses and injuries resulting from exposure to heat have been occurred over 11 years, from 1997 to 2007.[5] In a similar duration, from 1995 to 2005, the reported illnesses due to heat were 480 illnesses due to the heat were reported in Washington, America.[5] In Japan, 389 deaths occurred during 1989 to 2012 as a result of heat stroke.[6] Between 1992 and 2006, 68 agricultural male workers in America, died due to heat shock in America.[7]
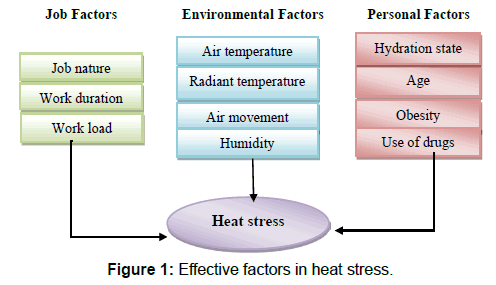
The risk of exposure to heat depends on several factors, that they may provide the conditions for developing some disorders, independently or in combination with other factors. In order to investigate these factors, they can be generally divided into three categories: individual risk factors, environmental risk factors, and occupational risk factors. Figure 1 shows these categories.
According to the third assessment report of the intergovernmental panel on climate change (IPCC), the definition of vulnerability is the degree to which a system or an individual is sensitive to, or unable to adapt to the adverse effects of climate changes. IPCC defines the vulnerability as a combination of sensitivity, exposure and adaptability (Adaptive Capacity).[8]
Sensitivity is the physical capacity of workers to be affected by a hazardous agent like the heat. Sensitive is an intrinsic and internal factor that indicates how the person is vulnerable to thermal stress. Individual risk factors in heat stress may decrease the individual’s tolerance to heat stress.
In various studies, the following factors were mentioned as predisposing ones for diseases and injuries caused by heat stress. Individual factors such as age, shift work, poor physical condition, obesity, heavy activity, heart and cardiovascular diseases, previous heat related diseases, lack of heat acclimatization, fatigue, using alcohol, and drugs that increase the activity of the parasympathetic nervous system.[9,10]
Due to the lack of studies regarding to the sensitivity to heat stress in the working environments, the aim of this study was to determine the criteria for sensitivity parameter using the Delphi technique and expert’s opinions, as well as determining the weight of each criterion using fuzzy hierarchical analysis and finally providing a model to estimate sensitivity parameter.
Subjects and Methods
This qualitative and practical, was designed in 10 stages. Due to the fact that there were no common criteria about the sensitivity parameter, the Delphi technique was used. Delphi technique is a process to collect data and create a consensus among the experts using their judgments. In the other word, this method originally has been developed as a systematic, interactive forecasting method which relies on a panel of experts. This process uses a set of methods for collecting and analyzing the data in combination with the received feedback reports. Using the Delphi method is useful when there is no integrated knowledge about an issue or problem. This method is appropriate, especially when the aim of study is to improve the understanding of the problems, opportunities, and solutions.[11]
Linstone and Turoff believe that Delphi can be considered as a method for structuring a communication process; so that this process allows the group members to solve a complex problem.[12]
Some researchers believe that the participants in Delphi study enter a wide range of knowledge and experience into the decisionmaking process. Also, another advantage of the technique is getting the opinions of experts from vast geographical distances. Additionally, Delphi makes a an inexpensive and efficient method to gain the knowledge and capabilities of a group of experts.[13]
Like other practical research, in Delphi the attention should be paid to planning and effective implementation of study. This technique includes four key activities:
1. Defining the problem
2. Selecting members of the group
3. Determining the group size
4. Implementation of Delphi
Ten steps in implementation of this study include:
1. Establishing of Delphi implementation and monitoring team
2. The selection of experts
3. Adjustment of questionnaire for the first session
4. Questionnaire editing for grammatical and spelling errors (remove any ambiguity)
5. Sending the questionnaire to specialist
6. Analyzing the first questionnaire results
7. Preparing the second session questionnaire with required review
8. Sending the second questionnaire to experts
9. Analyzing of the second questionnaire results
10. Determining the relative weight of each criterion
In the first stage, implementation and monitoring team was formed according to consultants’ advices, and then the objectives of the study were reviewed again. The experts and the Delphi panel members included: members of occupational health department, administration experts working in the health department of Health Ministry, and students who were working on a thesis associated with the heat stress. It should be noted that the number of qualified subjects in this study was 30 experts. According to surveys, if the group in Delphi study is homogeneous, a sample of 10 to 15 participants leads to significant results.[14] A signed informed consent had been obtained from all participants.
After designing open questions about theoretical concepts, they were edited based on recommendations of professors and consultants in order to improve the meaning and validity of questions. Then, the answers of the pilot questions were sent to ten specialists and experts to explore their perceptions of the questions for achieving the desired results. According to the results of the pilot study, the questionnaire was sent to 30 subjects.
Following the analysis of answers obtained from the first session, the criteria were extracted and scored, and also other criteria with lower score were examined. During several meetings with professors, a number of criteria were merged because of the same concept and overlap with each other. Also, a number of criteria were excluded due to non-measurability. At the end of meetings, extracted criteria were used for paired comparison and prioritization at the next session. After sending the second designed questionnaire to the 30 previous subjects, the paired comparisons between criteria were conducted. And finally, the weight of each criterion was determined using the hierarchical model.
Fuzzy analytic hierarchy process
Fuzzy analytic hierarchy Process (AHP), as an effective and strong decision-making technique, was introduced by Thomas El. Saaty. The decision-making in this method is based on qualitative criteria. Moreover, an important source in AHP method is the viewpoints of experts and experienced professionals. In this method, a multi-criteria framework is mathematically designed as a tool for prioritization. The AHP focuses on human thinking and also it utilizes an algorithm based on mathematical logic, therefore, it can be applied as an efficient methodology for problem-solving.[15]
The AHP employs a combination of qualitative and quantitative criteria. The pairwise comparison of criteria provides a way for appropriate decision-making with minimizing the impact of probable interferences. Using this process, perfect judgments are presented in respect to the problem. By AHP, the decision makers enable to assign the numerical values to criteria regarding to their importance. In fact, it shows the importance of various criteria and helps prioritizing them. In this process, after building the hierarchical model for problem of interest, the qualitative and quantitative criteria and their importance are determined by some calculations.[16]
In spite of the simplicity of the AHP method and its community among the decision-makers, there are some uncertainties and problems with the non-fuzzy APH.[16] The uncertainties in obtained information and also in weighting of criteria, as well as unbalanced scale of judgments can be mentioned. The personal judgment by decision-makers may affect the AHP results, greatly. On the other hand, it is not possible to determine an exact numerical value in some pairwise comparisons. In order to modify these uncertainties and avoid the negative impacts on performance, the fuzzification of the conventional method was considered. Development the fuzzy AHP helped obtaining the criteria weights in a fuzzy form, resulting in better prioritization of important factors and making a suitable judgment. Fuzzy logic principle provides determining more reliable and realistic weights and guarantees true decisions in spite of incompleteness of information. In 1996, Chang introduced this fuzzy analytic hierarchy Process (FAHP) that it was a combination of hierarchical analysis and fuzzy logic.[17]
The steps of fuzzy AHP
Developing a fuzzy comparison matrix and determining the linguistic variables
It was used nine basic linguistic terms, as ‘‘Equal”, ‘‘Weak advantage,” ‘‘Not Bad,” ‘‘Preferable,” ‘‘Good,” ‘‘Fairly good,” ‘‘Very good,” ‘‘Absolute” and ‘‘Perfect” with respect to a fuzzy nine level scale. As it can be seen in Table 1. the scale was Triangular Fuzzy Number (TFN) from one to nine, defined by Gumus as the membership function as shown in Table 1.[18] A TFN is fully characterized by a triple of real numbers (l, m, and u), in which, m shows the maximal grade of the membership function μ(x), and parameters l and u are the lower and upper bounds, limiting the field of the possible evaluation.
 (1)
(1)
 (2)
(2)
| Linguistic | Fuzzy number | Scale of Fuzzy number |
|---|---|---|
| Equal | 1 | (1, 1, 1) |
| Weak advantage | 2 | (1, 2, 3) |
| Not bad | 3 | (2, 3, 4) |
| Preferable | 4 | (3, 4, 5) |
| Good | 5 | (4, 5, 6) |
| Fairly good | 6 | (5, 6, 7) |
| Very good | 7 | (6, 7, 8) |
| Absolute | 8 | (7, 8, 9) |
| Perfect | 9 | (8, 9, 10) |
Table 1: Membership function of linguistic scale.
Define Fuzzy geometric means
The fuzzy geometric mean is then calculated using Equation (3).[19]
 (3)
(3)
Where  is a value of fuzzy comparison matrix from criteria i
to n. Result from the fuzzy geometric mean will be referred later
as the local fuzzy number.
is a value of fuzzy comparison matrix from criteria i
to n. Result from the fuzzy geometric mean will be referred later
as the local fuzzy number.
Calculate the weight of fuzzy of each dimension
The next step is to calculate the global fuzzy number for each evaluation dimension with Equation (4)
 (4)
(4)
Define the best non-Fuzzy performance (BNP)
Then the fuzzy number is converted to crisp weight value using the Centre of Area (COA) method to find the value of best BNP from the fuzzy weight in each dimension, calculated using Equation (5).[19]
 (5)
(5)
To assure the quality level of a decision, there is a need for calculation the consistency of an evaluation. The calculated consistency ratio (CR) is defined as a ratio between the consistency of a given evaluation matrix (consistency index CI) and the consistency of a random matrix (consistency index RI). It was expressed as Equation (6).
CR=CI/RI (6)
The CR less than 0.1 showed the comparisons are acceptable. With the CR higher than 0.1, the values of the ratio are indicative of inconsistent judgments.[20]
In this study, only the weighting of the criteria was used. After determining the criteria by the Delphi technique, pairwise comparisons were performed by specialists using Table 1.
Statistical analysis
After collecting the questionnaires, paired comparisons, and determining the priority of each person, the information extraction and analysis was done using Microsoft Excel version 2010 (Microsoft Inc., USA). First, the compatibility degrees of comparisons were determined, the acceptability of them confirmed, and then the mean score of opinions were calculated. Subsequently, the MATLAB software version 9 (R2016a) was applied to calculate the coefficients of each pair comparison for 30 specialists participated in this study.
Results
This study was aimed to determine the effective criteria for sensitivity and their weights using Delphi and Fuzzy Analytic Hierarchy Process (FAHP). After checking and completing the questionnaires, 36 criteria were extracted for sensitivity parameter. During a session with experts, derived criteria from Delphi model were discussed. Given that some of criteria had the same concept, and some others had no relevancy in the present study, they were reduced to 22 criteria. In another review session, due to lower importance of some criteria, the number of criteria was reduced to 10. Table 2 shows the criteria obtained from the Delphi model. The final criteria are shown in Table 3. According to Table 3, the maximum percentage of response (90% (27/30)) is allocated to age criterion. Some criteria such as gender, race, and skin color were excluded due to the low relevancy.
| Extracted criteria | |||
|---|---|---|---|
| 1 | Age | 12 | Drugs that interfere with the thermoregulatory processes |
| 2 | Gender | 13 | Physical health |
| 3 | Previous disease | 14 | Acclimatization level |
| 4 | Body Mass Index | 15 | skin color |
| 5 | work experience | 16 | Exposure to other harmful agents |
| 6 | Clothing | 17 | History of heat-related illness |
| 7 | Smoking Habits | 18 | Temperament |
| 8 | Race | 19 | Life Style |
| 9 | Metabolic Rate | 20 | Sweating condition |
| 10 | daily water consumption | 21 | Nutritional status |
| 11 | Physique | 22 | Fatigue |
Table 2: Extracted criteria by using Delphi technique.
| No | Extracted criteria | Percent | Frequency |
|---|---|---|---|
| 1 | Age | 90 | 27 |
| 2 | Pre ? existing disease | 66.6 | 20 |
| 3 | Body Mass Index | 56.6 | 17 |
| 4 | work experience | 53.3 | 16 |
| 5 | Clothing | 40 | 12 |
| 6 | Smoking Habits | 36.3 | 11 |
| 7 | Metabolic Rate | 33.3 | 10 |
| 8 | daily water consumption | 33.3 | 10 |
| 9 | Drugs that interfere with the thermoregulatory processes | 30 | 9 |
| 10 | Exposure to other harmful agents | 20 | 6 |
Table 3: Final criteria for sensitivity parameter (n=30).
Temperament and life style criteria were excluded due to very low percentage of response. The inability for quantitative measurement and very low percentage of response led to exclusion of the sweat rate criterion. The inconsistency of 0.078 in this study was lower than the acceptable level (0.1), so it was considered reasonable. According to the purpose of the issue, 10 criteria were selected, and their weighting was performed by the Analytic Hierarchy Process. Table 4 indicates the results of the paired comparison.
| No | Extracted criteria | BNP | u | m | l |
|---|---|---|---|---|---|
| 1 | Age | 0.068 | 0.080 | 0.068 | 0. 056 |
| 2 | work experience | 0.058 | 0.071 | 0.058 | 0.045 |
| 3 | Body Mass Index | 0.112 | 0.123 | 0.113 | 0.100 |
| 4 | Pre ? existing disease | 0.094 | 0.109 | 0.093 | 0.080 |
| 5 | Clothing | 0.137 | 0.151 | 0.137 | 0.124 |
| 6 | Metabolic Rate | 0.156 | 0.178 | 0.154 | 0.136 |
| 7 | daily water consumption | 0.139 | 0.162 | 0.136 | 0.119 |
| 8 | Smoking Habits | 0.051 | 0.066 | 0.050 | 0.037 |
| 9 | Drugs that interfere with the thermoregulatory processes | 0.086 | 0.107 | 0.084 | 0.068 |
| 10 | Exposure to other harmful agents | 0.099 | 0.121 | 0.1 | 0.076 |
Table 4: The evaluation matrix coefficients and weightings.
The sensitivity can be computed based on indicators reported above as following formula:
Sensitivity (%) = 0.068A+ 0.058 B + 0.112 C + 0.094 D + 0.137 E + 0.156 F + 0.139 G + 0.051H + 0.086I + 0.099 J
1. Normalized age: The ratio of average age of workers to the assumed maximum permissible age of employment multiplied to 100 (A)
2. Normalized experience: The ratio of average work experience of workers to the assumed maximum permissible experience of employment multiplied to 100 (B)
Normalized BMI: The ratio of average BMI of workers to 27.5 multiplied to 100 (C). It is worth mentioning that according to World Health Organization,[21] the BMI value between 25 to 30 kg/m2 indicates overweight and 27.5 is the average value of this category.[21]
Percentage of workers who have pre-existing disease (D)
3. Percentage of workers that have not appropriate working clothes (E)
4. Normalized metabolism: The ratio of the average working metabolism (W/m2) to 290 (W/m2) multiplied to 100(F). The metabolic rate for very heavy activities is 290 W/m2.
5. Normalized daily water consumption: The ratio of the average daily water consumption to 24 cups (G). National Institute for Occupational Safety and Health (NIOSH) recommends drinking small amounts of water frequently, for instance 1 cup (250 mL) every 15 or 20 minutes.[22]
6. Percentage of smokers (H)
7. Percentage of workers who use drugs (I)
8. Percentage of workers exposed to other harmful agents (J)
Since all indicators are based on the percentage of zero to 100, thus the sensitivity is unit less ranged between 0 and 1.
Discussion
The aim of this study was to identify and determine the effective criteria for sensitivity parameter, based on the opinions of occupational health experts and using the qualitative methods (Delphi model). By analyzing the questionnaires, 33 criteria for sensitive parameters were extracted. Finally, 10 criteria were selected after removing some of them by applying the exclusion factors [Table 3]. Then, Fuzzy Analytical Hierarchical Processing was used for comparison 10 criteria, one by one, in terms of their importance in sensitivity parameter.
According to Table 3, age had the highest percentage of responses (90%) and its relative weight was 0.063. After age, the highest percentages of response were assigned to the factors of pre-existing disease (66.6%), body mass index (56.6%), work experience (53.3%), and clothing (40%), respectively. Table 4 shows the relative weights of these factors.
Studies have shown elderly persons are more sensitive to heat effects and they are susceptible to losing muscle mass.[9] With increasing age, changes in body composition may predispose the workers to some diseases such as diabetes, hypertension, and reduced flexibility, as well as changes in the physical condition of body, lower sweat rates, and increase the skin blood flow. [23,24] In similar environmental situation and metabolic heat loads, older men (over 40 years old) showed a higher risk for heat-related illness compared to people less than 40.[23] On the other hand, total body water decreases with increasing age and it can be an effective factor. Epidemiological studies showed that younger workers are more susceptible to injuries and accidents caused by heat because of doing difficult tasks and lower level of their knowledge about the risk of heat exposure.[5,25]
Result of a study showed that when temperature exceeds 38˚C, more events and injuries happen for older people in smelting industry, although in normal temperature condition younger workers showed higher injury rates than older ones.[26] Briefly, in comparison with many investigations, this study has provided the relative weights for age and other factors.
Body Mass Index (BMI) provides a useful way to measure obesity. It has been proved that the obesity can predispose individuals to Heat-Related Illness (HRI).[27] Low physical fitness combined with overweight cause less surface area, resulting in relatively less evaporative cooling. Another effective factor in HRI is worker’s diet. A high protein diet, which is suggested by some diet may cause increased urea production and excrete the excess urea in the urine. Therefore, worker needs drinking additional amount of water to maintain proper hydration. According to studies the risk of HRI has the positive relationship with body mass index (BMI), and the highest risk is seen in BMI higher than 22 kg/m2.[28]
Overweight individuals with a BMI over 27 are susceptible to heat-related disorders due to the breakdown of the body’s heat control systems. In a survey conducted on farmers in the north of Iran, more than half of them (52%) were overweight or obese. The findings were similar to statistics in some countries such as Greece and Australia (with values of 86% and 64%, respectively). Therefore, there is a need for paying more attention to the health of these workers and reducing their exposure to heat.[29]
Many diseases may intensify disorders caused by heat. The risk factors of blood pressure, diabetes, lung disease, and skin problem can be named in this regard. Also diarrhea, vomiting and lack of sleep can be co-factors in development of heat disorders.[29] The metabolism process, the cardiovascular and also thermoregulatory responses can be affected by low number of red blood cells or anemia. Hypothyroidism in which there is no sufficient amount of thyroid hormone, directly affects the body temperature and metabolism.[30] The findings of a study in Iran showed that about 15% of the farmers suffered from at least one chronic disease such as cardiovascular disease, kidney disease, diabetes or high blood pressure.[29] A national cohort study in Thailand about the relationship between heat stress and occupational injuries has shown 3.6% of the 58495 workers suffered from occupational diseases, and at least 70% of those were younger than 35 years.[31]
It has been reported that using some drugs increases the risk of mortality due to heat in exposed population.[32] Some drugs can affect the human body thermoregulation by different ways including changes in the regulation mechanisms of body temperature, idiosyncratic reactions (hypersensitivity in some people), and allergic reactions.[33]
The medications for high blood pressure, such as beta blockers, can reduce skin blood flow, resulting in reduced convection mechanism. Potential side-effects of prescription drugs during hot weather may decrease the performance, reduce the amount of body water, heart rate, and blood pressure and increase the susceptibility to heat-related disorders.[30]
Some drugs such as antidepressants and bronchodilators interfere with thermoregulation processes that it can alter the heart rate and reduce sweat rates. So, many drugs and therapies should be used cautiously in persons exposed to heat.[29]
A cross-sectional study among farmers in Iran in 2008 showed that at least 13% of them have used the drug at the time of study. [29] Therefore, using drugs should be considered for persons who work in hot environments.
Clothing is an important individual factor affecting thermal comfort. Each type of cloth affects heat transfer from the human and the environment by mechanisms of conduction, radiation, and evaporation. Thermal resistance between body and environment depends on Clothing. Therefore, the role of clothing is maintaining the body temperature in different environments.[34] Clothing thermal insulation indicates the heat transfer between the skin surface and clothes. The “clo” is applied as a unit for thermal insulation of the cloth, so that one clo is equal to 0.155 m2K/W of thermal energy.[35] On the other hand, incorrect selection of appropriate clothing and use of personal protective equipment in the workplace can increase the thermal stress. To Concluding, although the clothing, especially working clothes as a protective factor, protects the individual against harmful agents, lack of a program to select suitable cloths can increase thermal load, causing thermal stress and strain.
Dehydration may cause the reduction in psychological, physical and mental performance [36] and it has been reported in 50% of all heat stroke cases in South African miners.[37] Therefore the fluid lost in sweating must be reciprocated when working in heat, and it should particularly be considered to design the protocols for extended shifts. The imbalance human body water increases core temperature that it may lead to cognitive impairment and affecting the physical performance and coordination, adversely. As a result, increased risk of injuries and accident is potentially probable by dehydration.
According to a study on outdoor workers of the surface mines, the urine samples showed that more than 70% of miners were poorly hydrated and 16% of them experienced the clinical dehydration.[38]
A study on construction workers in Iran reported the same findings.[39] In Nicaragua, the signs of dehydration were seen in nearly 80% of sugarcane workers, as well as 33% severe dehydration.[40]
Smoking habits and using alcohol are related to wide range of disorders such as physiological, mental, and social problems. Cigarette smoking also is a major cause of human death. Smoking habits interferes with body heat dissipation by reduction of the body’s aerobic capacity. Also it may induce the cardiovascular diseases such as high blood pressure, and lead to lower pulmonary ventilation, increasing the person’s susceptibility to heat-related illness.[9]
Metabolism is an important component in respect of the heat stress. The body requires certain internal processes to maintain the living state of the cells. The basal metabolic rate is the summation of these internal processes that the body needs for functions. When the body is subjected to a workload, it requires more energy that it is compensated by a higher metabolic rate. Metabolic rates can be determined by a direct calorimetry or measuring the oxygen uptake (indirect way) in a laboratory, or by estimation. There is a Threshold Limit Value (TLV) for heat stress, proposed ACGIH, and also an empirically derived table of tasks to be converted into metabolic rate (W/hr or Kcal/minute). The three components should be considered, including (a) the base metabolism value, (b) a value related to body position and movement, and (c) the type of work that the person performs.
Conclusion
At the individual level, exposure to a single risk factor may reduce worker’s heat tolerance, while exposure to a combination of several risk factors synergistically increases the risk of heatrelated illnesses. Individual risk factors include age, gender, obesity, fatigue, race, previous heat illness and dehydration. In addition, some diseases (such as cardiovascular disease, diabetes and infectious diseases), use of certain medications, drugs, and alcohol can reduce the heat tolerance.
Therefore, to judge the thermal stress situation in the workplace, it is necessary paying attention to individual parameters in addition to the environmental ones. Also, other parameters related to job and management should be considered to make a correct judgment.
In this study, a model for estimation of the workers’ sensitivity to heat stress was recommended for first time. For this purpose, at first 10 criteria influencing the sensitivity parameter were selected using the Delphi technique, then the weight of each criterion was determined by fuzzy hierarchical analysis, and finally a model to estimate the sensitivity (in percent) was developed. The amount of sensitivity will be between 0-100 percent.
Acknowledgement
This research has been sponsored by Institute for Environmental Research (GrantNo.94-01-46-28540). We are thankful to our colleagues, the professors of occupational health departments, post-graduate students, and the personnel of environmental and occupational health center in the ministry of health, who provided expertise that greatly assisted the research. The authors declare that there is no conflict of interests.
Financial support and sponsorship
This study was financially supported by Institute for Environmental Research and Tehran University of Medical Sciences
Conflicts of interest
There are no conflicts of interest.
References
- Farshad A, Montazer S, Monazzam MR, Eyvazlou M, Mirkazemi R. Heat Stress Level among Construction Workers. Iran J public health. 2014;43:492.
- Golbabaei F, Zakerian SA, Dehaghi BF, Ghavamabadi LI, Gharagozlou F, Aliabadi MM, et al. Heat stress and physical capacity: A case study of semi-professional footballers. Iran J public health. 2014;43:355.
- Asghari M, Nassiri P, Monazzam MR, Golbabaei F, Arabalibeik H, Shamsipour A, et al. Weighting criteria and prioritizing of heat stress indices in surface mining using a Delphi Technique and Fuzzy AHP-TOPSIS Method. J Environ Health SciEng. 2017;15:1.
- Lumingu HMM, Dessureault P. Physiological responses to heat strain: A study on personal monitoring for young workers. J Therm Biol. 2009;34:299-305.
- Xiang J, Bi P, Pisaniello D, Hansen A. Health impacts of workplace heat exposure: an epidemiological review. Industr health. 2014;52:91-101.
- Horie S. Prevention of heat stress disorders in the workplace. JMAJ. 2013;56:186-192.
- Control CD, Prevention. Heat-related deaths among crop workers--United States, 1992-2006. MMWR: Morbidity and mortality weekly report. 2008;57:649-653.
- Change OC. Climate change 2007: Impacts, adaptation and vulnerability. Genebra, Su��a. 2001.
- Rowlinson S, YunyanJia A, Li B, ChuanjingJu C. Management of climatic heat stress risk in construction: A review of practices, methodologies, and future research. Accid Anal Prev. 2014;66:187-198.
- Tawatsupa B, Lim LL, Kjellstrom T, Seubsman S, Sleigh A, Team TCS. The association between overall health, psychological distress, and occupational heat stress among a large national cohort of 40,913 Thai workers. Global health action. 2010;3.
- Asghari NP, Monazzam M R, Golbabaei F, Arabalibeik H, Shamsipour AA, et al. Determination and weighting the effective criteria in selecting a heat stress index using the Delphi technique and Fuzzy Analytic Hierarchy Process (FAHP). JHSW. 2017;7:23-32.
- Ahmadi F NK, Abazari P. Delphi technique: Tool in theinvestigation. Iran J Med Educ. 2008;8:175-185.
- Marshall AP, Currey J, Aitken LM, Elliott D. Key stakeholders? expectations of educational outcomes from Australian critical care nursing courses: A Delphi study. Austr crit care. 2007;20:89-99.
- Hung HL, Altschuld JW, Lee YF. Methodological and conceptual issues confronting a cross-country Delphi study of educational program evaluation. Evaluation and Program Planning. 2008;31:191-198.
- Meixner O, editor. Fuzzy AHP group decision analysis and its application for the evaluation of energy sources. Proceedings of the 10th International Symposium on the Analytic Hierarchy/Network Process, Pittsburgh, PA, USA; 2009.
- Sun CC. A performance evaluation model by integrating fuzzy AHP and fuzzy TOPSIS methods. Expert syst appl. 2010;37:7745-7754.
- Omidvar M, Nirumand F. Risk assessment using FMEA method and on the basis of MCDM, Fuzzy logic and Grey theory-A case study of overhead cranes. JHealth Safety Work. 2017;7:63-76.
- Gumus AT. Evaluation of hazardous waste transportation firms by using a two-step fuzzy-AHP and TOPSIS methodology. Expert syst appl. 2009;36:4067-4074.
- Hsieh TY, Lu ST, Tzeng GH. Fuzzy MCDM approach for planning and design tender?s selection in public office buildings. Int jproject manag. 2004;22:573-584.
- Alavi I. Fuzzy AHP method for plant species selection in mine reclamation plans: Case study sungun copper mine. IranJFuzzy Syst. 2014;11:23-38.
- WHO. Global database on body mass index: An interactive surveillance tool for monitoring nutrition transition. World Health Organization: Geneva. 2012.
- NIOSH. Workplace safety and health topics. Heat stress. US: US national institute for occupational safety and health (NIOSH); 2014.
- Brothers RM, Keller DM, Wingo JE, Ganio MS, Crandall CG. Heat-stress-induced changes in central venous pressure do not explain interindividual differences in orthostatic tolerance during heat stress. J appl physiol. 2011;110:1283-1289.
- Houston DK, Nicklas BJ, Zizza CA. Weighty concerns: The growing prevalence of obesity among older adults. J AmDietc Assoc. 2009;109:1886-1895.
- Estes C, Jackson L, Castillo D. Occupational injuries and deaths among younger workers-United States, 1998-2007. Morbidity and Mortality Weekly Report. 2010;59:449-455.
- Fogleman M, Fakhrzadeh L, Bernard TE. The relationship between outdoor thermal conditions and acute injury in an aluminum smelter. Int j industr ergon. 2005;35:47-55.
- Habibi P, Momeni R, Dehghan H. The effect of body weight on heat strain indices in hot and dry climatic conditions. Jundishapur J health sci. 2016;8.
- Dehghan H, Mortazavi SB, Jafari MJ, Maracy MR. Cardiac strain between normal weight and overweight workers in hot/humid weather in the Persian Gulf. Int jprev med. 2013;4.
- Tirgar SA, Haji Ahmadi M,Hosseini R. Determination of susceptibility to heat-related disorders and prevention methods among agriculture workers. JHSW. 2012;1:39-46.
- Platt M, Vicario S, Marx JA. Rosen's emergency medicine: Concepts and clinical practice 7th ed Philadelphia, Pa: Mosby Elsevier. 2010;57.
- Tawatsupa B, Yiengprugsawan V, Kjellstrom T, Berecki-Gisolf J, Seubsman S-A, Sleigh A. Association between heat stress and occupational injury among Thai workers: Findings of the Thai Cohort Study. Industrial health. 2013;51(1):34-46.
- Michenot F, Sommet A, Bagheri H, Lapeyre-Mestre M, Montastruc J. Adverse drug reactions in patients older than 70 years during the heat wave occurred in France in summer 2003: A study from the French PharmacoVigilance Database. Pharmacoepidemiol Drug Saf. 2006;15:735-740.
- Cuddy MLS. The effects of drugs on thermoregulation. AACN Adv Crit Care. 2004;15:238-253.
- Parvari RA, Aghaei HA, Dehghan H, Khademi A, Maracy MR, Dehghan SF. The effect of fabric type of common Iranian working clothes on the induced cardiac and physiological strain under heat stress. Arch environ occup health. 2015;70:272-278.
- Schiavon S, Lee KH. Dynamic predictive clothing insulation models based on outdoor air and indoor operative temperatures. Build Environ. 2013;59:250-260.
- Kenefick RW, Sawka MN. Hydration at the work site. J Am College Nutr. 2007;26:597-603.
- Jalali M, Aliabadi M, Farhadian M, Negahban S. Investigation of the variation ofurine densityas abiomarker of dehydrationconditionsin workers employed in hotworkplaces. Iran Occup Health. 2014;11:99-110.
- Miller V, Bates G. Hydration of outdoor workers in north-west Australia. J Occup HealthSafAustr NZ. 2007;23:79.
- Montazer S, Farshad AA, Monazzam MR, Eyvazlou M, Yaraghi AAS, Mirkazemi R. Assessment of construction workers? hydration status using urine specific gravity. Int J Occup Med Environ Health. 2013;26:762-769.
- Cortez OD. Heat stress assessment among workers in a Nicaraguan sugarcane farm. Glob health action. 2009;2.




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.