Debating Elective Single Embryo Transfer after in vitro Fertilization: A Plea for a Context‑Sensitive Approach
- *Corresponding Author:
- Dr. Euzebus Chinonye Ezugwu
Department of Obstetrics and Gynecology, University of Nigeria Teaching Hospital, Ituku-Ozalla, PMB 01129, Enugu, Nigeria.
E-mail: ezugwueuzebus@yahoo.com
Abstract
The number of embryos transferred after in vitro fertilization (IVF) have been a topic of debate for over a decade now. Due to the risk associated with multiple pregnancy, there has been a global effort at reducing the multiple pregnancy rates to a minimum while maintaining an acceptable level of successful IVF pregnancy rate. Elective single embryo transfer (eSET) is advocated in most European countries. In Belgium and Sweden, eSET is mandatory for couples with a good prognosis. However, despite clinical recommendations and policy statements, patients in clinical practice frequently do request for the transfer of multiple embryos in order to have twins. Such requests conflict with policy guidelines and create an ethical dilemma for physicians: Should the physician do as the couple requests, and there with respect the autonomy of patients, or adhere to medical policy that takes the health of the mother and children at heart? This article provides an exploration of the arguments found in the literature that plays a role in the discussion on this topic and eventually argues that what a physician should do depends on the specificities of the context in which patients and physicians are implicated. These contextual issues can be taken into account in a shared decision‑making procedure, which allows reflections and the responsibilities of both patients and physicians to be attended in decision about assisted reproduction.
Keywords
Autonomy, Embryo transfer, in vitro fertilization, Multiple pregnancy, Values and culture
Introduction
Assisted reproductive technology (ART) has restored hope to millions of infertile couples globally, with in vitro fertilization (IVF) and embryo transfer offered in virtually all ART units. This development in medicine lead to the delivery of the first test tube baby named Louise Brown on July 25, 1978 in Oldham, England after a 9-year history of infertility in her mother. This feat was achieved through the collaborative work of Steptoe and Edwards.[1] To date, over 4 million children have been born through IVF and embryo transfer.
However, IVF has also been associated with increased risk of multiple pregnancy.[2-4] Twin gestation and higher order pregnancy, usually, results when two or more embryos are transferred into the uterus after IVF. Countries with a higher incidence of multiple embryo transfer, usually, report a higher multiple pregnancy rate. In Canada, 29% (1003) of the 3428 live births through ART in 2007 resulted in multiple birth, 28.1% (974) were twins and 0.8% (26%) were triplets[5] compared to 9.5% multiple pregnancy rate in Belgium where elective single embryo transfer (eSET) for couples with good prognosis is mandatory.[6]
Several complications have been associated with multiple pregnancy. Some of the maternal complications include preeclampsia and other hypertensive disorders, nutritional deficiency, e.g. iron deficiency anemia, antepartum hemorrhage (abruption placenta and placental previa), postpartum hemorrhage, gestational diabetics, increased operative delivery.[2,3] Fetal complications include increased preterm birth and prematurity. Preterm birth accounts for almost 70% of neonatal deaths and 75% of neonatal morbidity, e.g., respiratory distress syndrome and neonatal infection.[7]
Currently, there is a drift toward elective single embryo transfer (eSET) to reduce the risk of multiple gestation and its attendant maternal and fetal complications. Single embryo transfer after IVF is very effective in preventing multiple pregnancy in IVF cycle. According to the Practice Committee of the American Society for Reproductive Medicine, elective SET is defined as “the transfer of a single embryo at either the cleavage or blastocyst stage of embryo development that is selected from a larger number of available embryos.”[8] The policy of mandatory eSET has been adopted in many developed countries such as Belgium, Sweden, and Quebec (Canada), resulting in a significant reduction of the multiple pregnancy rate.[4,6,9] A recent population-based study in Australia and New Zealand has also demonstrated that eSET results in a significant reduction of perinatal mortality when compared with double embryo transfer (DET).[10]
Policy requiring mandatory eSET may be acceptable in the medical circle, but challenges may nevertheless arise when patients make a request contrary to the policy guideline. In daily practice, this happens regularly. In a study from Port Harcourt, Nigeria, 94.4% of the respondents preferred the transfer of two or three embryos; 66.6% preferred transfer of two embryos while 27.8% preferred more than two embryos.[11] The amount of requests for multiple embryo transfer in the Nigerian study is high. But comparable studies in other countries show that a significant number of parents ask for multiple embryo transfer there too. About 58.7% of the infertile couples (n = 588) in a Danish study preferred having twins to having one child at a time while 89% of infertile couples (n = 265) in a German study desired twin pregnancy.[12,13] Furthermore, the Dutch national survey among 107 IVF professionals report women’s choice for twins (36%) as a perceived barrier for eSET.[14]
These frequent requests for multiple embryo transfer generate an ethical problem for the clinician. Should clinicians accede to the demand of infertile couples, thereby exposing the mother and the infant to a series of possible complications, or should they transfer just one embryo, which reduces the risk of complications and is in line with current medical recommendations? This article explores some of the arguments that have been provided in the literature about eSET and eventually argues that what a physician should do depends on the specificities of the context in which patients and physicians are implicated.
Materials and Methods
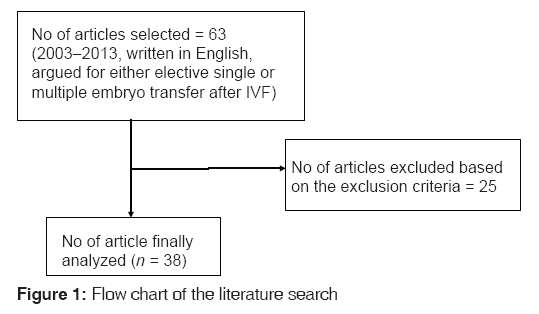
The literature were found through a search in PubMed, Medline, and Web of Science using the keywords: Embryo transfer guidelines, ethics, autonomy, multiple pregnancy, infertile couples’ values and culture, either alone or in combination. Criteria for inclusion in the study included, published articles that span from 2003 to 2013, written in English language and argued for either elective single or multiple embryo transfer after IVF were selected. Sixty-three articles were initially selected but based on above criteria, 38 articles were analyzed. On the basis of these articles, an inventory was made of the arguments that were brought forward. These arguments are described in the section on arguments and weighed in the discussion that follows it in order to find the answer to the question what the doctor should do. A section on socio cultural value was added to highlight the influence of the people’s value system in the decisions they make.
Results
These arguments include:
Medical argument
Medical arguments are primarily concerned with health risk management and cost-effect analyses. It derives its strength mainly from the principle of beneficence and nonmaleficence. The principle of beneficence has been referred to as a “statement of moral obligation to act for the benefit of others” while the principle of nonmaleficence obligates us to abstain from causing harm to other. The principle of nonmaleficence could sometimes be referred to by the maxim ‘Primum non nocere’, meaning, above all, do no harm refer. [15] These ethical principles suggest that doctors should aim at offering health services that will benefit the patient and abstain from causing harm to them.
In medical arguments, multiple pregnancy is considered one of the main complications of IVF and embryo transfer, because of its association with higher maternal and perinatal morbidity and mortality and should be prevented by promoting eSET.[16-24] Compared to a singleton pregnancy, the infant and neonatal mortality rate are higher, about six- and seven-fold in twins and triplet births, respectively.[25]
The risks associated with multiple pregnancy coupled with the advancement in the effectiveness of ART leading to successful pregnancies, lead to a medically supported call to reduce the number of embryos transferred. This arguably is in keeping with the principle of beneficence and nonmaleficence. An example of such call is that of the European Society of Human Reproduction and Embryology (ESHRE), which issued a consensus statement in 2002 that a single healthy baby is the true measure of success and twin gestation is an adverse complication of IVF.[26] However, some IVF experts seem to disagree with this consensus statement.[14,27-29] Gleicher and Barad report that the risk and cost of twin gestation may not be statistically different from singleton pregnancies in couples desiring twin gestation, if the correct methodology and outcome measures are applied in the cost-benefit analysis. They argue that “twin pregnancy is a desirable outcome of pregnancy.”[27] They argued that DET may be desirable, especially because it leads to more babies than eSET.
While studies have shown that eSET increases significantly the chance of healthier live births compared to DET,[18,30] eSET also yields a lower pregnancy and live birth rate compared to DET in a fresh IVF cycle.[30,31] But if eSET is followed by subsequent transfer of single thawed frozen embryo in the subsequent cycle, the live birth rate following eSET becomes comparable with that following DET.[30-32] This is, therefore, the strategy recommended by ESHRE for patients with a good prognosis and at risk of conceiving twins, because unlike double or multiple embryo transfers, eSET followed by the subsequent transfer of a single thawed frozen embryo in the subsequent cycle is associated with a dramatic reduction in the rate of multiple pregnancy.[26,30]
The recommendation of ESHRE, to transfer just one embryo in a fresh cycle and transfer a single thawed frozen embryo in the subsequent cycle in selected cases, gives high regard to risk reduction for the health of mother and child as well as to the effectiveness of IVF in realizing life. These considerations are, however, very general, and are sometimes criticized for not taking sufficiently into account patient’s preference and autonomy. Medical arguments should be attuned to specific characteristics of the patient; such as age, cause of infertility, embryo quality, opportunity for cryopreservation, and the experience of the clinician.[33] All these specifics ought to play a role in medical decision-making about the treatment of a specific couple.
Patient’s autonomy
Medical arguments in favor of eSET are often contrasted with the arguments that support patient autonomy. The principle of respect for autonomy entails “acknowledging the right of an autonomous agent to hold views, to make choices, and to take actions based on their values and beliefs.”[15]
It has been reported that a significant proportion of infertile couples in Europe, the United States, and Africa prefer to transfer more than one embryo in order to achieve a twin pregnancy.[11-13,27,34,35]
These requests raise the question whether the physician ought to comply with these preferences, and respect patient’s autonomy, or not. Respect for patient autonomy is a central constituent of clinical ethics, however, it has only prima facie standing, and competing moral considerations could sometimes override this principle.[15] In a clinical context respect for the autonomy of the patient is, usually, secured by means of an informed consent procedure. There are more and less formal ways to ask for consent, but the standard procedure is (1) that information is provided by health care professionals to the person whose consent is requested, (2) that this person should be able to understand the information that is provided and is thus enabled to (3) voluntarily decide whether or not to consent. In the end (4), the decision to give consent or not should be communicated to the person who requested consent, which in a clinical context would be a health care provider.[36,37]
In the literature discussing single or multiple embryo transfer, however, the topic of informed consent is often discussed in a negative way. The request that infertile couples make for the transfer of multiple embryos, is often represented as not being an autonomous informed decision at all. For example, in the discussion about the California Octuplet that resulted from the transfer of six embryos after IVF by the physician in order to respect the infertile couples’ demand, it is suggested that infertile couples may not be capable to decide by themselves on the number of embryos to be transferred after IVF.[38] Some authors have, therefore, argued that when patients request for medically inappropriate treatment, such as in the octuplet case, medical considerations which are brought forward as beneficence-based considerations and the virtue of professional integrity should draw a limit to patient’s autonomy.[38-40]
Apart from this extreme case, however, some authors also deny that the request for two embryos could result from an informed choice. Ryan et al. argue, for example that an infertile couple’s preference for multiple embryo transfer is based on ignorance and lack of awareness of the risk associated with multiple pregnancy.[35] Some authors argue that if couples still want to have twins, even if they have knowledge about the associated risks, additional interventions are needed to convince the infertile couple to transfer just one embryo.[41]
In spite of these negative approaches to patient autonomy, there are also authors who argue that the informed decision of an infertile couple desiring twin pregnancy should be respected.[27-29] Gleicher, for example, States that he is "struck by how colleagues are willing to ignore their patient’s right to self-determination".[28] Contrary to the most used terminology of eSET, Gleicher speaks about SET, because from the patient’s point of view it is not “elective.” He considers the imposition of SET (..) coercive and incompatible with the patient’s right toward self-determination.[28]
Articles that defend patient autonomy, report different reasons to prefer multiple embryo transfer, such as, the wish to achieve the desired family size, religious belief and socio-cultural factors, and considerations about costs depending on the part of the world where the requesting couples live.
Financial arguments
In general, ART is an expensive procedure making cost considerations important in the decision on the number of embryos transferred during ART. In 2004, about 4% of all preterm birth in USA resulted from ART with an estimated associated cost of about $1 billion.[42,43] In many European countries, and in the countries that mandate eSET by legislation, the government or insurance pays for ART treatment. In these contexts, the government has a stronger say in the decisions about the number of embryos to transfer. Arguably, in line with the principle of justice, there should be fairness in the management of the limited resources of the nation.
Based on studies about the cost effectiveness of eSET over double or multiple embryo transfer,[17,44,45] most European countries advocate for eSET followed by the subsequent transfer of a single thawed frozen embryo in the subsequent cycle for infertile couples with good prognosis. This practice is believed to promote the delivery of healthy babies, eliminating the money spent on the management of complications of multiple pregnancy, and the care for premature babies delivered as an outcome of multiple pregnancy. These countries suppose that funds that are saved in this way can then be used to pay for the cost of IVF for her citizens.[4,17,18]
This argument appears logical as justice demands that governments are expected to manage their limited resources effectively and in all fairness to the benefit of its entire citizen. However, in countries where patients pay for their health care without any hope of reimbursement as seen in most African and Asian countries, and in some parts of the USA and Canada,[4] achieving pregnancy and live birth with minimal attempts becomes a major goal. In most middle and low-income countries, patients do not have the luxury of several attempts as the costs of the first cycle may clear their entire life savings. The costs of an additional cycle of a single thawed embryo after the initial eSET is discouraging: Having to pay for IVF by themselves offers these infertile couples a strong motivation to ask for the transfer of more than one embryo.
In some countries, such as some parts of the UK-just a single IVF treatment is paid for by the insurance and a second treatment is reimbursed only when the first one was unsuccessful. In this context, infertile couples desiring two children may opt for DET in order to increase their chance to realize their desired number of children. DET to achieve twin pregnancy seems economically more acceptable to them.[41] Infertile couples are reluctant to choose eSET if they are not guaranteed reimbursement of eSET plus transfer of subsequent single thawed embryo.[18]
In deciding about the number of embryos, the role of financial evaluations differs, depending on who pays (such as the government or infertile couples themselves). While the government may have the authority to prescribe a guideline requiring eSET in countries where insurance pays for IVF and may even impose legislation, in contexts where patients pay for IVF by themselves there may be urgent reasons to ignore the medical guideline requiring eSET. The persuasive power of the guideline or policy may differ in considerations about how many embryos to transfer, depending on who pays.
Argument Based on Socio-Cultural Values
Socio-cultural values regarding having children and having twins are seldom discussed in the literature on whether to transfer one or more embryo’s in IVF treatment. Yet, in different contexts, there may be different values attached to motherhood and fatherhood, and to have twins. Physicians may encounter these values when they discuss IVF with their patients, and they may play an important role in the patient’s preference for the transfer of one or more embryo’s [Figure 1]. Although the birth of twins was initially seen as a bad omen in some ancient traditional African societies, twins are now received with joy.[46-48] It has been reported that the Yoruba tribe in South Western Nigeria has the highest rate of twin births in the world.[48] In Yoruba land, the birth of twins is welcomed and celebrated with a deeply rooted belief that twins attract supernatural wealth to the family. Twins are believed to bring happiness and joy to families.[46-48] This belief is also shared by the Yamba tribe in Cameroon.[49] Furthermore, the Bamana and Maninka of Mali value twins as a gift from the gods and are accorded privileged status.[50]
Although Christian and Islamic religion in these regions has affected this traditional belief and the performance of the traditional rituals associated with the birth of twins, the desire for twins by both fertile and infertile couples is usually still expressed. Even if many couples agree that there is no scientific evidence to support their belief that twins’ birth attracts wealth and blessing to the family, many still share that belief and it might influence the woman’s preference for the transfer of two or three embryos in order to achieve the desired twin gestation. Denying infertile couples, the opportunity to fulfill their dream within that cultural setting might affect the couple both emotionally and psychologically in a way that infertile couples in other parts of the world could not be affected.
In such a society, these beliefs may explain what patients will put forward when they ask for IVF. Physicians will therefore encounter requests that are motivated in different ways in different contexts; and refusing the realization of this wish will also hurt couples in different ways depending on the context in which they live, and the ideals of a good life that they strive to realize.
Discussion
The arguments provided in the literature offer input to come to an answer to the question what a physician should do when he/she is requested by a patient to transfer multiple embryos in case of IVF against the advocated eSET. The collection of arguments we encountered in the literature suggests that a physician cannot base his or her decision just on medical arguments concerning general risk assessments and cost-effect analyses. Medical judgment itself demands to look at the specific characteristics of the infertile couple, its history of infertility, the quality of the embryo, and the context in which they are being treated.
Besides medical arguments, the literature brings forward other relevant considerations as well, such as considerations about cost-distribution and socio-cultural values which may play a constitutive role in the lives of patients. If we take it that all of these arguments deserve a place in the consideration about the number of embryos to transfer, next to the medical arguments, this would demand to adopt a decision-making procedure that allows bringing in arguments that may differ in each context. As the specific content of these arguments may vary, depending on the local system of cost-distribution as well as the socio-cultural values of the patients that comes to the doctor’s cabinet, we suggest that physicians and patients work together to reach a decision at a specific time in a specific place.
Such a conversation between physician and patient that leads to a decision that satisfies both is furthermore justified by the responsibility of all participants. Since infertile couples need the help of a doctor to have children, it cannot be only the couple’s decision to decide how many embryos ought to be transferred. Respect for the infertile couple’s autonomy as earlier stated has only prima facie standing; therefore, competing moral considerations could sometimes override this principle. For example, request for the transfer six embryos like in the California octuplet[38] case poses significant risk to the mother. Based on other ethical consideration such as the principle of nonmaleficence and virtue of professional integrity of the IVF expert, the request should be denied.[39]
Both parents and physicians have a responsibility for the decision, and both have to be able to live with the eventual result. Shared decision-making would, therefore, seem to be the most appropriate approach, which does justice to the responsibility of all parties. Shared decision making is defined by Angela Coulter and Alf Collins as; “a process in which clinicians and patients work together to select tests, treatments, management or support packages, based on clinical evidence and the patient’s informed preferences.”[51]
A shared decision-making procedure may involve the use of a decision aid, which structures the conversation between doctor and patient and helps to make sure that all relevant topics are covered. The final decision is based on different types of arguments that stem from clinical information, considerations about costs and values that matter to patient’s lives. The content of the topics that are addressed in the conversation may differ from context to context, for example, physicians in Africa may encounter strong socio-cultural or religious beliefs regarding having children and having twins, which are nonexistent or very different in a European context. Nevertheless, these beliefs may be explanatory for the patient’s sense of well-being with the decision that is eventually reached. Furthermore, if the patient herself pays for IVF as in most developing countries, this may explain why a request to transfer more embryos is particularly forceful in this specific context, and physicians will have to deal with stronger expectations to deliver services in exchange for money. In these contexts, DET may be justified. However, in another context in which patients do not have to pay for IVF by themselves, physicians will not have to deal with similar expectations and it may be easier for them to bring forwards arguments from a medical policy perspective and have them heard and accepted by patients. In this context, eSET appears more appropriate. Cost distribution, therefore, also impacts on how different ingredients in the shared decision process are weighed, and will shape the conclusion that is eventually reached.
In the literature, Shared decision-making between the doctor and a well-informed and empowered infertile couple has been reported as an effective approach in deciding on the number of embryos to be transferred after IVF.[28,52] Misinformation about assisted reproduction techniques provokes differences between healthcare personnel and patients. It is very important that infertile couples are offered all the information necessary for informed decision making. In this work, however, Shared Decision Making has been judged for its effectiveness in improving the uptake of eSET through multifaceted empowerment strategy that involves the use of decision aid, support of a nurse specializing in IVF and an offer of an extra cycle.[53] While these support services may not be available in low-income countries – which is an obstacle to the implementation of this particular Shared Decision-Making protocol-the diverse arguments in this article also give reason to ask whether Shared Decision Making should be univocally serving the goal of eSET acceptance. It is not clear in advance that the general medical considerations about eSET always deserve prevalence. Given the medical characteristics of a specific infertile couple that requests IVF, the financial situation in which they operate, and the socio-cultural values that guide their considerations, it may be that a physician and a couple come to the conclusion that DET is appropriate in a young woman with good prognosis.
In this article, we, therefore, want to add that while Shared Decision-Making is sometimes presented as an effective procedure to make patients reach a decision that is in accordance with policy-recommendations, we are more interested in its potential to help physicians and patients to take all the specific arguments into consideration that characterize the situation of the infertile couple, and reach a decision that has a chance to be satisfying to all stakeholders. Policy legislation and mandatory guidelines do not allow for the flexibility needed to address issues in different contexts; such as the medical specifics of the couple, arguments that flow from their socio-cultural values and the financial situation that co-determines their request. But these contextualized issues ought to be taken into account.
Conclusion/Recommendation
What a physician should do when confronted with a patient’s request which conflicts with medical recommendations depends on the specificities of the context in which patients and physicians are implicated. The arguments brought forward in this article pointed out that shared decision making is the appropriate approach, which does justice to the responsibilities that both patients and physicians have in assisted reproduction. But shared decision-making is just a procedural approach, and the quality of the eventual decision that is reached may be very different from context to context.
Acknowledgments
We thank the anonymous commentators of the Erasmus Mundus Master of Bioethics course, who commented on an earlier version of this paper.
References
- Steptoe PC, Edwards RG. Birth after the reimplantation of a human embryo. Lancet 1978;2:366.
- Young BC, Wylie BJ. Effects of twin gestation on maternal morbidity. Semin Perinatol 2012;36:162-8.
- Walker MC, Murphy KE, Pan S, Yang Q, Wen SW. Adverse maternal outcomes in multifetal pregnancies. BJOG 2004;111:1294-6.
- Bissonnette F, Phillips SJ, Gunby J, Holzer H, Mahutte N, St-Michel P, et al. Working to eliminate multiple pregnancies: A success story in Québec. Reprod Biomed Online 2011;23:500-4.
- Gunby J, Bissonnette F, Librach C, Cowan L, IVF Directors Group of the Canadian Fertility and Andrology Society. Assisted reproductive technologies (ART) in Canada: 2007 results from the Canadian ART Register. Fertil Steril 2011;95:542-7.e1.
- Van Landuyt L, Verheyen G, Tournaye H, Camus M, Devroey P, Van Steirteghem A. New Belgian embryo transfer policy leads to sharp decrease in multiple pregnancy rate. Reprod Biomed Online 2006;13:765-71.
- Wen SW, Smith G, Yang Q, Walker M. Epidemiology of preterm birth and neonatal outcome. Semin Fetal Neonatal Med 2004;9:429-35.
- Practice Committee of Society for Assisted Reproductive Technology, Practice Committee of American Society for Reproductive Medicine. Elective single-embryo transfer. Fertil Steril 2012;97:835-42.
- Karlström PO, Bergh C. Reducing the number of embryos transferred in Sweden-impact on delivery and multiple birth rates. Hum Reprod 2007;22:2202-7.
- Sullivan EA, Wang YA, Hayward I, Chambers GM, Illingworth P, McBain J, et al. Single embryo transfer reduces the risk of perinatal mortality, a population study. Hum Reprod 2012;27:3609-15.
- Okohue JE, Onuh SO, Ikimalo JI, Wada I. Patients’ preference for number of embryos transferred during IVF/ICSI: A Nigerian experience. Niger J Clin Pract 2010;13:294-7.
- Borkenhagen A, Brähler E, Kentenich H. Attitudes of German infertile couples towards multiple births and elective embryo transfer. Hum Reprod 2007;22:2883-7.
- Højgaard A, Ottosen LD, Kesmodel U, Ingerslev HJ. Patient attitudes towards twin pregnancies and single embryo transfer - A questionnaire study. Hum Reprod 2007;22:2673-8.
- van Peperstraten AM, Hermens RP, Nelen WL, Stalmeier PF, Scheffer GJ, Grol RP, et al. Perceived barriers to elective single embryo transfer among IVF professionals: A national survey. Hum Reprod 2008;23:2718-23.
- Beauchamp TL, Childress J. Principles of Biomedical Ethics. 7th ed. New York, Oxford University Press; 2013.
- de Mouzon J, Goossens V, Bhattacharya S, Castilla JA, Ferraretti AP, Korsak V, et al. Assisted reproductive technology in Europe, 2006: Results generated from European registers by ESHRE. Hum Reprod 2010;25:1851-62.
- Lukassen HG, Schönbeck Y, Adang EM, Braat DD, Zielhuis GA, Kremer JA. Cost analysis of singleton versus twin pregnancies after in vitro fertilization. Fertil Steril 2004;81:1240-6.
- Association of Clinical Embryologists, Bliss, British Fertility Society, British Infertility Counselling Association, Donor Conception Network, Endometriosis UK, et al. Multiple births from fertility treatment in the UK: A consensus statement. Hum Fertil (Camb) 2011;14:151-3.
- Khalaf Y, Bewley S, Braude P. Reducing multiple pregnancies after assisted reproduction treatment: Québec says ‘Yes, we can!’. Reprod Biomed Online 2011;23:407-10.
- Cabello Y, Gómez-Palomares JL, Castilla JA, Hernández J, Marqueta J, Pareja A, et al. Impact of the Spanish Fertility Society guidelines on the number of embryos to transfer. Reprod Biomed Online 2010;21:667-75.
- Ryan GL, Sparks AE, Sipe CS, Syrop CH, Dokras A, Van Voorhis BJ. A mandatory single blastocyst transfer policy with educational campaign in a United States IVF program reduces multiple gestation rates without sacrificing pregnancy rates. Fertil Steril 2007;88:354-60.
- Kresowik JD, Stegmann BJ, Sparks AE, Ryan GL, van Voorhis BJ. Five-years of a mandatory single-embryo transfer (mSET) policy dramatically reduces twinning rate without lowering pregnancy rates. Fertil Steril 2011;96:1367-9.
- Moustafa MK, Sheded SA, El Aziz Mousta MA. Elective single embryo transfer versus double embryo transfer in assisted reproduction. Reprod Biomed Online 2008;17:82-7.
- Stillman RJ, Richter KS, Jones HW Jr. Refuting a misguided campaign against the goal of single-embryo transfer and singleton birth in assisted reproduction. Hum Reprod 2013;28:2599-607.
- Oleszczuk JJ, Oleszczuk AK, Keith DM, Keith LG. Twin and triplet birth: Facts, figure and cost. Female Patient (Parsippany) 2003;28:11-6.
- Land JA, Evans JI. Risks and complications in assisted reproduction techniques: Report of an ESHRE consensus meeting. Hum Reprod 2003;18:455-7.
- Gleicher N, Barad D. Twin pregnancy, contrary to consensus, is a desirable outcome in infertility. Fertil Steril 2009;91:2426-31.
- Gleicher N. Eliminating multiple pregnancies: An appropriate target for government intervention? Reprod Biomed Online 2011;23:403-6.
- Gleicher N. The irrational attraction of elective single-embryo transfer (eSET). Hum Reprod 2013;28:294-7.
- McLernon DJ, Harrild K, Bergh C, Davies MJ, de Neubourg D, Dumoulin JC, et al. Clinical effectiveness of elective single versus double embryo transfer: Meta-analysis of individual patient data from randomised trials. BMJ 2010;341:c6945.
- Gelbaya TA, Tsoumpou I, Nardo LG. The likelihood of live birth and multiple birth after single versus double embryo transfer at the cleavage stage: A systematic review and meta-analysis. Fertil Steril 2010;94:936-45.
- Pandian Z, Bhattacharya S, Ozturk O, Serour G, Templeton A. Number of embryos for transfer following in-vitro fertilisation or intra-cytoplasmic sperm injection. Cochrane Database Syst Rev 2009:CD003416.
- Practice Committee of American Society for Reproductive Medicine, Practice Committee of Society for Assisted Reproductive Technology. Criteria for number of embryos to transfer: A committee opinion. Fertil Steril 2013;99:44-6.
- Murray S, Shetty A, Rattray A, Taylor V, Bhattacharya S. A randomized comparison of alternative methods of information provision on the acceptability of elective single embryo transfer. Hum Reprod 2004;19:911-6.
- Ryan GL, Zhang SH, Dokras A, Syrop CH, Van Voorhis BJ. The desire of infertile patients for multiple births. Fertil Steril 2004;81:500-4.
- Beauchamp TL, Childress J. Principles of Biomedical Ethics. Oxford: Oxford University Press; 2001.
- Faden T, Beauchamp TL. A History and Theory of Informed Consent. New York: Oxford University Press; 1986.
- Minkoff H, Ecker J. The California octuplets and the duties of reproductive endocrinologists. Am J Obstet Gynecol 2009;201:15.e1-3.
- Chervenak FA, McCullough LB. Professional integrity, respect for autonomy, and the self-regulation of reproductive endocrinology. Am J Obstet Gynecol 2009;201:3-4.
- Rosenthal MS. A preventive ethics approach to IVF in the age of octuplets. Fertil Steril 2010;93:339-40.
- Scotland GS, McNamee P, Peddie VL, Bhattacharya S. Safety versus success in elective single embryo transfer: Women’s preferences for outcomes of in vitro fertilisation. BJOG 2007;114:977-83.
- Collins J. Cost efficiency of reducing multiple births. Reprod Biomed Online 2007;15 Suppl 3:35-9.
- Wright VC, Chang J, Jeng G, Chen M, Macaluso M, Centers for Disease Control and Prevention. Assisted reproductive technology surveillance-United States, 2004. MMWR Surveill Summ 2007;56:1-22.
- Bromer JG, Ata B, Seli M, Lockwood CJ, Seli E. Preterm deliveries that result from multiple pregnancies associated with assisted reproductive technologies in the USA: A cost analysis. Curr Opin Obstet Gynecol 2011;23:168-73.
- Mistry H, Dowie R, Young TA, Gardiner HM, TelePaed Project Team. Costs of NHS maternity care for women with multiple pregnancy compared with high-risk and low-risk singleton pregnancy. BJOG 2007;114:1104-12.
- Renne EP . Twinship in an Ekiti Yoruba town . Ethnology [Internet]. 2001;40:63-78.
- Oruene T. Magical powers of twins in the socio-religious beliefs of the yoruba. Folklore 1985;96:208-16.
- Leroy F, Olaleye-Oruene T, Koeppen-Schomerus G, Bryan E. Yoruba customs and beliefs pertaining to twins. Twin Res 2002;5:132-6.
- Gufler H. Yamba twin ritual. Anthropos 1996;91:33-51.
- Imperato GH, Imperato PJ. Beliefs and practices concerning twins, hermaphrodites, and albinos among the Bamana and Maninka of Mali. J Community Health 2006;31:198-224.
- Coulter A, Collins A. Making shared decision-Making a Reality; No Decision About Me, Without Me The King’s Fund; London 2011. p. 1-56. Available at http://www.kingsfund.org. uk/publications/making-shared-decision-making-reality. last accessed on the 27th September, 2014.
- van Peperstraten AM, Hermens RP, Nelen WL, Stalmeier PF, Wetzels AM, Maas PH, et al. Deciding how many embryos to transfer after in vitro fertilisation: Development and pilot test of a decision aid. Patient Educ Couns 2010;78:124-9.
- van Peperstraten A, Nelen W, Grol R, Zielhuis G, Adang E, Stalmeier P, et al. The effect of a multifaceted empowerment strategy on decision making about the number of embryos transferred in in vitro fertilisation: Randomised controlled trial. BMJ 2010;341:c2501.




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.