Association of Vitamin D Levels with Blood Pressure in Dialysis Patients in a Dialysis Centre in Tehran
2 Research Institute for Endocrine Sciences, AJA University of Medical Sciences, Tehran, Iran, Email: o_gh_79@yahoo.com
3 Research Institute for Endocrine Sciences, Shahid Beheshti University of Medical Sciences, Tehran, Iran, Email: shahnaz442@yahoo.com
4 Department of Nephrology, Loghman Hakim Hospital, Clinical Research Development Center, Tehran, Iran
Citation: Tofangchiha S, et al. Association of Vitamin D Levels with Blood Pressure in Dialysis Patients in a Dialysis Centre in Tehran. Ann Med Health Sci Res. 2018;8:239-243
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Introduction: Prevalence of vitamin D deficiency among patients with kidney failure is about 70 to 80 percent. Among the main controversies in the field of patients with kidney failure is the relationship between vitamin D deficiency and prevalence and natural course of hypertension. Many studies have been conducted on the relationship between vitamin D levels and hypertension, but they have mostly been inconclusive and have generated inconsistent results. Materials and methods: This cross-sectional study was conducted on 120 patients with dialysis in three dialysis centers in Tehran, Iran. Vitamin D levels were measured by dialysis centers every three months for a year. Also, the centers recorded blood pressure after each dialysis session. These measurements were collected and their means for each patient were calculated and analyzed by backward multivariate linear regression in order to determine the association between blood pressure and levels of vitamin D. Besides, during the study, data on other confounding factors such as age, sex, weight, and so on were gathered. Levels of calcium, phosphorus, and PTH were also measured. A previously prepared checklist was used by the nurses in order to record patient data. Results: In this cross-sectional study, 101 dialysis patients were assessed, of which 45 were female and 56 were male. The mean age of the patients was 60 years. 55.6% of the patients had vitamin D deficiency (vitamin D <30 ng/ml). After entering and analyzing data, the serum level of vitamin D had a significant association with diastolic blood pressure, and Pearson correlation coefficient between diastolic blood pressure and serum levels of vitamin D was statistically significant (p<0.002). Conclusion: In this observational study, a significant linear association was found between serum levels of vitamin D and diastolic blood pressure in patients with dialysis. It seems that vitamin D levels had a negative association with diastolic blood pressure in those patients.
Keywords
Vitamin D; Diastolic blood pressure; Dialysis
Introduction
Cardiovascular complications are the most common cause of death in dialysis patients. The most important cardiovascular complication in this group of patients is hypertension. [1] A cohort study on 2535 dialysis patients from United States revealed that the prevalence of hypertension was 86%, and despite using anti-hypertensive medications by 76% of patients, the rate of controlled-hypertension in this study was only 30%. [2] Although there is no accurate record on the prevalence of hypertension among Iranian dialysis patients, considering this remarkable evidence from the United States population, it is expected that hypertension contributes significantly too among dialysis patients in the Iranian population. Therefore, more detailed knowledge of the factors related to controlling blood pressure among dialysis patients in Iran is urgently needed.
One of these factors that have been raised in the last decade is the concentration of vitamin D in dialysis patients. More than one billion people in the world have vitamin D deficiency [3] and the prevalence of vitamin D deficiency among patients with kidney failure is about 70 to 80 percent. [4,5] Although there are no strict national figures regarding this issue in Iran, the present literature suggest that this country is no exception and that vitamin D deficiency is a serious health challenge in Iran. Many studies have been conducted on the relationship between vitamin D levels and hypertension, but they have mostly been inconclusive and have generated inconsistent results.
In this regard, in the study conducted by Lu Wang et al. in 2008 on 28886 women aged over 45 years, there was a negative correlation between vitamin D levels and hypertension. [6] Similar results have been found between low levels of vitamin D and high blood pressure in a meta-analysis study conducted by Anand Vaidya et al. [7] However; in study by Kashani et al. which assessed 251 Tehranian adults could not find any relationship between levels of vitamin D and hypertension. [8] Besides, McMullan et al. in 2017 observed that vitamin D modification could not improve hypertension control among 84 patients. [9] Due to above-mentioned controversy, as well as the lack of sufficient evidence in Iranian population, we aimed to assess the association of vitamin D levels with hypertension among patients with dialysis.
Materials and Methods
This cross-sectional study was conducted on 120 patients with dialysis in three dialysis centers in Tehran. Patients were included in the study whose renal failure was confirmed and had been dialyzed for at least three months at the time of assessment. The study was observational and no intervention in the treatment or prescribed vitamin D supplementation was performed. Vitamin D levels that were measured by dialysis centers every three months for a year by a kit provided by an Immunodiagnostics kit Monobind Co., Tehran, Iran. As Also, the centers recorded blood pressure after each dialysis session was collected and their means for each patient were calculated and analyzed by the SPSS Software, version 25. To determine the regression equation for prediction of diastolic blood pressure, backward multivariate linear regression was used. This test was performed in 7 steps, and the variables that remained after the 7th step were included in the results.
Besides, during the study, data on other confounding factors such as age, sex, weight, and so on were gathered by dialysis nurses. Levels of calcium, phosphorus (Bionic Co, Tehran, Iran), and PTH (ECL kit provided by Akbarieh Co., Tehran, Iran) were also measured. In order to standardize and minimize the variation between centers, the same make and model of the digital device was used to record blood pressure. All blood tests were performed by Loghman Hospital laboratory. A previously prepared checklist was used by the nurses in order to record patient data (Appendix 1). Patients who had the following criteria were excluded from the study:
• Patients who did not have compliance with medication and did not use the anti-hypertensive drug regularly.
• Patients who did not undergo dialysis regularly (less than 3 times per week) or did not have adequate dialysis, and were clinically edematous even post-dialysis.
• Patients who were admitted to hospital during the study due to the manifestation of disease including, but not limited to, cardiovascular events and infections.
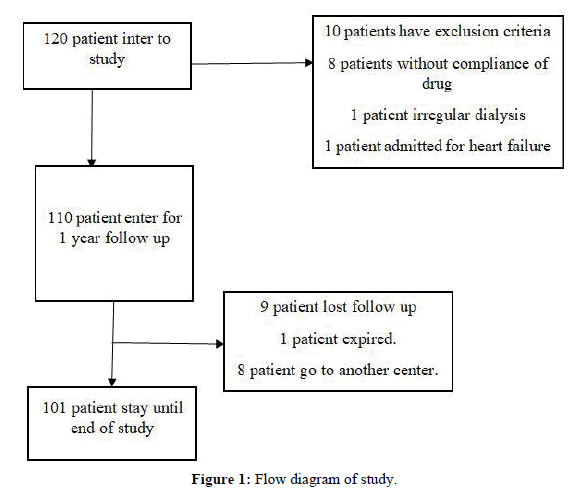
• After one year of follow-up, out of 120 patients ultimately 101 individuals remained and were included in the final analysis [Figure 1].
Results
In this cross-sectional study, 101 dialysis patients were assessed, of which 45 were female and 56 were male. The mean age of the patients was 60 years. The mean and standard deviation of measured variables are shown in Table 1. 55.6% of the patients had vitamin D deficiency (vitamin D <30 ng/ml). After entering and analyzing data, the serum level of vitamin D had a significant association with diastolic blood pressure, and Pearson correlation coefficient between diastolic blood pressure and serum levels of vitamin D was statistically significant (p<0.002).
| Variables | Systolic blood pressure |
Diastolic blood pressure | weight | Age | Vitamin D level | Weight gain between two dialysis sessions | Ca | P | PTH |
|---|---|---|---|---|---|---|---|---|---|
| Valid | 101 | 101 | 100 | 101 | 99 | 100 | 101 | 93 | 99 |
| Missing | 0 | 0 | 1 | 0 | 2 | 1 | 0 | 8 | 2 |
| Mean | 120.6 | 80.2 | 69 | 60.2 | 30.8 | 3.4 | 8.7 | 4.8 | 527.2 |
| Std. Deviation | 17.2 | 14.3 | 14.1 | 14.3 | 20.4 | 11.4 | 0.9 | 0.9 | 489.7 |
| Minimum | 80 | 50 | 32 | 19 | 4.5 | .0 | 6.2 | 2.7 | 12.5 |
| Maximum | 170 | 120 | 110 | 84 | 126.0 | 117 | 11.2 | 7.8 | 2020.0 |
Table 1: Mean and standard deviation of variables.
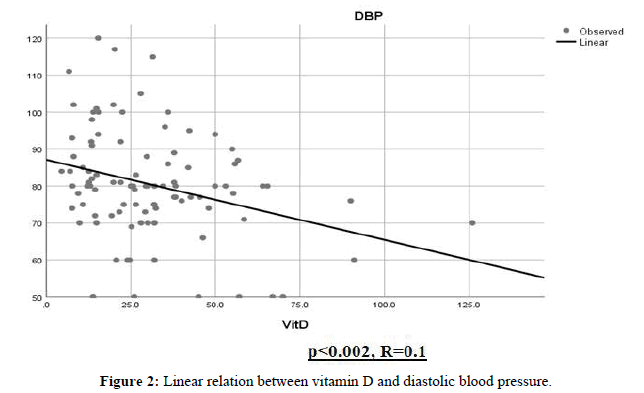
To determine the relationship between diastolic blood pressure and vitamin D levels, backward multivariate linear regression was used as mentioned in the methods section. After the 7th step of the regression model, vitamin D was the only variable that had a statistical significance. In all seven steps, the whole model had statistical validation (p<0.05).Variables such as weight in step 2, age in step 3, calcium in step 4, PTH in step 5, weight gain between dialysis in step 6, and phosphorus in step 7 were not statistically analyzed due to meaningfulness. The relationship between the level of vitamin D and diastolic blood pressure is presented in Figure 2.
Discussion
Over 25 years, biological mechanisms have investigated the relationship between vitamin D deficiency and blood pressure, and it has shown that vitamin D, through the renin-angiotensin system, could affect intracellular calcium in the smooth muscle of the ventricular septum. [7] More than 20 large cross-sectional studies have been conducted on the association of serum vitamin D levels with blood pressure and most of them have indicated that low levels of vitamin D are associated with high blood pressure. [9-11] However, two major studies have not been able to find an association between vitamin D levels and risk of high blood pressure. Some cohort studies presented similar results and showed that the blood pressure in patients with vitamin D levels >30 was lower than in those with vitamin D levels <15. [12]
However, contrary to the observational studies, clinical controlled trials were not able to show the desirable effect of vitamin D intervention on reducing the blood pressure. A summary of these studies are presented in the following Table 2. [13-25] Despite vitamin D supplementation, most of these studies was not able to achieve enough vitamin D levels and did not measure the change in vitamin D status. However, it is possible that vitamin D deficiency is a sign of an underlying disorder leading to, rather than a direct “cause” of, high DBP. Consistent with this, even a meta-analysis that included 9 to 12 studies mentioned in Table 2 could not prove the therapeutic effect of vitamin D on hypertension. [26]
| Study | N | Dose | Duration | Baseline 25(OH)D | Change in 25(OH)D | Effect on Blood Pressure |
|---|---|---|---|---|---|---|
| Orwoll et al. [13] | 65 | 1000 IU/d | 3 y | Not given | Not given | Null |
| Pan et al. [14] | 58 | 200 IU/d | 11 wk | 24 ng/mL | Not given | Null |
| Scragg et al. [15] | 189 | 100 000 IUX1 | 5 wk | 13 ng/mL | 7 ng/mL | Null |
| Pfeifer et al. [16] | 148 | 800 IU/d | 8 wk | 10 ng/mL | 12 ng/mL | Decrease |
| Schleithoff et al. [17] | 93 | 10 000 IU/d | 15 mo | 15 ng/mL | 27 ng/mL | Null |
| Major et al. [18] | 63 | 400 IU/d | 15 wk | Not given | Not given | Null |
| Sugden et al. [19] | 34 | 100 000 IUX1 | 8 wk | 15 ng/mL | 9 ng/mL | Decrease |
| Margolis et al. [20] | 36 282 | 400 IU/d | 7 y | 19 ng/mL | Not given | Null |
| Zittermann et al. [21] | 165 | 16 600 IU/d | 1 y | 12 ng/mL | 22 ng/mL | Null |
| Daly et al. [22] | 140 | 800 IU/d | 2 y | Not given | Not given | Null |
| Jorde et al. [23] | 32 | 40 000 IU/wX24 | 6 mo | 24 ng/mL | 23 ng/mL | Null |
| Nagpal et al. [24] | 71 | 120 000 IUX3 | 6 wk | 13 ng/mL | 14 ng/mL | Null |
| Jorde et al. [25] | 438 | 20 000 or 40 000/w | 1 y | 23 ng/mL | 17–32 ng/mL | Null |
Table 2: Summary of clinical trial.
Despite the controversy among observational and interventional studies on the relationship between vitamin D and blood pressure, studies in this area are very limited in Iran. One comprehensive study performed at Shahid Beheshti University of Medical Sciences in 2003 showed that, contrary to other studies, there was no relationship between serum vitamin D levels and hypertension in people aged >40 years who live in the eastern part of Tehran. [8]
Regarding the association of vitamin D levels with hypertension in patients with renal failure, the evidence is even less. Given the high prevalence of hypertension in patients with dialysis and presence of other risk factors for hypertension in these patients, elucidating the potential effects of a variable such as vitamin D on the pathogenesis of hypertension will be significantly more challenging. [27]
Initially, it seems that because of impaired activity of 1-alphahydroxylase in kidney of patients with renal failure, prescription of 25-hydroxy vitamin D is not required when the active form of vitamin D is used. While, the 1-alpha-hydroxylase enzyme is also found outside the kidney and its activity is preserved even in non-renal patients. [28] In addition, the beneficial effects of vitamin D on dialysis patients have been described in recent years. For instance, vitamin D levels in dialysis patients were associated with muscle strength. [29] It has also been observed that serum levels of 25-hydroxy vitamin D are predictors of mortality in patients with chronic kidney disease, so that some studies have recommended maintaining a level of vitamin D of 40 to 80 ng/ml instead of 30 ng/ml. [30,31] Besides, it has been proven in clinical studies that oral vitamin D supplementation is safe in hemodialysis patients and does not significantly alter serum concentration of calcium, phosphorus and parathyroid hormone. [32]
In our study, more than 50% of dialysis patients suffered from vitamin D deficiency; according to previous studies, this prevalence was not too far from expectation. Also a significant relationship between vitamin D and diastolic blood pressure was detected. Although, as expected, due to the limitations of observational studies, the contribution of the ability to predict diastolic blood pressure in the linear regression equation for vitamin D is not significant, and this might be because of the lack of including moderator confounding factors for analysis. Similar to the Ishir Bayhan et al. and Tehran Study, the current study found no significant correlation between vitamin D, calcium, phosphorus, and PTH and similar to Tehran Study, we did not find any significant correlation between calcium, phosphorus, and PTH levels with systolic or diastolic blood pressure. The inconsistency in the results of observational studies on the association of vitamin D levels and blood pressure can be attributed to several factors. For example, in the Tehran Study [8] the definition of vitamin D deficiency was >20 ng/ml, which is different to our study and another study with similar finding, or in the Amsterdam study [33] one third of patients were taking anti-hypertensive drugs, which can hide the effects of vitamin D. However, taking anti-hypertensive medications among patients with vitamin D levels > 30 ng/ml were 33% less likely compared to those with vitamin D > 10. In addition, in the study by Raco-Bernardo et al. conducted in Southern California, 98% of the population had normal levels of vitamin D. [34]
Therefore, considering these limitations, it can be concluded that in most observational studies, including ours, there is a significant relationship between the levels of vitamin D and blood pressure.
Conclusion
In this observational study, a significant linear association was found between serum levels of vitamin D and diastolic blood pressure in patients with dialysis. It seems that vitamin D levels had a negative association with diastolic blood pressure in those patients.
Limitations
Although we have tried to adjust confounding factors through following patients for one year, choosing more patients under analysis, and removing unstable patients, the nature of this observational study may have led to some limitation, and we would not be able to consider all of the confounders during the study. As a result, the contribution of the regression equation to predict diastolic blood pressure was low.
Conflict of Interest
The authors disclose that they have no conflicts of interest.
REFERENCES
- Foley RN, Herzog CA, Collins AJ. Blood pressure and long-term mortality in United States hemodialysis patients: USRDS Waves 3 and 4 Study. Kidney Int. 2002;62 :1784-1790.
- Agarwal R, Nissenson AR, Batlle D, Coyne DW, Trout JR, Warnock DG. Prevalence, treatment, and control of hypertension in chronic hemodialysis patients in the United States. Am J Med. 2005;115:291-297.
- Holick MF. Vitamin D deficiency. N Engl J Med. 2007;357:266-281.
- LaClair RE, Hellman RN, Karp SL, Kraus M, Ofner S, Li Q, et al. Prevalence of calcidiol deficiency in CKD: A cross-sectional study across latitudes in the United States. Am J Kidney Dis. 2005;45:1026-1033.
- Bhan I, Burnett-Bowie SA, Ye J, Tonelli M, Thadhani R. Clinical measures identify vitamin D Deficiency in dialysis. Clin J Am Soc Nephrol. 2010;5:460-467.
- Wang L, Manson JE, Buring JE, Lee IM, Sesso HD. Dietary intake of dairy products, calcium, and vitamin D and the risk of hypertension in middle-aged and older women. Hypertension. 2008;51:1073-1079.
- Vaidya A, Forman JP. Vitamin D and hypertension current evidence and future directions. Hypertension. 2010;56:774-779.
- Kashi Z, Mirmiran P, Mehrabi Y, Hedayati M, Azizi F. Association of blood pressure, serum vitamin D, calcium and PTH in individuals over 40 in East Tehran. 2003;5:261-270.
- Scragg R, Sowers M, Bell C. Serum 25-hydroxyvitamin D, ethnicity, and blood pressure in the Third National Health and Nutrition Examination Survey. Am J Hypertens. 2007;20:713-719.
- Hintzpeter B, Mensink GB, Thierfelder W, Muller MJ, Scheidt-Nave C. Vitamin D status and health correlates among German adults. Eur J Clin Nutr. 2008;62:1079 -1089.
- Hypponen E, Boucher BJ, Berry DJ, Power C. 25-Hydroxyvitamin D, IGF-1, and metabolic syndrome at 45 years of age: A cross-sectional study in the 1958 British Birth Cohort. Diabetes. 2008;57:298-305.
- Forman JP, Giovannucci E, Holmes MD, Bischoff-Ferrari HA, Tworoger SS, Willett WC, et al. Plasma 25-hydroxyvitamin D levels and risk of incident hypertension. Hypertension. 2007;49:1063-1069.
- Orwoll ES, Oviatt S. Relationship of mineral metabolism and long-term calcium and cholecalciferol supplementation to blood pressure in normotensive men. Am J Clin Nutr. 1990;52:717-721.
- Pan WH, Wang CY, Li LA, Kao LS, Yeh SH. No significant effect of calcium and vitamin D supplementation on blood pressure and calcium metabolism in elderly Chinese. Chin J Physiol. 1993;36:85-94.
- Witham MD, Nadir MA, Struthers AD. Effect of vitamin D on blood pressure: a systematic review and meta-analysis. J Hypertens. 2009;27:1948-1954.
- Pfeifer M, Begerow B, Minne HW, Nachtigall D, Hansen C. Effects of a short-term vitamin D(3) and calcium supplementation on blood pressure and parathyroid hormone levels in elderly women. J Clin Endocrinol Metab. 2001;86:1633-1637.
- Schleithoff SS, Zittermann A, Tenderich G, Berthold HK, Stehle P, Koerfer R. Vitamin D supplementation improves cytokine profiles in patients with congestive heart failure: a double-blind, randomized, placebo-controlled trial. Am J Clin Nutr. 2006;83:754-759.
- Major GC, Alarie F, Dore J, Phouttama S, Tremblay A. Supplementation with calcium _ vitamin D enhances the beneficial effect of weight loss on plasma lipid and lipoprotein concentrations. Am J Clin Nutr. 2007;85:54-59.
- Sugden JA, Davies JI, Witham MD, Morris AD, Struthers AD. Vitamin D improves endothelial function in patients with type 2 diabetes mellitus and low vitamin D levels. Diabet Med. 2008;25:320-325.
- Margolis KL, Ray RM, Van Horn L, Manson JE, Allison MA, Black HR, et al. Effect of calcium and vitamin D supplementation on blood pressure: The Women’s Health Initiative Randomized Trial. Hypertension. 2008;52:847-855.
- Zittermann A, Frisch S, Berthold HK, Gotting C, Kuhn J, Kleesiek K, et al. Vitamin D supplementation enhances the beneficial effects of weight loss on cardiovascular disease risk markers. Am J Clin Nutr. 2009;89:1321-1327.
- Daly RM, Nowson CA. Long-term effect of calcium-vitamin D(3) fortified milk on blood pressure and serum lipid concentrations in healthy older men. Eur J Clin Nutr. 2009;63:993-1000.
- Jorde R, Figenschau Y. Supplementation with cholecalciferol does not improve glycaemic control in diabetic subjects with normal serum 25-hydroxyvitamin D levels. Eur J Nutr. 2009;48:349-354.
- Nagpal J, Pande JN, Bhartia A. A double-blind, randomized, placebocontrolled trial of the short-term effect of vitamin D3 supplementation on insulin sensitivity in apparently healthy, middle-aged, centrally obese men. Diabet Med. 2009;26:19-27.
- Jorde R, Figenschau Y, Emaus N, Hutchinson M, Grimnes G. Serum 25-hydroxyvitamin D levels are strongly related to systolic blood pressure but do not predict future hypertension. Hypertension. 2010;55:792-798.
- Pittas AG, Chung M, Trikalinos T, Mitri J, Brendel M, Patel K, et al. Systematic review: vitamin D and cardiometabolic outcomes. Ann Intern Med.152:307-314.
- Zahed NS, Gharooi O, Gachkar L, Nikbakht H. The evaluation of relationship between blood pressure and dialysate Na concentration in chronic hemodialysis patients. J Renal Inj Prev. 2016;5:118-122.
- Williams S, Malatesta K, Norris K. Vitamin D and chronic kidney disease. Ethn Dis. 2009;19:S5-S11.
- Zahed N, Chehrazi S, Falaknasi K. The evaluation of relationship between Vitamin D and muscle power by micro manual muscle tester in end-stage renal disease patients. Saudi J Kidney Dis Transpl. 2014;25:998-1003.
- Jones G. Expanding role of vitamin D in chronic kidney disease: Importance of blood 25-OH-D levels and extra-renal 1a-hydroxylase in the classical and nonclassical actions of 1a,25-dihydroxy vitamin D3. Seminars in Dialysis. 2007;20:316-324.
- Heaney RP. Vitamin D in health and disease. Clin J Am Soc Nephrol. 2008;3:1535-1541.
- Bhan I, Dobens D, Tamez H, Deferio JJ, Li, YC, Warren HS. Nutritional Vitamin D Supplementation in Dialysis: A Randomized Trial. Clin J Am Soc Nephrol. 2015;10:611-619.
- Reis JP, von Muhlen D, Kritz-Silverstein D, Wingard DL, Barrett-Connor E. Vitamin D, parathyroid hormone levels, and the prevalence of metabolic syndrome in community-dwelling older adults. Diabetes Care. 2007;30:1549-1555.
- Snijder MB, Lips P, Seidell JC, Visser M, Deeg DJ, Dekker JM, et al. Vitamin D status and parathyroid hormone levels in relation to blood pressure: a population-based study in older men and women. J Intern Med. 2007;261:558-565.




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.