Association of Physical Performance and Fear-Avoidance Beliefs in Adults with Chronic Low Back Pain
- *Corresponding Author:
- Dr. Gurav RS
Department of Musculoskeletal Sciences, MGM College of Physiotherapy, Sector 1, Kamothe, Navi Mumbai - 410 209, Maharashtra, India.
E-mail: reshmagurav81@gmail.com
This is an open access article distributed under the terms of the Creative Commons AttributionNon CommercialShare Alike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.
Abstract
Background: Low back pain is a commonest musculoskeletal disorder affecting majority of people. Activity limitations are difficulties an individual may have in executing activities resulting from person’s functioning and disability. According to the fear‑avoidance model of low back pain, individuals who perceive pain as a sign of potential damage are more likely to avoid behaviors that increase their anxiety and show sub‑maximal performance during physical activity.Aim: Purpose of this study was to find the association between activity limitation and fear avoidance belief in patients with chronic low back pain. Subjects and Methods: Thirty subjects with chronic low back pain were included in the study. Activity limitation was measured using Back Performance Scale (BPS). Patients’ fear of pain and avoidance of physical activities was assessed with Fear Avoidance Belief Questionnaire (FABQ). Results: It was observed that performance was affected in roll up, fingertip to floor and lift test. In the two subscales of FABQ, 47 percent had more fear in physical activity component and 27 percent had more fear in work component. The scores of BPS and FABQ were correlated using Pearson’s correlation test showed strong positive correlation (r = 0.685, P value < 0.01). Higher scores on FABQ are indicative of greater fear and avoidance beliefs. Conclusion: Higher scores on the FABQ 47% in physical activity and 27% in work component are indicative of greater fear and avoidance beliefs. A strong relationship exists between elevated fear avoidance beliefs (FABQ) and activity limitation (BPS) in patients with chronic low back pain.
Keywords
Activity limitation, Back performance scale, Fear avoidance beliefs, Low back pain
Introduction
Chronic low back pain (CLBP) is defined as pain that persists for 12 weeks or longer, even after an initial injury or underlying cause of acute low back pain (LBP) has been treated. [1] About 20% of people affected by acute LBP develop CLBP with persistent symptoms at 1 year. [2] LBP is a most common musculoskeletal disorder involving the muscles and bones of the back. It affects about 40% of people at some point in their lives. [3] Activity limitation is a difficulty an individual may have in executing activities, which results from person’s functioning. [4] LBP is the leading cause of physical impairments and work absence throughout much of the world, and it causes an enormous economic burden on individuals, families, and communities. [2] Studies conducted in developed countries have shown that seven million adults have physical impairments as a result of CLBP. [5]
The consequences of back pain are described as a melting pot of dysfunction affecting psychological, social, occupational, and family life. [6] Bodily pain, limitation of physical activities, and role limitation due to physical health are frequently occurring problems in this group of patients. Back performance scale (BPS) involving physical performance tests of daily activities is a measurement tool which has been found to reflect important aspects of physical functioning in patients with long-lasting back problems. [7] Pain problems have been viewed as complex, multidimensional developmental processes where various psychosocial factors are of the utmost importance. [8,9]
Fear of movement – kinesiophobia – has emerged as a significant predictor of pain-related outcomes including disability and psychological distress across various types of pain. Exacerbation of fear, possibly generating a phobic state in LBP results in long-term consequences in the initiation and maintenance of chronic pain disability. Fear-avoidance, which refers to the avoidance of movements or activities based on fear, has been put forth as a central mechanism in the development of long-term back pain problems. In particular, fear-avoidance is thought to play an instrumental role in the so-called deconditioning syndrome. [10].
Previous studies have shown that pain-related fear is a strong predictor of self-reported disability in both acute and CLBP. [10-14] Several studies have also reported that in patients with CLBP, pain-related fear is significantly associated with restricted physical performance. [15,16]
The fear-avoidance belief questionnaire (FABQ) is a questionnaire based on the fear-avoidance model of exaggerated pain perception. The FABQ measures patient’s fear of pain and consequent avoidance of physical activity (PA) because of their fear. [14] Thus, the FABQ is an outcome measure that serves as a clinically useful screening tool in identifying patients with high fear-avoidance belief who are at risk for prolonged disability.
Most of the previous studies have used self-report disability scales (e.g., the Oswestry LBP disability questionnaire, Roland–Morris disability questionnaire) to measure physical performance; however, the purpose of this study was to find the relationship between physical performance and fear-avoidance beliefs in adults with CLBP.
Subjects and Methods
Thirty subjects with CLBP visiting Musculoskeletal Physiotherapy Outpatient Department of MGM Hospital, Kamothe, Navi Mumbai, were included in the study after obtaining ethical approval from MGM College of Physiotherapy research review committee. Study period was 3 months. The inclusion criteria were patients with mechanical LBP secondary to degenerative conditions of low back (more than 3 months). Exclusion criteria were patients with inflammatory, infectious, malignant conditions of spine, postsurgery patients with LBP, and pregnant women. Informed consent was taken from all the subjects. The basic demographic data (age, gender, occupation) were recorded. The intensity of LBP was measured using numerical rating scale (NRS) ranging from 0 to 10. Higher scores indicate greater pain intensity (0 = no pain, 10 = worst possible pain).
Physical performance was measured using BPS. It is a reliable and valid scale which measures daily activities requiring mobility of the trunk. It includes sock test, pick-up test, roll-up test, fingertip-to-floor test, and lift test (intraclass correlation [ICC] was 0.91).
The BPS is a 16-point scale ranging from 0 to15. Each BPS test was scored from 0 to 3 over the 4-point ordinal scales according to the observed physical performance level. A score of 0 was considered a good performance with no signs of physical impairment, a score of 1 was considered a somewhat limited performance, a score of 2 was considered a rather distinct limitation of performance, and a score of 3 was considered a substantially limited performance if performed at all. Total score was calculated by adding the individual scores of the 5 tests. Higher the score less is the physical performance. [7]
The five BPS tests which involve trunk mobility and combined movement are useful to assess physical impairments in patients with back pain. These tests, which entail harmonious movement of body and lower limbs, begin from different starting positions such as standing and require different angular values of knees. The tests and scoring alternatives are described in Table 1.
| Tests | Performance | Scoring categories (therapist circle scores) | Scores |
|---|---|---|---|
| Sock test | The patient is sitting on a high, firm bench, the feet not reaching the floor. One leg is tested at the time - the least reach scored Instruction: Can you grab your toes with fingertips of both hands when the leg is flexed in the sagittal plane? |
Can easily grab the toes with fingertips of both hands | 0 |
| Can hardly grab the toes with fingertips | 1 | ||
| Can reach beyond the malleoli, but not reach the toes | 2 | ||
| Can hardly, if at all, reach as far as to the malleoli | 3 | ||
| Pick-up test | The patient is standing on the floor. A curled piece of paper is dropped on the floor Instruction: Can you pick up the paper? Can you do it in different ways showing flexibility of the trunk? |
Can do the task with ease in varied ways | 0 |
| Can do the task with minor effort or some decreased variability | 1 | ||
| Can do the task with marked effort or lack of flexibility, may need support of hand on thigh | 2 | ||
| Cannot perform the task at all or need external support | 3 | ||
| Roll-up test | The patient is lying supine on a firm mattress Instruction: Can you roll up slowly into a long-sitting position, with arms relaxed? |
Can roll up with ease, to a long-sitting position | 0 |
| Can roll up with marked effort or partially to long-sitting position | 1 | ||
| Can roll up in supine between the 8th and 12th thoracic vertebra | 2 | ||
| A roll-up above the 8th thoracic vertebra, supine | 3 | ||
| Fingertip-to-floor test |
The patient is standing on the floor, feet 10 cm apart and knees straight Instruction: Can you reach as far as possible to the floor? |
Can reach to the floor, distance=0 cm | 0 |
| Can reach to a distance>0 cm, ≤20 cm | 1 | ||
| Can reach to a distance>20 cm, ≤40 cm | 2 | ||
| Can reach to a distance>40 cm | 3 | ||
| Lift test | The patient is standing on the floor in front of a table Instruction: Can you repeat lifting this box, containing a sandbag of 5 kg, for 1 minute, from the floor to the table (height 76 cm) and back to the floor using an optional technique The box, with grip: 1.35 kg, sized 0.36 cm × 0.36 cm × 0.25 cm |
Can do the lifting task>15 times | 0 |
| Can do the lifting task>10, ≤15 times | 1 | ||
| Can do the lifting task>0, ≤10 times | 2 | ||
| Cannot do the lifting task=0 | 3 |
The patient is to wear loose clothing and no shoes. The activities are explained and demonstrated to the patient. BPS scale: 0-15
Table 1: Back Performance Scale - test protocol
After assessment of physical performance, patients’ fear of pain and avoidance of physical activities were assessed using the FABQ, which is a self-report health questionnaire. The therapist administrating the FABQ was blinded to the BPS score of the patient. The FABQ consists of 2 subscales, the first subscale (items 1–5) is the PA subscale (FABQ-PA) and the second subscale (items 6–16) is the work subscale (FABQ-W) as described in Table 2. Each subscale was graded separately by summing the responses respective scale items (0–6 for each item); for scoring purposes, only 4 of the PA scale items are scored (sum items 2, 3, 4, and 5) and only 7 of the work items (sum items 6, 7, 9, 10, 11, 12, and 15). The physical activities’ score was classified as low fear (0–14 points) or high fear (15 points or more). Work subscale score was classified as low fear (0–33 points) or high fear (34 points or more). [17] The reliability of total FABQ is 0.97 (ICC = 0.97) and the evidence shows that the FABQ is correlated with Roland– Morris disability questionnaire. The correlation coefficients for the FABQ, FABQ-W subscale, and FABQ-PA subscale are 0.52, 0.63, and 0.51, respectively.
| Questions | Completely disagree | Unsure | Completely agree | ||||
|---|---|---|---|---|---|---|---|
| Here are some of the things which other patients have told us about their pain. For each statement please circle any number from 0 to 6 to say how much physical activities such as bending, lifting, walking or driving affect or would affect your back pain | |||||||
| 1. My pain was caused by physical activity | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
| 2. Physical activity makes my pain worse | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
| 3. Physical activity might harm my back | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
| 4. I should not do physical activities which (might) make my pain worse | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
| 5. I cannot do physical activities which (might) make my pain worse | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
| The following statements are about how your normal work affects or would affect your back pain | |||||||
| 6. My pain was caused by my work or by an accident at work | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
| 7. My work aggravated my pain | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
| 8. I have a claim for compensation for my pain | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
| 9. My work is too heavy for me | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
| 10. My work makes or would make my pain worse | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
| 11. My work might harm my back | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
| 12. I should not do my normal work with my present pain | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
| 13. I cannot do my normal work with my present pain | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
| 14. I cannot do my normal work till my pain is treated | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
| 15. I do not think that I will be back to my normal work within 3 months | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
| 16. I do not think that I will ever be able to go back to that work | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
Source: Waddell et al.[14] Scoring: Scale 1: Fear-avoidance beliefs about work - items 6, 7, 9, 10, 11, 12, 15, Scale 2: Fear-avoidance beliefs about physical activity - items 2, 3, 4, 5
Table 2: Fear-Avoidance Beliefs Questionnaire
The association of physical impairments on BPS and fear of pain and avoidance of physical activities on FABQ in patients with CLBP was found using Pearson’s correlation test. Data analysis was done using the SPSS for Windows, version 16.0., SPSS Inc., Chicago, IL, USA.
Results
The demographic data of our study showed that 73% (22/30) were males and 27% (8/30) were females with the mean (standard deviation [SD]) age of 36 (9) years. All patients reported LBP on activities ranging from 4 to 7 on NRS with bending and lifting heavy objects as the major aggravating factors. The mean of total BPS score was 9.53 out of 15. It was observed that the performance was affected in roll-up, fingertip-to-floor, and lift test with the mean score of 2.23, 2.20, and 2.30, respectively. The mean scores and SDs of each BPS component are as given in Table 3.
| BPS components | n | Mean | SD | SEM |
|---|---|---|---|---|
| Sock test | 30 | 1.3000 | 0.74971 | 0.13688 |
| Pick-up test | 30 | 1.5000 | 0.62972 | 0.11497 |
| Roll-up test | 30 | 2.2333 | 0.67891 | 0.12395 |
| Fingertip-to-floor test | 30 | 2.2000 | 0.76112 | 0.13896 |
| Lift test | 30 | 2.3000 | 0.53498 | 0.09767 |
| Total BPS score | 30 | 9.5333 | 2.54251 | 0.46420 |
BPS: Back Performance Scale, SD: Standard deviation, SEM: Standard error of mean
Table 3: Mean scores of each Back Performance Scale component
In the two subscales of FABQ, 47% (14/30) participants had more fear in PA component and 27% (8/30) had more fear in work component.
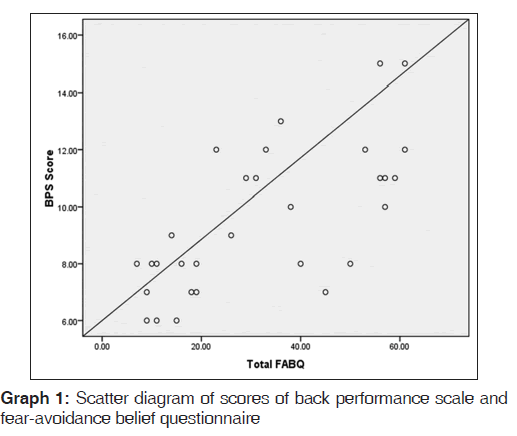
The scores of back performance and FABQ were correlated using Pearson’s correlation test which showed strong positive correlation (P < 0.01) with r value of 0.685 [Graph 1]. Further, each component of BPS was correlated with FABQ-PA and FABQ-W which showed significant association as given in Table 4.
| BPS tests | Mean | FABQPA | FABQW | ||
|---|---|---|---|---|---|
| r | P | r | P | ||
| Sock test | 1.3000 | 0.3649 | 0.05 | 0.4040 | 0.027 |
| Pick-up test | 1.5000 | 0.6282 | <0.00 | 0.6875 | 0.000 |
| Roll-up test | 2.2333 | 0.4546 | 0.01 | 0.5489 | 0.002 |
| Fingertip-to-floor test | 2.2000 | 0.5750 | <0.01 | 0.5752 | 0.001 |
| Lift test | 2.3000 | 0.3225 | 0.08 | 0.2328 | 0.217 |
| Total BPS score | 9.5300 | 0.6246 | <0.001 | 0.6572 | <0.001 |
Correlation significant P<0.01. FABQPA: Fear-Avoidance Belief Questionnaire-physical activity subscale, FABQW: Fear-Avoidance belief questionnaire-work subscale, BPS: Back performance scale
Table 4: Correlation of Back Performance Scale tests components with Fear-Avoidance Belief Questionnaire-physical activity subscale and Fear-Avoidance Belief Questionnaire-work subscale
Discussion
It was observed that CLBP limited physical performance of participants in this study. Physical performance was associated with pain and fear-avoidance behavior in roll-up, fingertip-to-floor, and lift test. The finger-to-floor test requires shoulder and hip movement in addition to body mobility. The roll-up test requires adopting a sitting position and is related to abdominal muscle strength which could reflect difficulty in performance if there is weakness in abdominal muscle strength. Flexibility and strength evaluation was not carried out as part of our study. The results obtained from the sock test and the pick-up performance test were similar to findings in previous literature. [18]
In the component analysis of FABQ, 47% participants had fear in performing FABQ-PA and 27% participants had fear while performing work at workplace (FABQ-W). Pain is an unpleasant subjective experience that has physiological and psychological components. Psychological factors are a “sequence of processes starting with initial awareness of a noxious stimulus; then, cognitive processing, appraisal, and interpretation that lead people to act on their pain (i.e., their pain behavior). These processes are influenced by their consequences and are limited by the environment (e.g., cultural and social values).” [19]
As rightly pointed out by Linton and Shaw, [20] interpretation of pain is a result of highly complex cognitive and emotional processing of noxious stimuli that shapes behavior. Interpretation is influenced by beliefs (e.g., negative - “pain is harmful”), attitude (e.g., passive - “the doctor will fix my pain”), expectations (e.g., fictitious - “going to work will hurt even more”), distorted cognition (e.g., catastrophizing - “I’ll end up in a wheelchair”), and emotional distress (e.g., depression - “life’s not worthy anymore”). [20]
In our study, the association of fear (FABQ) with lack of physical performance (BPS) showed strong positive correlation with R = 0.685. As the fear increases, the physical impairment is more and vice versa. The results of the current study are in line with investigations involving chronic pain patients. [15,21,22] Prior studies in a sample of individuals with an episode of acute LBP found pain-related fear to be a significant predictor of perceived (future) disability. Interpreting pain as harmful could lead a patient to avoid activity. The fear-avoidance model would suggest that fear of activity can create further development of chronic pain through a cycle of catastrophizing, depression, deconditioning, and disability.
Clinically, to improve the activities in CLBP patients, multidisciplinary approach including cognitive behavioral therapy and graded exposure to PA may be suggested. Researchers are studying various complementary and alternative therapies for LBP, including those aimed at reducing stress and negative emotions believed to aggravate the experience of pain. For example, virtual reality programs are being studied for their ability to help people cope with persistent pain. [23] Thus, clinicians should consider the significant role of psychological mechanisms (e.g., fear of pain and reinjury) when interpreting patient performance and PA. They should also be aware that fear-avoidance beliefs may reflect patients’ actual (nonexaggerated) experience with how best they handle their LBP.
Conclusion
This study concludes that a strong relationship exists between fear-avoidance beliefs and physical activities in patients with CLBP. It also indicates the importance of testing psychological aspects such as fear and avoidance of movement in CLBP patients.
Limitations
The study has been conducted in adult population with CLBP and the findings cannot be generalized to adults with acute LBP.
Acknowledgment
We would like to thank all the participants of our study.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Meucci RD, Fassa AG, Faria NM. Prevalence of chronic low back pain: Systematic review. Rev Saude Publica 2015;49. pii: S0034-89102015000100408.
- Duthey B. Priority Medicines for Europe and the World “A Public Health Approach to Innovation”Update on 2004, Background Paper, BP 6.24 Low Back Pain; 15 March, 2013. (http://www.who.int/medicines/areas/ priority_medicines/BP6_24LBP.pdf)
- Hoy D, Bain C, Williams G, March L, Brooks P, Blyth F, et al. A systematic review of the global prevalence of low back pain. Arthritis Rheum 2012;64:2028-37.
- International Classification of Functioning, Disability and Health: ICF. World Health Organization 2001. WHO Library Catalogue, page 14. (http://apps.who.int/iris/ bitstream/10665/42407/1/9241545429.pdf)
- Chou R. Pharmacological management of low back pain. Drugs 2010;70:387-402.
- Koley S, Singh G, Sandhu R. Severity of disability in elderly patients with low back pain in Amritsar, Punjab. Anthropologist 2008;10:265-8.
- Strand LI, Moe-Nilssen R, Ljunggren AE. Back Performance Scale for the assessment of mobility-related activities in people with back pain. Phys Ther 2002;82:1213-23.
- Skevington SM. Psychology of Pain. Chichester: Wiley; 1995.
- Gatchel RJ, Turk DC. Psychological approaches to pain management. A Practitioner’s Handbook. New York, London: Guildford Press; 1996.
- Swinkels-Meewisse IE, Roelofs J, Oostendorp RA, Verbeek AL, Vlaeyen JW. Acute low back pain: Pain-related fear and pain catastrophizing influence physical performance and perceived disability. Pain 2006;120:36-43.
- Fritz JM, George SZ. Identifying psychosocial variables in patients with acute work-related low back pain: The importance of fear-avoidance beliefs. Phys Ther 2002;82:973-83.
- Sieben JM, Vlaeyen JW, Tuerlinckx S, Portegijs PJ. Pain-related fear in acute low back pain: The first two weeks of a new episode. Eur J Pain 2002;6:229-37.
- Swinkels-Meewisse IE, Roelofs J, Verbeek AL, Oostendorp RA, Vlaeyen JW. Fear of movement/(re) injury, disability and participation in acute low back pain. Pain 2003;105:371-9.
- Waddell G, Newton M, Henderson I, Somerville D, Main CJ. A Fear-Avoidance Beliefs Questionnaire (FABQ) and the role of fear-avoidance beliefs in chronic low back pain and disability. Pain 1993;52:157-68.
- Al-Obaidi SM, Nelson RM, Al-Awadhi S, Al-Shuwaie N. The role of anticipation and fear of pain in the persistence of avoidance behavior in patients with chronic low back pain. Spine (Phila Pa 1976) 2000;25:1126-31.
- Geisser ME, Haig AJ, Theisen ME. Activity avoidance and function in persons with chronic back pain. J Occup Rehabil 2000;10:215-27.
- Fritz JM, George SZ, Delitto A. The role of fear-avoidance beliefs in acute low back pain: Relationships with current and future disability and work status. Pain 2001;94:7-15.
- Teixeira da Cunha-Filho I, Lima FC, Guimarães FR, Leite HR. Use of physical performance tests in a group of Brazilian Portuguese-speaking individuals with low back pain. Physiother Theory Pract 2010;26:49-55.
- Banerjee G, Bostick GP. Nonspecific non-acute low back pain and psychological interventions: A review of evidence and current strategies. Indian J Pain 2015;29:21.
- Linton SJ, Shaw WS. Impact of psychological factors in the experience of pain. Phys Ther 2011;91:700-11.
- Heuts PH, Vlaeyen JW, Roelofs J, de Bie RA, Aretz K, van Weel C, et al. Pain-related fear and daily functioning in patients with osteoarthritis. Pain 2004;110:228-35.
- Peters ML, Vlaeyen JW, Weber WE. The joint contribution of physical pathology, pain-related fear and catastrophizing to chronic back pain disability. Pain 2005;113:45-50.
- Bethesda, Maryland, United States: National Institutes of Neurological Disorder and Stroke [NINDS], National Institutes of Health [NIH]; 1950. (https://www.ninds.nih. gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/ Low-Back-Pain-Fact-Sheet, accessed on 15th July 2015)




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.