Comparative Evaluation of Classical Inferior Dental Nerve Block and Gow-Gates Mandibular Nerve Block for Posterior Dentoalveolar Surgery : A prospective study and literature review
2 Department of Oral & Maxillofacial Surgery, Career Post Graduate Institute of Dental Sciences and Hospital, Lucknow Uttar Pradesh, India
3 Department of oral and maxillofacial surgery, Inderprastha dental College & hospital, Sahibabad, Ghaziabad, Uttar Pradesh, India, Email: drdeepakpassi@gmail.com
4 Department of Dentistry, Government Medical College, Kannauj, Uttar Pradesh, India
5 Departmemt of Dentistry, Hind Institute of Medical Sciences, Sitapur, Uttar Pradesh, India
6 Departmemt of Dentistry, Major S.D. Singh Medical College & Hospital, Farrukhabad, Uttar Pradesh, India
7 Department of oral and maxillofacial surgery, ESI Dental college and hospital, Rohini, Delhi, India
8 Department of Oral Pathology, GDCH Aurangabad, Aurangabad, Maharashtra, India
Citation: Dubey M, et al. Comparative Evaluation of Classical Inferior Dental Nerve Block and Gow-Gates Mandibular Nerve Block for Posterior Dentoalveolar Surgery : A prospective study and literature review. Ann Med Health Sci Res. 2017; 7: 92-96
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Aim & Objective: This study aimed to evaluate the efficacy of anesthesia obtained with a Classical inferior dental nerve block compared with the Gow-Gates mandibular nerve block for posterior dentoalveolar surgical procedures. Material & Methods: 100 Patients requiring mandibular posterior dentoalveolar surgical procedure under local anesthesia were randomly selected from the outpatient department. These patients were divided equally into two groups of 50 each with age range of 18 to 56 years. In group A, local anesthetic solution administered by standard technique to achieve mandibular anesthesia while in group B the Gow-Gate technique was used. The statistical analysis was done using SPSS (Statistical Package for Social Sciences) Version 15.0 statistical Analysis Software. The values were represented in Number (%) and Mean ± SD. Result: The patients in group B showed no complications during or after injection, time of onset on anesthesia and complete recovery from anesthesia were found more in group B. Most of the patients were highly satisfied with Gow-Gates nerve block. Conclusion: Gow- Gates technique is superior to inferior alveolar nerve block . It requires expertise and higher skill which one develops with practise.
Keywords
Inferior dental nerve block; Gow-Gates mandibular nerve block; Onset of anesthesia; Duration of anesthesia; Recovery from anesthesia
Introduction
Perception of pain is a subjective experience that can only be ascertained by the individual experiencing the sensation or direct physical examination. pain threshold is more dependent on physiological factors and pain tolerance on psychological factors. Traditionally, the inferior alveolar nerve block, also known as the standard mandibular nerve block/ Halsted block has been used to provide anesthesia for mandibular posterior teeth. The Gow-Gates mandibular block technique is a concept introduced by George AE Gow- Gate. [1] to intercept sensory conduction in the mandible. All oral branches of the mandibular nerve are blocked by depositing an adequate volume of anesthetic solution in only one position away from the proximity of nerve membranes. The present study was conducted in an endeavour to achieve anesthesia of mandibular tissues for posterior dentoalveolar surgical procedures by using either of the two techniques, standard technique and Gow-Gates technique and to correlate the results.
Materials and Methods
Hundred Patients requiring mandibular posterior dentoalveolar surgical procedure under local anesthesia were randomly selected . These patients were divided equally into two groups of 50 each with age range of 18 to 56 years. In group A, local anesthetic solution administered by standard technique to achieve mandibular anesthesia while in group B the Gow- Gate technique was used. Patient’s having 35 mm or above maximum inter-incisal mouth opening was selected for the study. Medically compromised patients, patients allergic to local anesthetic solution and those having localized infection at injection site were excluded from the study. The present study was conducted after the approval by ethical committee of Career Post Graduate Institute of Dental Sciences and Hospital, Lucknow (U.P). Prior to the administration of nerve block and any surgical procedure all subjects signed a consent form explaining the experimental procedures and all possible risk in Hindi / English language.
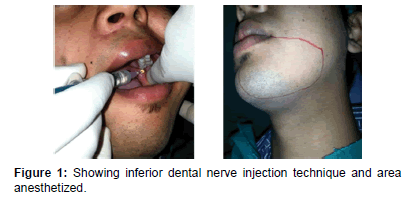
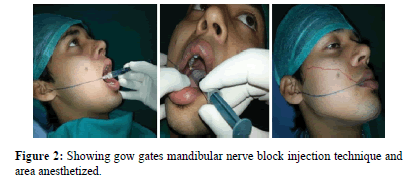
The anesthetic solution used for injection was 1.8 ml of a 2% lignocaine hydrochloride solution with 1: 80,000 epinephrine. The solution was injected through 25 gauges, sterile long disposable needle (38 mm) with a endodontic file stopper mounted on a 3 ml conventional disposable syringe. Prior to injection all the patients had preoperative mouth risne with povidine iodine solution. Each injection site was dried with a gauze wipe and no topical anesthetic agent was used prior to injection [Figures 1 and 2].
Following aspiration in two planes classical inferior dental nerve block was given in group A while in group B Gow Gates nerve block was given. 5-10 minutes after administration of local anesthetic solution subjective and objective symptoms were cheked for the effectiveness of the block.
Results
Out of 100 patients enrolled in the study, 50 patients were given classical inferior dental nerve block while remaining 50 were given Gow-Gates mandibular nerve block for posterior dentoalveolar surgery.
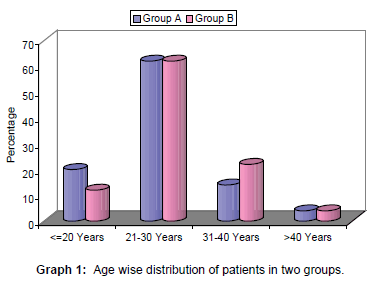
In present study age of patients ranged from 18 to 56 years. Majority of patients in both the groups were aged 21-30 years. Mean age of patients in group A was 26.08 ± 7.36 years as compared to 28.16 ± 5.72 years in group B. Statistically, the difference in mean age between two groups was not significant (p=0.596) [Table 1 and Graph 1].
| Age Group (Years) | Group A (n=50) | Group B (n=50) | ||
|---|---|---|---|---|
| No. | % | No. | % | |
| <20 | 10 | 20 | 6 | 12 |
| 21-30 | 31 | 62 | 31 | 62 |
| 31-40 | 7 | 14 | 11 | 22 |
| >40 | 2 | 4 | 2 | 4 |
| Mean Age ± SD (Range) | 26.08 ± 7.36 (18-56) | 28.16 ± 5.72 (20-48) | ||
Table 1: Age wise distribution of patients in two groups.
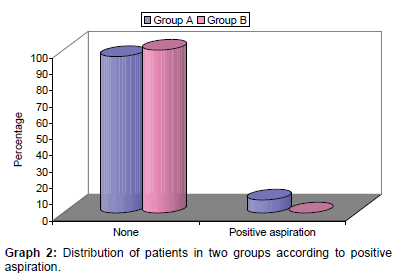
Positive aspiration was observed in 4 (8%) cases of group A while none in group B. The block was ineffective in 1st attempt in 2 patients of group A while in group B it was ineffective in 11 patients hence required repetition of respective blocks. Hence anesthetic need was 3.6 ml in 2 (4%) of group A and 11 (22%) of group B patients while others required 1.8 ml of solution. This difference between groups was statistically significant (p=0.004) [Table 2 and Graph 2].
| Complications | Group A (n=50) | Group B (n=50) | ||
|---|---|---|---|---|
| No. | % | No. | % | |
| Absent | 46 | 92 | 50 | 100 |
| Present | 4 | 8 | 0 | 0 |
Table 2: Distribution of patients in two groups according to positive aspiration.
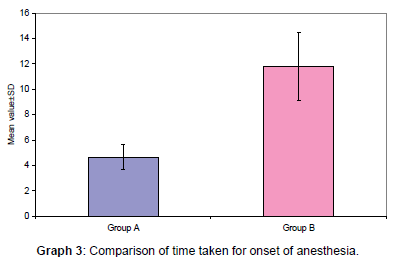
Mean time taken for onset of anesthesia was 4.65 ± 0.98 min in group A as compared to 11.82 ± 2.68 in group B. Statistically, this difference was significant (p<0.001) [Table 3 and Graph 3].
| Parameters | Group A (n=50) | Group B (n=50) |
|---|---|---|
| Mean | 4.65 | 11.82 |
| SD | 0.98 | 2.68 |
| Minimum | 3.00 | 8.00 |
| Max | 6.50 | 18.17 |
Table 3: Comparison of time taken for onset of anesthesia.
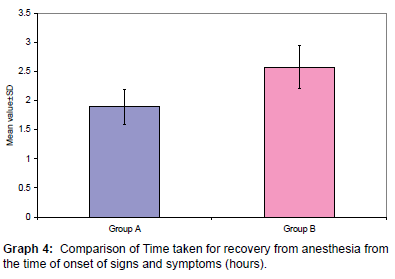
Time taken for recovery was calculated from the time of onset of anaesthesia to complete wear off both subjectively and objectively ranged from 1.00 to 3.42 hrs. Mean time taken was 1.8 ± 0.30 hrs in group A as compared to 2.57 ± 0.37 hours in group B and was found to be statistically significant (p<0.001) [Table 4 and Graph 4].
| Parameters | Group A (n=50) | Group B (n=50) |
|---|---|---|
| Mean | 1.89 | 2.57 |
| SD | 0.30 | 0.37 |
| Minimum | 1.00 | 2.00 |
| Max | 2.33 | 3.42 |
Table 4: Comparison of Time taken for recovery from anesthesia from the time of onset of signs and symptoms (hours).
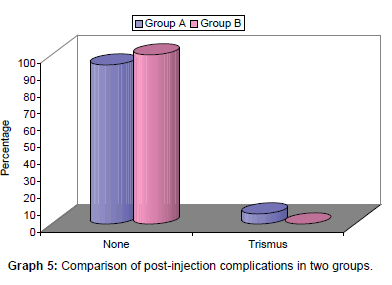
No complication was observed in group B, however, in group A, 3 (6%) cases had trismus. Majority of patients in both the groups were satisfied or highly satisfied. Statistically, the difference between two groups was not significant (p=0.124) [Table 5 and Graph 5].
| Findings | Group A (n=50) | Group B (n=50) | ||
|---|---|---|---|---|
| No. | % | No. | % | |
| None | 47 | 94 | 50 | 100 |
| Trismus | 3 | 6 | 0 | 0 |
Table 5:Comparison of post-injection complications in two groups.
The statistical analysis was done using SPSS (Statistical Package for Social Sciences) Version 15.0 statistical Analysis Software. The values were represented in Number (%) and Mean ± SD.
Discussion
2% lignocaine hydrochloride with 1:80,000 epinephrine is a standard solution which has been used over a long period of time for achieving adequate local anesthesia. In this present study for each injection 1.8 ml of 2% Lignocaine hydrochloride with 1: 80,000 epinephrine of Warren pharmaceuticals were used in both the groups. Lignocaine hydrochloride to a certain extent possess vasodilating property resulting in rapid uptake of drug from the local site thereby reducing the duration of anesthesia. Addition of 1:80,000 adrenaline increases the properties which are desired for proper anesthesia (depth and duration of anesthesia) and shortens the time of onset.
In present study 1.8 ml 2% lignocaine with 1:80,000 adrenaline provided adequate anesthesia in 48 cases of group A as compared to 39 cases in group B. In our opinion the requirement of repetition of injection was due to non-deposition of solution at the correct site rather than the amount of the local anesthetic solution. This can be attributed to the fact that Gow Gates is more technique sensitive and its anatomical landmarks being soft tissue only and are subjected to variation. Local anesthetic agent is supposed to be delivered in the proximity of the nerve and retained there for the duration of the procedure. Since the delivering of the anesthetic solution in the proximity of the nerve is a blind procedure and nerve & vessels lie together in the form of neurovascular bundle, Possibilities of inadvertent intravascular delivery of local anesthetic is always there. Delivering of local anesthetic inside the blood vessel results in the systemic side effects and failure of anesthesia as not enough local anesthetic is available to act on the nerve. In Gow-Gate technique the vascular areas located near the site of injection include the internal maxillary artery and pterygoid plexus of vein. If the needle is placed at the recommended spot in contact of neck of the condyle and then only the solution is deposited, the possibilities of inadvertent intravascular injection can be completely eliminated. Using a 38 mm long needle with correct technique and two plane aspiration resulted in no case of positive aspiration signifying no intravascular placement while 4 (8%) cases produced positive aspiration in Group A (classical inferior dental nerve block technique),well supported by Daniel A Haas [2]
Inferior alveolar neurovascular bundle enters into the mandibular foramen and a bony projection called lingula is the nearby bony landmark in inferior dental nerve block. Inadvertent penetration into inferior alveolar vessels during injection is the cause of positive aspiration in inferior dental technique. In our study no case of positive aspiration was found in Group B owing to needle placement site 1 to 2 mm anteriomedial part of condylar neck below the insertion of lateral pterygoid muscle which is relatively avascular area. According to the findings of Fanyuan Yu et al. [3] they found lower rate of positive aspiration in Gow- Gate technique as compared to Inferior dental technique. Hence likelihood of vascular accidents is lesser. Animesh Barodiya et al. [4] reported positive aspiration in the Gow-Gate technique and explained it to be due to puncturing of the internal maxillary or middle meningeal artery. The rate of positive aspiration for standard technique was found to be 10-15%. Abbas Haghighat et al. [5] stated in his clinical study of comparison of success rate and onset time of two different anesthesia techniques found that the onset of anesthesia depends on closeness of approximation of the nerve blocking drugs to the related nerve trunk. The numbness of lower lip was regarded as the onset of anesthesia in this study. Mean time taken for onset of anesthesia was 4-5 minute in Group A, while in Group B was 11-13 minutes which was statistically significant. There can be two reasons for longer time of onset in Gow Gates technique. Firstly, greater the diameter of mandibular nerve as compared to inferior alveolar nerve which requires longer time for local anesthetic to penetrate and reach the core fibres. Secondly, moreover additional time of approximately 60 secs is required as advocated by the Gow Gates, during which the patient is asked to keep his mouth wide open. This allows anesthetic solution to percolate down in response to gravity which causes larger cross section of nerve trunk to be bathed in local anesthetic solution within the confines of inter pterygoid facial pouch. This is further assisted by the anatomic outline surrounding the point of deposition of solution as it is bounded laterally by tendon of temporalis, medially by medial pterygoid amd superiorly by lateral pterygoid. This was supported by the assessment of Stanley F Malamed et al. [6]
Pei-Chuan Hung et al. [7] in their study for the comparison of Gow-Gate mandibular block and inferior dental nerve block found higher success rate in the inferior dental block than in the Gow-Gate mandibular block. In the molar buccal area the success rates at 5 and 60 minutes after injection were higher in inferior dental nerve block group (97% and 100%) than in the Gow-Gate mandibular nerve block group (88.7% and 99.9%). Though in terms of the efficacy of pulp and gingival tissue anesthesia the difference was not significant.
In our study we have found sequential appearance of anaesthesia in Gow-Gate technique starting from the buccal aspect of canine, followed by the lingual aspect and then the buccal aspect of first molar,signifying that the sequence of exposure of anesthesia was inferior dental nerve first followed by lingual and the long buccal nerve. This could be due to the anatomical positioning of these fibres in the nerve trunk. In our study we have found that 96% of cases in classical inferior dental nerve block were successful with the first injection and only 4% required a repeat block. As against only 78% were successful with the Gow- Gate technique and 22% were found to be not having adequate anesthesia, requiring the repetition of nerve block to attain adequate anesthesia,well supported by Bernhard Rolf Kohler et al., [8] and Yang J, et al. [9]
No injection was administered without two plane aspiration hence intravascular injection as a cause of failure can be excluded. In Gow-Gate technique the solution was deposited only after hitting the neck of the condyle whenever the patient moved his mandible in response to infection we found the failure rate to be highest.
The success of Gow- Gate technique depends upon the position of the condyle.
• The extreme forward position of the condyle, in the wide open mouth position. The penetration of needle during injection is thus much close to nerve trunk.
• The restricting influence of the inter pterygoid fascia that prevent virtually completely the medial diffusion of local anesthetic solution, which must then diffuse predominantly into the sagittal plane, as far as the anterior and posterior limit of the interpterygoid fascia.
Moreover in case of Gow-Gate technique either there is complete failure of the anesthesia or completely effective anesthesia in all three branches i.e., long buccal, lingual and inferioe alveolar nerve, as a longer course of nerve is always bathed in local anesthetic solution. However in case of inferior dental nerve block the possibility of either long buccal or lingual nerve not being anesthetized is always there if the solution is not deposited at the level before the branching takes place. Pain scoring done by the patient himself on visual analogue scale provided by operator. In Group A, 2 (4%) patients reported of Slight discomfort/pain during procedure as compared to 3 (6%) in Group B. However, this difference is not significant.
No complications were encountered during the study except that 3 patients (6%) in group A who received classical inferior alveolar nerve block had post extraction trismus where the patient had undergone atraumatic extraction of mandibular third molar supported by Sthitaprajna Lenka et al. [10] Mean time for recovery from anesthesia from the time of onset of signs and symptoms ranged was 1.8 ± 0.30 hours (90 to 126 minutes) in Group A as compared to 2.57 ± 0.37 hours (132-176 minutes) in Group B. Statistically this difference between groups was significant. This finding of longer duration of anesthesia with the same amount of local anesthetic agent in Gow-Gate technique signifies that more volume of local anesthetic agent is present at the target nerve for a longer period of time owing to the less vascular nature of the surrounding tissue. Hence for the longer procedures, Gow-Gate technique could be preferred. Satisfaction level assessed by visual analogue scoring which was marked by the patient themselves. Majority of patients in both the groups were satisfied or highly satisfied. 68% patients were satisfied and 26% patients were highly satisfied in group A, while 48% patients were satisfied and 44% patients were highly satisfied in group B. Thus in group B more number of patients was highly satisfied. No complication was observed in group B, however, in group A, 3 (6%) cases had trismus. No ocular or other complications were observed in our study which has been attributed to inadvertent intra-arterial deposition of local anesthetic solution. Meticulously following the procedure in two plane aspiration using 25 gauge needles we were able to prevent any inadvertent intravascular injection. Trismus seen in cases of inferior dental nerve block could be due to deposition of anesthetic solution in the medial pterygoid while withdrawing the needle and deposition of anesthetic solution into a highly vascular space.
Conclusion
An evaluation was conducted between the two groups to compare their effectiveness and the following conclusions could be drawn.
• When meticulously followed, both techniques give adequate anesthesia in posterior mandibular region.
• Gow-Gates technique requires greater skill compared to the standard technique.
• The percentage of successful anesthesia in our study for Gow-Gate technique was found greater in comparison to other authors reported earlier. We used 25 gauge needles which have less deflection resulting in accurate positioning of needle at the neck of the condyle and hence resulted in more successful anesthesia.
• We feel that patient attempting to close the mandible or move the mandible during injection may have affected the outcome of the Gow-Gate technique and hence we recommend that a mouth prop can be placed on opposite side to maintain the fixed mouth opening during the procedure.
• Time taken for onset of anesthesia in Gow-Gates technique was greater than inferior dental technique and in some cases it was approximately 20 minutes so it is advisable for the operator to have patience and not to repeat the block.
• Postoperative comfort and patient’s satisfaction was greater in Gow Gates compared to inferior dental nerve block technique.
• In all of the cases using Gow-Gates technique lingual, long buccal and inferior alveolar branches were anesthetized and single branch failure was not observed, signifying that once the Gow-Gates block becomes effective no supplementary block or infiltraion required.
We infer that Gow-Gates technique is superior to inferior alveolar nerve block aut requires expertise and higher skill which one develops with practise. Present study was performed by a single operator and was unicentric. Hence further multicentric study should be done with larger sample size for precise clinical outcomes.
Conflict of Interest
All authors disclose that there was no conflict of interest.
REFERENCES
- George AE. Gow-Gates: Mandibular conduction anesthesia; A new technique using extraoral landmarks; Journals of Oral Surgery 1973; 3: 321-330.
- Haas DA. Alternative mandibular nerve block techniques JADA 142: September 2011; 1-5.
- Yu F, Xiao Y, Liu H, Wu F, Lou F, Chen D, et al. Evaluation of three block anesthesia methods for pain management during mandibular third molar extraction: A meta-analysis, 2017.
- Barodiya A, Thukral R, Agrawal SM, Rai A, Singh S. Temporary Blindness after Inferior Alveolar Nerve Block. Journal of Clinical and Diagnostic Research. 2017; 11: ZD24-ZD25.
- Haghighat A, Jafari Z, Hasheminia D, Samandari MH, Safarian V, Davoudi A. Comparison of success rate and onset time of two different anesthesia techniques Med Oral Patol Oral Cir Bucal. 2015; 20: e459-e463.
- Malamed SF. Handbook of local anesthesia (6th edition) 2011, chapter 11 page 226-223, 236-240.
- Hung PC, Chang HH, Yang PJ, Kuo YS, Lan WH, Lin CP. Comparison of the Gow-Gates mandibular block and inferior alveolar nerve block using a standardized protocol J Formos Med Assoc | 2006; Vol 105: 3-4
- Kohler BR, Castellón L, Laissle G. Gow-Gates Technique: A pilot study for extraction procedures with clinical evaluation and review. Anesth Prog 2008; 5:2-8.
- Yang J, Liu W, Gao Q. The anesthetic effects of Gow-Gates technique of inferior alveolar nerve block in impacted mandibular third molar extraction, 2013; 31: 381-384
- Lenka S, Jain N, Mohanty R, Singh DK, Gulati M. A clinical comparison of three techniques of mandibular local anaesthesia. Journal of Research and Advancement in Dentistry 2013; 2: 61-67.




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.