Association of Maternal Working Condition with Low Birth Weight: The Social Determinants of Health Approach
- *Corresponding Author:
- Dr. Masoud Karimlou
Dr. Masoud Karimlou, University of Social Welfare and Rehabilitation Sciences, Tehran, Iran.
E-mail: mkarimlo@yahoo.com
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.
Abstract
Background: The socioeconomic conditions have made more job opportunities available to women. This has created interest to conduct studies on the effect of working lifestyle on pregnancy outcomes. Aim: This study was conducted with the aim to assess the relationship between mothers’ working status as a social determinant and the incidence of low birth weight (LBW) of the newborn. Subjects and Methods: This case–control study was conducted on 500 women with normal weight infants (control group) and 250 women with LBW infants (case group) in selected hospitals in Tehran. Data were collected using a researcher‑made questionnaire, designed to assess the effect of mothers’ prenatal lifestyle, as a social determinant, on LBW of the newborn. A section of the questionnaire involved assessment of mother’s working condition in terms of the work environment, activities, and job satisfaction. Data were analyzed using Chi‑square and logistic regression tests. Results: LBW among employed mothers was 5 times more likely than unemployed ones (odds ratio = 5.35, P < 0.001). Unfavorable work conditions such as humid environment, contact with detergents, and being in one standing or sitting position for long hours were significantly associated with LBW (P < 0.001). Conclusion: The present study showed that unfavorable work conditions were associated with LBW; therefore, they need special attention.
Keywords
Low birth weight, Pregnancy, Socioeconomic factors, Working conditions
Introduction
With the social and economic changes in recent years, women’s roles have also significantly changed and with a considerable increase in women’s share of the job market, 42% of the working population is now women, making up a necessary factor in the national economy.[1] As in most developing countries, along with socioeconomic changes, women’s willingness to work and job opportunities have increased in Iran.[2]
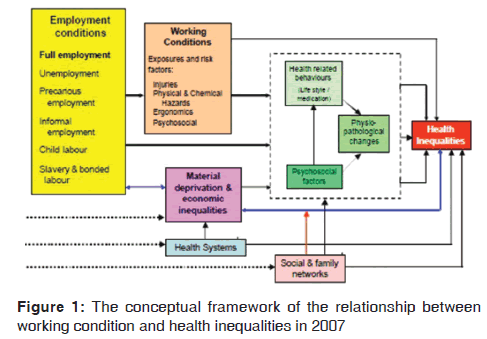
Because of the nature of their gender, women are exposed to different physiological changes including menstruation, pregnancy, and child care that can influence their conditions and type of work.[1] Moreover, more desire of women to work outside home usually means postponing marriage and pregnancy to later years, which eventually affects their personal and social health.[3] Furthermore, work conditions such as stress, prolonged standing, and contact with chemicals could lead to adverse consequences such as spontaneous abortion, preterm birth, low birth weight (LBW), and neonatal abnormalities. There is also published evidence of adverse effects of occupational stress on fetal growth and development.[4] The effect of working conditions on unfavorable pregnancy outcomes is a controversial issue. Working conditions are linked to personal health through psycho-social, behavioral, and psychological mechanisms. These risk factors can be classified into four main categories of physical, chemical, ergonomic, and psychosocial, for example, physical and chemical hazards, repetitive movements, hard and intense physical work, working shift, and lack of control [Figure 1].[5] Therefore, biological, psycho-social, and social differences together with exposure to occupational risk factors create a particular gender pattern for occupational health problems.[1]
Most studies aiming to assess the effects of working conditions on pregnancy outcome did not identify the same working conditions as a risk factor, nor did they consider the relationship between working conditions and adverse pregnancy outcomes such as LBW, while many studies have reported the effects of duration, working shift, and occupational stress on these outcomes.[6-8] Pregnancy outcomes such as LBW and preterm delivery are extremely important and dangerous factors that affect neonatal mortality and morbidity.[9] Birth weight is an important determinant of the newborn’s survival, growth and development, and physical health. In terms of the public health, average birth weight in society indicates the quality of healthcare, availability of care, and nutrition to mothers, and it is a useful benchmark for monitoring the quality of prenatal care and intrauterine growth.[10,11]
Infant birth size reflects two factors: Gestational age and fetal growth. Therefore, it should be considered with gestational age; otherwise, larger size that occurs with aging could interfere with expression of growth and maturity of the fetus.[12] According to the World Health Organization, LBW is defined as weight <2500 g. LBW neonates as compared to normal weight neonates are more likely to be exposed to such risks as cerebral palsy, mental retardation, neurological impairments, respiratory diseases, sudden death syndrome, and intensive care complications. In addition to psycho-physical problems, maintaining and treatment of these infants costs 6 times as much as other infants.[13]
In recent years, despite advances in health, high prevalence of LBW still persists which reflects the need for attention to its influencing factors. The socioeconomic changes in the society and increased number of working women, and also, conflicting results of studies on the effect of occupation on adverse pregnancy outcomes, and lack of studies that would investigate this factor’s relationship with pregnancy outcomes on the one hand, and priority of studying occupational accidents to identify causes mechanisms, and preventative interventions,[9,14] encouraged the researchers to conduct a study in this area.
The present study is the results of part of a larger study titled “the relationship model of mother’s prenatal lifestyle and low birth weight.”
Subjects and Methods
This case–control study was conducted in Tehran in 2012. The data were collected through a researcher-made questionnaire, designed to measure lifestyle with the approach of social determinants of health.
The questionnaire contained 132 items in 10 sections: Three sections covered general characteristics, pregnancy history, and laboratory test results recorded in the file, and seven sections included physical activity, occupation, nutrition, stress control, self-care, social relationships, and inappropriate health behaviors.
Regarding the psychometrics of the questionnaire, face and content validities (qualitative and quantitative aspects), criterion validity,[15] and construct validity (exploratory factor analysis) were used.
Cronbach’s alpha coefficient of 0.709 also confirmed high internal consistency of occupation.[16]
In this study, the results related to occupational lifestyle were presented with 18 items of 5-point Likert style including work environment, duty, working shift, job satisfaction, and employer’s perceived empathy.
In this study, the city of Tehran was first divided into five geographical zones; North, South, East, West, and center.
Subsequently, from the hospitals that had a maternity ward in each zone, clusters that included one or two governmental or social security hospitals, were selected according to their delivery rates. Following a review of literature, the required sample size was determined by considering a 10% prevalence rate for LBW, and calculating research variables. The number of items in the measurement tool and key concepts was determined as 3–10 samples for each variable.[17]
Accordingly, 250 infants with a weight of 2500 g or less were selected as the case group, and 500 infants weighing more than 2500 g were assign to the control group. The inclusion criteria included:
Mothers
• Iranian women 15–45 years old, at a gestational age of 37–42 weeks based on the 1st day of their last menstruation period or sonography, who went to the selected hospitals for their delivery
• Lack of problems such as multiple pregnancy, cardiovascular diseases, diabetes, renal diseases, thyroid disorders, pulmonary diseases, autoimmune disorders, preeclampsia, placental abruption, premature rupture of membranes, hepatitis, AIDS, and other problems. Mothers who had not used any drugs that could affect the birth weight during pregnancy.
Infants
Infants weigh <4500 g, with no known medical problems such as congenital abnormalities and cardiac or pulmonary diseases.
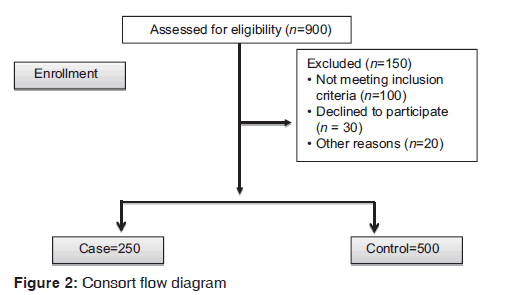
After obtaining permission from university and hospital authorities, we presented the required information to the study population and invited them to participate. The questionnaire was then filled out by a team of trained people. First, the researcher selected mothers with inclusion criteria in the delivery room and monitored them until delivery. At the time of delivery, a researcher went to the delivery room, and immediately after delivery, if the infant had no medical problems, congenital disorders, cardiac-pulmonary diseases, etc., and the infant’s weight was 2500 g or lower using the scale in the delivery room, it was placed in the case group. If it weighed between 2500 g and 4500 g, it was placed in the control group [Figure 2]. Measurement accuracy of all scales in the delivery rooms was determined by the researcher as follows: A standard weight (control weight of 100 g) was used to calibrate the scale after every 10 samples. Following transference of the mother to the postpartum care unit, women who were in a good condition and willing to participate in the study were asked to fill out a consent form.
Questions related to the patient’s file including laboratory test results and ultrasound examinations were completed by the researcher using the mother’s medical file. Another section that included demographic and lifestyle questions was filled out by interviewing the mother.
In this section, information related to other factors affecting LBW such as socioeconomic conditions (family income per annum, education, occupation, household size, spouse’s occupation), pregnancy parameters (age, number of pregnancies), and mother’s health status (blood pressure, increased weight, body mass index [BMI]) were collected and used in the results of this study.
Ethical considerations
The study was conducted following permission obtained from the chancellors of the Tehran University of Medical Sciences, Shahid Beheshti University of Medical Sciences and the General Department of Social Security for their affiliated hospitals. Moreover, prior to the study, the pregnant women signed an informed consent form after they had been informed of the objectives of the study and were assured that their information would remain confidential that they could withdraw from the study at any time and that their privacy was respected.
The study was approved by the Welfare and Rehabilitation Sciences University and the Ethics Committee of the Research Center for the Social Determinants of Health.
Statistical analysis
The data were analyzed and interpreted in SPSS, Version 16 (Chicago, IL, USA) using t-test Chi-square, Fisher and logistics regression at confidence interval of 95% and P < 0.5.
Results
In this study, out of the participating 750 pregnant women (case and control), 12.1% (91/750) were employed, and the rest were a homemaker. There was no significant difference between the two groups in terms of mean age, mean BMI, pregnancy age, pregnancy intervals, and family income. However, mothers’ mean increased weight during pregnancy showed a significant difference between the two groups (P < 0.01). In assessing education levels, chances of having LBW neonates in illiterate mothers were 3 times higher compared to educated mothers (P = 0.03, odds ratio [OR] = 3.27). Spouse’s occupation and mother’s employment were other variables associated with LBW, and with an unemployed spouse, the chances of this outcome would be 4.5 times as much (P < 0.001, OR = 4.49). Mother’s employment versus housekeeper also increased the chance of LBW by 5.4 times (P < 0.001, OR = 5.4). Table 1 presents personal social details of participants in the two groups separately.
| Variables | Normal•mean (SD) | LBWmean (SD) | t-test |
|---|---|---|---|
| Age (years) | 27.34 (5.2) | 27.95 (5.3) | P=0.13 |
| Weight before | 63.07 (11.65) | 63.94 (11.47) | P=0.33 |
| pregnancy (kg) | |||
| Weight gain (kg) | 13.92 (5.29) | 12.68 (5.06) | P<0.01 |
| BMI (kg/m2) | 24.25 (4.14) | 25.54 (4.08) | P=0.35 |
| Hb | 11.98 (1.1) | 11.97 (1.9) | P=0.94 |
| Hct | 36.35 ) 3.6) | 4.1 (36.98) | P=0.22 |
| Interval of | 5.47 (1.17) | 1.39 ) 5.22) | P=0.06 |
| pregnancy (mount) | |||
| Residential density | 26.9 (12.65) | 28.03 (12.99) | P=0.25 |
| per unit | |||
| n (%) | n (%) | &chi2 | |
| Educational | |||
| Illiterate | 5 (1) | 8 (3.2) | P=0.03 |
| Literate | 495 (99) | 242 (5.8) | OR=3.273 |
| CI=1.05-10.11 | |||
| Husbands’ job* | |||
| Unemployed | 12 (2.2) | 23 (9.2) | P<0.001 |
| Employed | 488 (97.8) | 227 (90.8) | OR=4.49 |
| CI=2.15-9.37 | |||
| Mothers job* | |||
| Employed | 29 (5.8) | 62 (24.8) | P<0.001 |
| Housekeeper | 471 (94.2) | 188 (75.2) | OR=5.35 |
| CI=3.34-8.58 | |||
•Normal weight - infants weighing 2500 g and more, Low weight - infants weighing <2500 g, *Significant. OR: Odds ratio, CI: Confidence interval, SD: Standard deviation, BMI: Body mass index, Hb: Hemoglobin, Hct: Hematocrit, LBW: Low birth weight
Table 1: Comparing some personal social factors of research units in the two groups of normal weight and low weight infants 2012
In terms of the work environment and materials that mother had been in contact with, LBW had a significant relationship only with humidity and contact with cleaning materials (P < 0.001). However, other variables, such as noise, had insignificant relationships. Types of activity in prolonged standing and sitting (P < 0.001) and working shift (P = 0.03) were related to LBW. Furthermore, a significant relationship was found between mother’s level of activity (in her own view) (P = 0.023), feeling tired (P < 0.01), work stress (P < 0.01), and job satisfaction (P = 0.01) and this outcomes [Table 2].
| Variables | Normal | LBW | Result | ||
|---|---|---|---|---|---|
| n (%) | n (%) | ||||
| Moisture | |||||
| Always | 1 | (3.4) | 6 | (9.7) | F=16.66 |
| Often | 6 (20.7) | 39 | (62.9) | P<0.001 | |
| Sometimes | 0 (0) | 7 (11.3) | |||
| Seldom | 1 | (4.3) | 2 | (3.2) | |
| Never | 21 | (72.4) | 8 (12.9) | ||
| Noise | |||||
| Always | 5 (17.2) | 2 | (3.2) | χ2=4.16 | |
| Often | 6 (20.7) | 16 | (25.8) | P=0.13 | |
| Sometimes | 4 (13.8) | 14 | (22.6) | ||
| Seldom | 1 | (3.4) | 24 | (38.7) | |
| Never | 13 | (44.8) | 6 | (9.7) | |
| Detergents | |||||
| Always | 0 (0) | 22 | (35.5) | F=26.77 | |
| Often | 8 (27.6) | 20 | (32.3) | P<0.001 | |
| Sometimes | 0 (0) | 11 | (17.7) | ||
| Seldom | 1 | (3.4) | 0 (0) | ||
| Never | 20 | (68.9) | 9 (14.5) | ||
| Standing | |||||
| Always | 8 (27.6) | 9 (14.5) | F=21.27 | ||
| Often | 5 (17.2) | 32 | (51.6) | P<0.001 | |
| Sometimes | 3 (10.3) | 15 | (24.2) | ||
| Seldom | 12 | (41.4) | 4 | (6.5) | |
| Never | 1 | (3.4) | 2 | (3.2) | |
| Sitting | |||||
| Always | 10 | (34.5) | 4 | (6.4) | F=23.58 |
| Often | 6 (20.7) | 26 | (41.9) | P<0.001 | |
| Sometimes | 2 | (6.9) | 22 | (35.5) | |
| Seldom | 11 | (37.9) | 9 (14.5) | ||
| Never | 0 (0) | 1 | (1.6) | ||
| Walking | |||||
| Always | 8 (27.6) | 2 | (3.2) | F=2.14 | |
| Often | 3 (10.3) | 27 | (43.5) | P=0.35 | |
| Sometimes | 7 (24.1) | 19 | (30.6) | ||
| Seldom | 10 | (34.5) | 13 (21) | ||
| Never | 1 | (3.4) | 1 | (1.6) | |
| What was your work shift? | |||||
| Long (a.m. to p.m.) | 13 | (46.4) | 28 | (45.9) | F=12.67 |
| (pm to night) | P=0.03 | ||||
| Night rotation | 0 (0) | 12 | (19.7) | ||
| Afternoon (pm) | 2 | (7.1) | 4 | (6.6) | |
| Morning | 13 | (46.4) | 17 | (27.9) | |
| Using leave in the | |||||
| last 3 months | |||||
| Always | 19 | (65.5) | 32 | (51.6) | F=2.84 |
| Never | 10 | (34.5) | 30 | (48.4) | P=0.21 |
| How tired were you after work? | |||||
| Always | 12 | (41.3) | 31 (50) | F=11.09 | |
| Often | 1 | (3.4) | 15 | (24.2) | P<0.01 |
| Sometimes | 8 (27.6) | 14 | (22.6) | ||
| Seldom | 2 | (6.9) | 2 | (3.2) | |
| Never | 6 (20.7) | 0 (0) | |||
| Stress at workplace | |||||
| Always | 2 | (6.9) | 18 (29) | F=18.65 | |
| Often | 4 (13.8) | 19 | (30.6) | P<0.01 | |
| Sometimes | 7 (24.1) | 20 | (32.3) | ||
| Seldom | 2 | (6.9) | 2 | (3.2) | |
| Never | 14 | (48.2) | 3 | (4.8) | |
| Satisfaction from the workplace | |||||
| Always | 4 (13.8) | 6 | (9.7) | F=23.8 | |
| Sometimes | 5 (17.2) | 18 (29) | P=0.01 | ||
| Seldom | 2 | (6.9) | 16 | (25.8) | |
| Never | 18 | (62.1) | 22 | (35.5) | |
| Sympathy officials in the workplace | |||||
| Always | 16 | (55.1) | 13 (21) | F=15.01 | |
| Often | 4 (13.8) | 33 | (53.2) | P<0.01 | |
| Sometimes | 5 (17.2) | 10 | (16.1) | ||
| Seldom | 2 | (6.9) | 5 | (8.1) | |
| Never | 2 | (6.9) | 1 | (1.6) | |
| Mothers activity (in her opinion) | |||||
| Sever | 14 | (48.3) | 34 | (54.8) | F=16.8 |
| Moderate | 11 | (37.9) | 28 | (45.2) | P=0.02 |
| Low | 4 (13.8) | 0 (0) | |||
| Very low | 14 | (48.3) | 34 | (54.8) | |
The results of the regression test for unfavorable working conditions revealed that chances of LBW were 5 times as much as that with favorable working conditions (P < 0.01, OR = 4.89). The best and worst scores for the questionnaire were 18 and 90, respectively, based on physical, ergonomic, mental conditions of work. Lack of spouse’s help in house (P = 0.04, OR = 1.44) and living in a household with 4 or more people increased the chances of LBW (P < 0.001, OR = 1.78) [Table 3].
| Variables | B | S | E Significant | Exp (B) | CI |
|---|---|---|---|---|---|
| Weight gain (kg) | |||||
| <5 kg | 0.47 | 0.490.33 | 0.62 | 0.23-1.64 | |
| 5-10 kg | 0.25 | 0.200.21 | 0.77 | 0.51-1.15 | |
| 11-16 kg | Reference (1) | ||||
| 17-22 kg | 0.36 | 0.240.13 | 1.43 | 2.29-0.89 | |
| >22 kg | 0.21 | 0.390.59 | 0.81 | 0.37-1.76 | |
| BP (mmHg) | |||||
| Normal | Reference (1) | ||||
| =14.9 | 0.94 | 0.23P<0.001 | 2.56 | 0.24-0.61 | |
| Parity | |||||
| 0 | Reference (1) | ||||
| 2-3 | 0.13 | 0.460.76 | 0.87 | 0.35-2.150 | |
| >4 | 0.49 | 0.360.16 | 0.61 | 0.30-1.23 | |
| Family size | |||||
| 2 | Reference (1) | ||||
| 3 | 0.43 | 0.360.33 | 0.71 | 0.35-1.43 | |
| =4 | 0.58 | 0.270.03 | 1.78 | 0.95-0.33 | |
| Educational | |||||
| Illiterate | Reference (1) | ||||
| Literate | 0.56 | 0.660.39 | 0.56 | 0.15-2.10 | |
| Husbands’ job | |||||
| Employed | Reference (1) | ||||
| Unemployed | 0.83 | 0.450.06 | 0.43 | 0.17-1.05 | |
| Husband’s | |||||
| support at home | |||||
| Yes | Reference (1) | ||||
| No | 0.36 | 0.180.04 | 1.44 | 0.48-0.98 | |
| Working condition | |||||
| Housekeeper | 0.41 | 0.490.40 | 0.66 | 0.25-1.73 | |
| Unfavorable | 1.58 | 0.57P<0.01 | 4.89 | 1.60-14.98 | |
| Favorable | Reference (1) | ||||
LBW=1, Normal=0. LBW: Low birth weight, BP: Blood pressure, SE: Standard error, CI: Confidence interval
Table 3: Relationship among LBW, occupation, and mothers’ personal and social details, attending selected hospitals in Tehran, based on infant’s weight (2012)
Discussion
The results of the study showed that occupational factors have an important role in the incidence of LBW. Working mothers are 5 times more likely to have LBW infants than a homemaker. Among factors, mothers are exposed to at work, humidity, contact with cleaning materials, prolonged standing or sitting; shift work and fatigue were related to LBW.
Based on epidemiological evidence, 5 most common occupational factors of standing and hard physical work, lifting objects, long working hours, and shift working have important roles in many pregnancy outcomes including preterm delivery, LBW, and as prenatal and infant mortality determinant,[11] as well as in preventative factor, and adverse future complications such as growth retardation, neurological and congenital defects, hypertension, insulin-dependent diabetes, and heart diseases.[18] Niedhammer et al. reported that working more than 40 h/week and shift working are associated with increased incidence of LBW, being small for gestational age, and preterm birth. They also found that occasional jobs are a preventative factor in premature births.[9] Bonzini et al. also found that long working hours is associated with increased risk of preterm birth for mothers.[18] Long working hours is also associated with a wide range of other complications such as job-related accidents and injuries, musculoskeletal disorders, fatigue, psycho-social disorders, and unhealthy behaviors.[5]
These consequences can be attributed to increased activity of sympathetic nervous system in muscles following activities such as long hours of standing, sitting, and working shifts; blood return to active muscles from visceral veins; increased sweating; reduced plasma volume and its consequent reduced blood flow to uterine; and placental vessels.[7] Furthermore, there is evidence that hard work, through changes in women’s diet, has a role in unfavorable pregnancy outcomes.[19] Croteau et al. also found a relationship between shift working and being small for gestational age.[20] However, Arafa et al. argued that there was no relationship between long working hours, fatigue, and shift working and adverse pregnancy outcomes.[21] The reason for the difference in results can be due to the fact that in Arafa et al. study, women could not accurately measure durations of standing, sitting, or of any other work activity, and this could perhaps be the main reason for not finding a relationship between these factors. Another very important point is exposure of mothers to situations such as prolonged standing, sitting, and working shifts that increased fatigue in them. Other researchers also considered work-related problems including disrupted sleep, waking rhythm during shift working, humidity, noise, cold, and exposure to chemicals as influential factors in increased fatigue. Fatigue is one of the top 10 health concerns for women.[22] In the present study, work stress, lack of job satisfaction, and perceived understanding of officials for mothers’ conditions were associated with LBW. Factors creating work stresses include poor working conditions, long hours, and poor relationship between colleagues and managers. People’s responses and reactions to these stresses are usually manifested in sleep disorders, digestive system disorder, muscle cramp, shortness of breath, and job dissatisfaction. In addition, work stress can lead to hypertension.[23,24] Work stress, especially in the second trimester of pregnancy is associated with increased level of corticotropin, which can affect LBW directly through passing the placenta or indirectly through maternal vascular function and reduction in uterine-placenta blood flow.[25]
In the present study, mothers with unfavorable working conditions such as physical conditions (humidity), heavy activity, unsuitable psychological conditions (work stress and job dissatisfaction), and chances of having LBW infants were 5 times more compared to women with good working conditions. In other words, apart from mothers’ are employed, unfavorable working conditions are also a very important factor in incidence of low weight. Hawamdeh et al. believe that material deprivations and economic inequities such as improper nutrition, poverty, living conditions, inadequate income due to bad working conditions, both through psycho-social factors and lifestyle-related behaviors, and physiopathological changes have important effects on the incidence of people’s chronic diseases and mental health.[5]
With regard to job and gender, World Health Organization reported women are engaged in hard physical work both at home and work, which leads to adverse pregnancy outcomes although not much information is available on women’s working conditions in low-income countries.[1]
Conclusion
The present study shows that unfavorable work conditions are associated with LBW; therefore, they need special attention.
Strength
A strength of the present study is that study groups matched for confounding factors such as pregnancy age and family income level.
Limitation
Participants in this study consisted of mothers that had attended selected hospitals. Thus, they may have only remembered information close to their delivery. Therefore, it is recommended that a prospective study be conducted in this area, so that different pregnancy months can be compared.
Acknowledgement
This research is derived from a PhD thesis in specialized research on the social determinants of health approved by the Research Council Session in Welfare and Rehabilitation Sciences University dated 16.04.2012, and the meeting of the Ethics Committee of that university 04.12.2011 with no. 91.801.A.2.1227. We appreciate the cooperation by the honorable research deputy of the university and the head of the Research Center for Social Determinants of Health, and all participants in this study.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Overview of Activities 2004-2005 Gender, Women and Health in Headquarters and Regional Offices World Health organization. Department of Gender, Women and Health (GWH); 2006
- Ahmad-Nia S. Women’s work and health in Iran: A comparison of working and non-working mothers. Soc Sci Med 2002;54:753-65.
- Mozurkewich EL, Luke B, Avni M, Wolf FM. Working conditions and adverse pregnancy outcome: A meta-analysis. Obstet Gynecol 2000;95:623-35.
- Mutsaerts MA, Groen H, Buiter-Van der Meer A, Sijtsma A, Sauer PJ, Land JA, et al. Effects of paternal and maternal lifestyle factors on pregnancy complications and perinatal outcome. A population-based birth-cohort study: The GECKO Drenthe cohort. Hum Reprod 2014;29:824-34.
- Benach J, Muntaner C, Santana V, Chairs F. Employment conditions and health inequalities. Final Report to the WHO Commission on Social Determinants of Health (CSDH) Employment Conditions Knowledge Network (EMCONET). Geneva: WHO; 2007.
- Saurel-Cubizolles MJ, Zeitlin J, Lelong N, Papiernik E, Di Renzo GC, Bréart G; Europop Group. Employment, working conditions, and preterm birth: Results from the Europop case-control survey. J Epidemiol Community Health 2004;58:395-401.
- Ebrahim M. The relationship between occupational fatigue and preterm delivery. Iran South Med J 2012:17 (2):233-242
- Vrijkotte TG, van der Wal MF, van Eijsden M, Bonsel GJ. First-trimester working conditions and birthweight: A prospective cohort study. J Inf 2009; 99 (8):1409-16.
- Niedhammer I, O’Mahony D, Daly S, Morrison JJ, Kelleher CC; Lifeways Cross-Generation Cohort Study Steering Group. Occupational predictors of pregnancy outcomes in Irish working women in the Lifeways cohort. BJOG 2009;116:943-52.
- Campos-Serna J, Ronda-Pérez E, Artazcoz L, Moen BE, Benavides FG. Gender inequalities in occupational health related to the unequal distribution of working and employment conditions: A systematic review. Int J Equity Health 2013;12:57.
- Ohlsson A, Shah P, Economics IoH. Determinants and Prevention of Low Birth Weight: A Synopsis of the Evidence. Alberta Perinatal Health Program: Institute of Health Economics; 2008.
- Shah SS. Detection of low birth weight newborns by foot length as proxy-mesaure for birth weight. Welwyn Garden City, UK; Department of Paediatrics and Child Health, Institute of Medicine, Tribhuvan University, Kathmandu, Nepal, India 2005.
- Alexander GR, Wingate MS, Mor J, Boulet S. Birth outcomes of Asian-Indian-Americans. Int J Gynaecol Obstet 2007;97:215-20.
- Yaser J, Mehdi R, Zahra K, Jamil S, Khalil M. Relationship between the occupational accidents and absence frome work employees in Shiraz Namazi hospital. Payavard Salamat 2011;5:59-69.
- Fard MK, Alizadeh R, SehatiShafaei F, Gojazadeh M. The effect of lifestyle on the rate of preterm birth. J Ardabil Univ Med Sci 2010;10:55-63.
- Mahmoodi Z, Karimlou M, Sajjadi H, Dejman M, Vameghi M. Development of mother’s lifestyle scale during pregnancy with an approach to social determinants of health. Glob J Health Sci 2013;5:208-19.
- Munro BH. Statistical Methods for Health Care Research. Wolters Kluwer Health/Lippincott Williams & Wilkins; 2004.
- Bonzini M, Coggon D, Godfrey K, Inskip H, Crozier S, Palmer KT. Occupational physical activities, working hours and outcome of pregnancy: Findings from the Southampton Women’s Survey. Occup Environ Med 2009;66:685-90.
- Behrouzian F, Khajeddin N, Hodaei F, Zamani N. The relationship of job satisfaction and coping mechanism with general health, among private industrial’s staff. Jundishapur Sci Med J 2009;8:353-45.
- Croteau A, Marcoux S, Brisson C. Work activity in pregnancy, preventive measures, and the risk of preterm delivery. Am J Epidemiol 2007;166:951-65.
- Arafa MA, Amine T, Abdel Fattah M. Association of maternal work with adverse perinatal outcome. Can J Public Health 2007;98:217-21.
- Ozgoli G, Nooryazdan SH, Jamal SH, Alavi-Majd H. Fatigue in pregnant women. Nurs Midwifery Fac J 2007;16:12-8.
- Khatoni A, Mlahasani M, Khoeniha S. IC conferences. IJME 2011;11:140-8.
- Aghilinegad M, Attarchi M, Golabadi M, Chehregosha H. Comparing stress level of woman nurses of different units of Iran university hospital in autumn 2009. JAUMS 2010;8:44-8.
- Cunningham F, Leveno K, Blomm S, Hauth J, Rouse D, Spong C. Williams Obstetrics. 23rd ed. Bethesda, Maryland: McGraw-Hill Companies; 2010.
Select your language of interest to view the total content in your interested language
Awards Nomination
20+ Million Readerbase
Google Scholar citation report
Citations : 24805
Annals of Medical and Health Sciences Research received 24805 citations as per google scholar report
Annals of Medical and Health Sciences Research peer review process verified at publons
Indexed in
PubMed Central Index Copernicus Emerging Sources Citation Index
Abstracted/Indexed in
- Include Baidu Scholar
- CNKI (China National Knowledge Infrastructure)
- EBSCO Publishing's Electronic Databases
- Exlibris – Primo Central
- Google Scholar
- Hinari
- Infotrieve
- National Science Library
- ProQuest
- TdNet
- African Index Medicus
 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.