Determinants of Adherence to Antiretroviral Therapy among HIV-Positive Women Accessing Prevention of Mother to Child Transmission Services in Ebonyi State, Nigeria
2 Department of Paediatrics, Federal Teaching Hospital, Abakaliki, Nigeria
3 Department of Epidemiology and Medical Statistics, University of Ibadan, Nigeria, Email: ikeola2452@gmail.com
Citation: Agboeze J, et al. Determinants of Adherence to Antiretroviral Therapy among HIV-Positive Women Accessing Prevention of Mother to Child Transmission Services in Ebonyi State, Nigeria. Ann Med Health Sci Res. 2018;8:248-253
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Background: Mother-to-child transmission (MTCT) of HIV accounts for over 90% of all pediatrics infection globally. Strict adherence to antiretroviral drugs is needed to achieve maximal reduction of HIV transmission in pregnancy. Objective: To determine the level of adherence among HIV infected pregnant women on Prevention of Mother to Child Transmission. (PMTCT) antiretroviral therapy and to establish the factors that contribute to poor adherence. Methods: A cross sectional study was conducted in which 268 HIV positive pregnant women were recruited by systematic sampling method from PMTCT clinic of Federal Teaching Hospital Abakaliki. Pre tested interviewer administered questionnaire was used for data collection. Information on socio-demographic characteristics, knowledge of PMTCT, barriers to PMTCT and obstetric characteristics were obtained. Knowledge on PMTCT was accessed and a score of <4 out of 5 indicated poor knowledge. Adherence Level was calculated using the respondent self-report using (3 day recall) and a value < 95% indicated poor adherence. Data were analyzed using descriptive statistics, Chi square and logistic regression (p ≤ 0.05). Results: The mean age was 30.7 ± 4.2 years. Two hundred and nineteen (81.7%) of the respondents were married, 124 (46.3%) were traders and 141 (52.6%) had secondary education. The prevalence of good adherence was 89.2% and 227 (89.0%) had good knowledge of PMTCT. Fear of being identified as HIV positive (21%) pregnancy related illness (13.7%) and forgetfulness (12.5%) were the most common reasons for non-adherence. Partner’s support (OR=.03, 95% CI=0.01-0.09, p=0.001), and duration of ART (OR=4.39, 95% CI=1.3- 14.5, p=0.019) at bivariate analysis were found to be significantly associated with good adherence. Partners support (OR=0.027, 95%CI=0.01-0.09) retained the association with good adherence after controlling for cofounders. Conclusion: The study identified that stigmatization and pregnancy related illnesses were related to poor adherence while having Partners support improve adherence to HAART.
Keywords
Adherence; Antiretroviral; Pregnancy; Prevention; Transmission
Introduction
HIV/AIDS is a major public health problem. About 35.9 million people are currently living with HIV/AID worldwide of which 23.5 million are in Sub-Sahara Africa. [1] Nigeria has a current HIV prevalence of 4.1% with about 3.2 million infected with the virus and estimated 1.6 million eligible for Anti-retroviral drugs. [2]
The main route of Pediatrics HIV infection is Mother-tochild- transmission (MTCT) and accounts for over 90% of all pediatrics infection. Adherence monitoring among large number of women on PMTCT programme in most ART centres in Nigeria is a major concern to achieving ART programme success. World Health Organisation recommends HAART as a key component of all effective PMTCT strategies. About 25- 40% of infants born to HIV-positive mothers will contract the virus without preventive intervention. [3]
Factors that affect ART adherence are known to affect PMTCT service uptake. Studies in Nigeria reveals that the average rate of vertical HIV transmission was 22.5%, but for babies whose mothers had PMTCT service the rate was 9.6% and 2.8%. [4,5] Higher transmission rates were associated with vaginal delivery, breastfeeding and lack of PMTCT services to the mothers. Adherence to ART is an important factor which determines treatment success and occurrence of viral resistance. [6] Previous research findings showed adherence rates of 78.3% and 90.6% and identified factors such as high pill-burden, high cost of transport fares, religion, medical side-effects, stigma and discrimination, attitude and poor education were associated with poor adherence to ARV drugs among patients. [7-9] The poor adherence to therapy resulting from inadequate viral suppression is further challenged by low potency of antiretroviral regimen, Viral resistance to antiretroviral medication and pharmacokinetic interactions causing inadequate drug delivery. [10] The transmissibility of the antiretroviral resistant viruses from person to person further compounds the problem of mother to child transmission of HIV. It is a clinical and public health challenge. [11]
This study was aimed at determining the level of adherence to PMTCT among HIV infected pregnant women on PMTCT antiretroviral therapy, and to identify the factors that contribute to poor adherence. The findings will be useful in planning strategies to improve PMTCT adherence.
Methods
This study was conducted at PMTCT site at Federal Teaching Hospital Abakaliki. The Federal Teaching Hospital, Abakaliki is a tertiary health care facility established in the year 2012. The hospital is a referral centre for health facilities within and outside the state and located in Abakaliki the capital of Ebonyi state Nigeria. The inhabitants are mainly the Igbos. About 75% of the populations dwell in the rural areas with farming as their major occupation. [12]
The PMTCT clinic in the hospital is the main service provider of PMTCT services in Ebonyi State. It currently provides counseling and testing, treatment and care services for over 10,000 HIV/AIDS patients. The HIV clinic received addition support from donor Agencies with about 2000 patients on PMTCT in 2015.
Study design
It was cross sectional study at the PMTCT clinic of Federal Teaching Hospital, Abakaliki, Nigeria.
Study Period
The period for the preparation and conclusion of the study was from January, 2016 to July, 2016. The pilot study and pre-test of study materials were conducted in March, 2016 while the main data collection was carried out in April and May, 2016.
Sample size
Sample size was calculated using the formula:
n= (Z2pq/d2)
Where; p=prevalence of ART non adherence among pregnant women in Nigeria, i.e., 19.4% [8]
d==Allowable Error (5%), and q=100-p.
Therefore the sample size (n)=Z2pq/d2 1.96 × 1.96 × 0.194 (1- 0.194)/0.05 × 0.05=240
The minimum sample size was obtained after adjusting for nonresponse rate of 10% (n =240/0.9)=267.
Study population
The study population includes all HIV positive pregnant women enrolled in PMTCT at Federal Teaching Hospital Abakaliki.
Inclusion criteria
HIV positive pregnant women with known gestational age who have received ART therapy for at least 3 month prior to the study period and are able to give informed consent.
Exclusion criteria
Patients who stopped ART on medical grounds and patients who were very sick.
Sampling method
Systematic random sampling technique was applied for participants‟ selection in the study. The sampling units were pregnant women who have been at least 3months on ART prior to the study. From the list of patients attending the HIV Clinic obtained from Medical Records Department and based on average daily clinic attendance of 100 patients per day, a total of 25 eligible patients were recruited per clinic day using systematic random sampling method using a sampling fraction of 1:4. The first patient was randomly selected; thereafter every other fourth eligible patient was selected each until the sample size was completed. For those who failed to consent on particular clinic days, they were subsequently replaced using the same sampling technique on subsequent clinic days.
Data collection
A pretested structured interviewer administered questionnaire was used. It was pretested at the PMTCT clinic Federal Teaching Hospital Abakaliki. The questionnaire captured information on their self-reported adherence levels, their socio demographic indices as well as their knowledge and perceptions towards antiretroviral therapy and other factors that may influence their strict adherence to treatment. Following the written informed consent process, the structured questionnaire was administered by a trained research assistant who understands the local language very well. Participant specific identifiers were used to ensure that no participant will be interviewed more than once. Participants were interviewed in a quiet private room by the research assistant.
Assessment of adherence and knowledge
The main outcome variable was the Adherence status of the respondents. This was measured by three days recall of their intake of prescribed doses prior to the interview. 8 To minimize recall bias the patients were asked about their adherence over the previous day, previous 2 days, previous 3days and previous week. The adherence level was calculated using the respondent’s self-report and the following formula.
Adherence (%)=Number of pills (doses) taken × 100/Number of pill prescribed or supposed to be taken where number of pills taken=number of pills prescribed or supposed to be taken – number of pills missed over one month period. [13,14]
The level of adherence was classified into ‘good adherence’ those with ≥ 95% adherence and ‘poor adherence’ those with <95% adherence. The respondents’ level of knowledge was computed by the total correct responses to the questions posed to test for knowledge and those who accepted all the correct responses were grouped as having ‘good knowledge.
Statistical analysis
Epi info software version 7.1.4 (CDC, Atlanta, Georgia, USA). was used for data analysis. Univariate analysis was performed for frequencies and proportions, bivariate analysis for associations using chi square test of statistical significant. Logistic regression was used to identify independent predictors of poor adherence among the study group. Statistical significant level was taken at p value ≤ 0.05 at 95%confidence interval.
Ethical considerations
Ethical approval with reference no. EB/EBOSACA/ES/R/003 for the study was obtained from Ministry of health Ebonyi state. Ethical standards and best practice were adhered to throughout the conduct of the study
Results
Two hundred and sixty eight eligible HIV –positive pregnant women were interviewed. Two hundred and thirty nine (89.2%) had adherence level of ≥ 95%. The non-adherent rate level was 10.8%.
Respondents’ socio-demographic characteristics
The Respondents’ socio-demographic characteristics are shown in Table 1. The mean age was 30.7 ± 4.2 years. Majority of the women were aged between 30-34 years (42.9%) followed by 25-29 years (31.8%). Most of the women 219 (81.72%) were married and 124 (42.27%) were Traders. One hundred and forty one (52.6%) of the respondents, had secondary education and 72 (26.7%) had tertiary education. Fifty-six (20.9%) of respondents were unemployed and 20 (7.46) were civil servants.
| Characteristics | Percentage (%) |
|---|---|
| Age (years) | |
| 20-24 | 16 (5.9) |
| 25-29 | 85 (31.8) |
| 30-34 | 115 (42.9) |
| 35-39 | 52 (19.4) |
| Marital status | |
| Married | 219 (81.7) |
| Single | 49 (18.3) |
| Occupation | |
| Banker | 7 (2.6) |
| Civil servant | 20 (7.5) |
| Farmer | 10 (3.7) |
| Hair dresser | 28 (10.5) |
| Tailoring | 11 (4.1) |
| Student | 12 (4.5) |
| Trader | 124 (46.3) |
| Not employed | 56 (20.9) |
| Educational level | |
| No formal education | 24 (6.9) |
| Primary | 31 (13.8) |
| Secondary | 141 (52.6) |
| Tertiary | 72 (26.7) |
Table 1: The socio-demographic characteristics of HIV infected pregnant woman accessing PMTCT in Ebonyi state, Nigeria, 2016.
Table 2 shows the two hundred and thirty three (86.9%) had partners support and 161 (60.1%) had been on ARV drugs for more than two years. Two hundred and twenty three (83.2%) commenced ARV drugs in their index pregnancy and 167 (62.3%) have no previous PMTCT experience. Of the two hundred and sixty eight respondents 184 (68.7%) have gestational ages between 13-28 weeks followed by those whose gestational ages were above 28 weeks.
| Characteristics | Number of respondents (%) |
|---|---|
| Duration of ART | |
| 0- 2 Years | 107 (39.93) |
| >2years | 161 (60.07) |
| Partners Support | |
| Yes | 233 (86.94) |
| No | 35 (13.06) |
| Gestational Age | |
| <13 weeks | 3 (1.12) |
| 13-28 weeks | 184 (68.66) |
| >28 weeks | 81 (30.22) |
| Previous PMTCT Experience | |
| Yes | 101 (37.7) |
| No | 167 (62.3) |
| Time of ART initiation | |
| Before pregnancy | 45 (16.8) |
| Index pregnancy | 223 (83.2) |
Table 2: The pregnancy and HIV characteristics of the HIV infected pregnant women accessing PMTCT in Ebonyi state, Nigeria, 2016.
Barriers to ART adherence among respondents
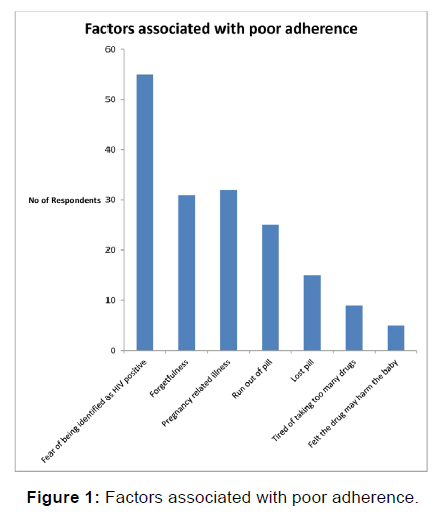
Figure 1 shows the reasons given by the Respondents for missing or skipping their drugs. The fear of being identified as HIV positive (55.0%) was the main reason for missing drugs followed by pregnancy related illness (32%). Others include forgetfulness (31%), and run out of pill (25%).
Knowledge of PMTCT and ART by the respondents
All the respondents knew that MTCT is possible and 248 (92.5%) knew that HAART can prevent transmission of HIV. Two hundred and fifty four (94.8%) respondents were sure that they will take HAART as prescribed while only 7 (2.6%) do not know the consequences of not taking the drugs as prescribed. Two hundred and sixty one (97.4%) respondents knew that HAART can prevent opportunistic infection. On the Knowledge score, 255 (95.2%) of the respondents had good knowledge of PMTCT. Respondent mean knowledge score was 2 ± 0.04 [Table 3].
| Variables | Frequency | Percentage (%) |
|---|---|---|
| HIV can be transmitted from mother to child during pregnancy? | ||
| Yes | 268 | 100 |
| No | 0 | |
| Can HAART prevent MTCT | ||
| Yes | 248 | 92.5 |
| No | 20 | 7.5 |
| Will you be able to take HAART as prescribed | ||
| Very sure | 254 | 94.8 |
| Not sure | 14 | 5.2 |
| Do you know the consequences of not taking drugs | ||
| Yes | 261 | 97.4 |
| No | 7 | 2.6 |
| Can HAART prevent opportunistic infections | ||
| Yes | 261 | 97.4 |
| No | 7 | 2.6 |
| Knowledge of PMTCT | ||
| Good | 255 | 95.2 |
| Poor | 13 | 4.9 |
Table 3: Knowledge of PMTCT by HIV infected pregnant women accessing PMTCT in Ebonyi state, Nigeria, 2016.
Factors associated with ART adherence
Table 4 shows the association between the socio-demographic characteristics and ART adherence. Of all the variables, Age (p=0.591), Occupation (p=0.909), Marital status (p=0.263) and level of education (p=0.054), were not significantly associated with good adherence.
| Factors | Adherence (%) | Non Adherence (%) | X2 | p-value |
|---|---|---|---|---|
| Age (years) | ||||
| 20-29 | 91 (91) | 9 (9) | 0.29 | 0.591 |
| 30-39 | 148 (88.1) | 20 (11.9) | ||
| Occupation | ||||
| Employed | 179 (89.1) | 22 (10.9) | 0.01 | 0.909 |
| Unemployed | 60 (89.6) | 7 (10.5) | ||
| Marital status | ||||
| Married | 198 (90.4) | 21 (9.6) | 1.25 | 0.263 |
| Single | 41 (83.7) | 8 (16.3) | ||
| Level of Education | ||||
| ≤ Primary | 53 (96.36) | 2 (3.6) | ||
| Secondary | 120 (85.11) | 21 (14.9) | 5.83 | 0.054 |
| Tertiary | 66 (91.67) | 6 (8.3) |
Table 4: The association between socio-demographic characteristics and ART adherence among HIV-positive pregnant women accessing PMTCT in Ebonyi state, Nigeria, 2016.
Association between obstetrics characteristics and ART adherence
Table 5 shows the association between Obstetric characteristics and ART Adherence. Of the variables, gestational age (p=0.983) was not significantly associated with ART adherence. Duration of ART (p=0.019) and Partners support (p=0.001) were found to be significantly associated with good adherence. ART Adherence. There was no significant association between Knowledge and ART Adherence (p=0.931).
| Factors | Adherence Respondents (%) | Non adherence Respondents (%) | X2 | p-value |
|---|---|---|---|---|
| Gestational age | ||||
| <28 weeks | 71 (89.9) | 8 (10.1) | 0.00 | 0.983 |
| ≥28 weeks | 168 (88.9) | 21 (11.1) | ||
| Duration of ART | ||||
| 0-2years | 78 (88.6) | 10 (11.3) | 5.46 | 0.019 |
| Above 2years | 137 (97.2) | 4 (2.8) | ||
| Partners Support | ||||
| Yes | 218 (93.6) | 15 (6.4) | 67.2 | < 0.001 |
| No | 6 (30) | 14 (70) | ||
| Knowledge of ARV/PMTCT | ||||
| Good | 227 (89.0) | 28 (10.9) | .007 | 0.931 |
| Poor | 12 (92.3) | 1 (7.7) |
Table 5: Association between Obstetrics characteristics and ART Adherence of HIV infected pregnant women accessing PMTCT in Ebonyi state, Nigeria, 2016.
Binary logistic regression
Analysis of factors associated with art adherence during pregnancy. Table 6 shows that Partners support (OR=0.27; 0.01- 0, 08; p<0. 05) retained the association with good adherence. Those that do not have partner support are three times less likely to adhere to ART in pregnancy than women with partners support
| Variables | OR | 95% confidence Lower |
Interval Upper |
p-value |
|---|---|---|---|---|
| Duration of ART | ||||
| >2 | 1 | |||
| ≤ 2 | 0.3 | 0.06 | 1.92 | 0.219 |
| Partners support | ||||
| Yes | 1 | |||
| No | 0.03 | 0.01 | 0.08 | < 0.001 |
Table 6: Factors associated with ART adherence during pregnancy.
Discussion
In this study, 89.2% reported good adherence. The higher adherence among HIV positive pregnant women suggests that women are always willing to protect their offspring from harm. The non-adherence rate was 10.8%. This finding is lower than 21.7% reported in South east Nigeria and comparable to 19.4% reported in South west Nigeria. [7,8] It is much lower than 37.1% and 37.4% reported from Southwestern Nigeria, among people living with HIV. [9,15] It seems that adherence is much better in pregnancy. [7,8] The fact that there is no gold standard in the measurement of adherence and the differences in the quality of service delivery provided to the patients might have accounted for differences in adherence levels from other studies. [8]
The adherence measurement technique used in this study though may be prone to recall bias has been shown to demonstrate a strong association to virologic, immunologic and clinical outcomes in HIV treatment. [6,16] Other methods are either expensive, laborious or impractical for routine use in clinical settings. [17]
Most of the respondents were married, aged between 30 and 34 years and had secondary level of education. The inhabitants being mostly subsistent farmer may have contributed to these findings. The social demographic characteristics of the respondents did not affect significantly the adherence level in our study. This corroborates with the findings of other researchers. [8,18,19]
Most of the respondents had good knowledge about ART/ PMTCT. Given that pregnant woman are generally required to attend health facilities for regular health checks, the contacts with the health care workers and the health education which is routine during the antenatal period could have contributed to the good knowledge recorded. This is similar to findings from other studies in Nigeria. [7-9,20-22] Other researchers from some African countries have also reported higher level of knowledge about ART/PMTCT among study respondents. A study in Ghana reported 96.7% among pregnant women accessing PMTCT service. [23]
It would be expected that high knowledge of ART among study participants would have influence on adherence. In this study, there was no association between adherence and level of knowledge. This was similar to report in Lagos [8] but in contrast to the report from Nnewi. [7,23]
The main factor associated with poor adherence was fear of being identified as HIV positive. This is not surprising as discrimination and stigmatization against people living with HIV is common in our society and remains important factors militating against quality HIV care. Similar findings were documented in Nigeria. [8,9,24] The effect of pregnancy related illnesses was noticed in this study, as a major reason for missing drugs. Our findings suggest the need for obstetricians and midwives to routinely evaluate patients who are in their first and second trimesters and advise them on what to do regarding the taking of their medications. Other reasons reported were forgetfulness, Loss of pill, tired of taking too many drugs and feelings that the drugs will affect the baby. These findings were consistent with other studies in Nigeria. [25,26]
Women who have been on ART for up to two years, in our study, were found to be more likely to be adherent to their ARV drugs.. Patients who commenced antiretroviral therapy newly usually experience severe side effect and therefore may not adhere strictly to the treatment compare to the people who had been on ART for more than two years. This is consistent with a study in Zambia but contrast to the study in Nnewi. [7,27]
The multivariate logistic regression showed that those who have partners support were more likely to have good adherence to ART. This finding is consistent with previous studies. [8,28] The disclosure of HIV status to partner will not only provide support but also act as treatment partner, although in some cases disclosure could be accompanied by partner violence. [28]
Limitations
The study was facility based. Data on HIV-related parameters (CD4 cell count, HIV RNA) and antiretroviral regimen used and the rate of MTCT were not included in the study. Adherence was calculated using self-report, some of the respondents might have over- or under- reported their adherence to ART due to challenge of remembering the number of times they miss their dosages
Conclusion
The level of adherence on ART in this study was high. Partners support was significantly associated with good adherence. The major reasons for missing drugs were stigmatization, pregnancy related illness and forgetfulness. There was a high knowledge of PMTCT and HIV/AIDS among the respondents.
Acknowledgement
We appreciate the Nigeria Field Epidemiology and Laboratory Training Programme (NFELTP), for providing technical supports during the study period.
We thank the Staff of Obstetrics and Gynaecology department and management of Federal Teaching Hospital Abakaliki for their support during the study period.
Conflict of Interest
The authors disclose that they have no conflicts of interest.
REFERENCES
- Global Health Observatory (GHO). 2013.
- Federal Ministry of Health. National HIV Sero-prevalence Sentinel Survey Technical Report. 2010;1-111.
- Abdulsalami N, Tekena O. The epidemiology of HIV/AIDS in Nigeria, in AIDS in Nigeria: A Nation on the Threshold, O. Adeyi, P. Kanki, O. Odutolu, and J. Idoko, (Eds), Havard Center for Population and Development Studies, Cambridge, Mass, USA. Joseph Afe. 2011. HIV & AIDS Review 10; 2011.
- Ikechebelu JI, Ugboaja JO, Kalu SO, Ugochukwu EF. The outcome of prevention of mother to child transmission (PMTCT) of HIV infection programme in Nnewi, southeast Nigeria. Niger J Med 2011;20:421-425.
- Mannheimer SB, Matts J, Telzak E, Chesney M, Child C, Wu AW. Quality of life in HIV-infected individuals receiving antiretroviral therapy is related to adherence. AIDS Care, 2006;17:10-22.
- Igwegbe AO, Ugboaja JO, Nwajiaku LA. Prevalence and determinants of non-adherence to antiretroviral therapy among HIV positive pregnant women in Nnewi, Nigeria. International Journal of Medicine and Medical Sciences, 2010;2:238-245.
- Ekama SO, Herbertson EC, Addeh EJ, Onwujekwe DI, Tayo F, Ezechi OC. Pattern and Determinants of Antiretroviral Drug Adherence among Nigerian Pregnant Women. Journal of Pregnancy. 2012:1-6.
- Olowookere SA, Fatiregun AA, Adewole IF. Original Article Knowledge and attitudes regarding HIV/AIDS and antiretroviral therapy among patients at a Nigerian treatment clinic. J Infect Dev Ctries. 2005;6:809-816.
- Weiser SD, Leiter KHM. A population-based study on alcohol and high-risk sexual behaviour in Botswana. PLoS Medicine. 2006;3:1940-1948.
- Oku AO, Owoaje ET, Ige OK, Oyo-Ita A. Prevalence and determinants of adherence to HAART amongst PLHIV in a tertiary health facility in south-south Nigeria. BMC Infectious Diseases BMC-I Disease Infectiousness. 2013;13:1-9.
- National Population Commission. Report of Nigeria’s National Population Commission on 2006 Census, Population and Development Review. 2007;33:206-210.
- Ogundahunsi OA, Daniel OJ, Oladapo OT. Adherence to antiretroviral drugs among AIDS patients in Sagamu, Nigeria. International Journal of Biomedical and Health Sciences. 2008;4:41-45.
- Onyeonoro UU, Ebenebe UE, Ibeh CC, Nwamoh UN, Ukegbu AU, Emelumadu OF. Human immunodeficiency virus/acquired immunodeficiency syndrome in a tertiary health facility in South Eastern Nigeria. Journal of HIV and Human Reproduction. 2013;1:1-6.
- Shaahu VN, Lawoyin TO, Sangowawa AO. Adherence to highly active antiretroviral therapy (HAART) at a Federal Medical Centre. Afr J Med Med Sci. 2008;37:29-36.
- Nieuwkerk PT, Sprangers MA, Burger DM. For the ATHENA project. Limited patient adherence to highly active antiretroviral therapy for HIV-1 infection in an observational cohort study. Arch Intern Med. 2001;161:1962-1968.
- Arnsten JH, Demas PA, Farzadegan H, Grant RW, Gourevitch MN, Chang CJ, et al. Antiretroviral Therapy Adherence and Viral Suppression in HIV-Infected Drug Users: Comparison of Self-Report and Electronic Monitoring. Afr. J. Med. Med. Sci., 2001;37:29-36.
- Mohammed MD. Adherence to antiretroviral drugs in North-Central zone of Nigeria. East and Central African Journal of Pharmaceutical Sciences. 2004;7:52-55.
- Kleeberger C, Phair J, Strathdee S, Detel R, Kingsley L, Jacobson LP. Determinants of heterogeneous adherence to HIV antiretroviral therapies in the multicentre AIDS cohort study. J. AIDS. 2001;26:82-92.
- Uzochukwu B, Onwujekwe O, Onoka A, Okoli C, Uguru N, Chukwuogo O. Determinants of non-adherence to subsidized anti-retroviral treatment in southeast Nigeria. Health Policy Plan. 2009;24:189-196.
- Afolabi MO, Ijadunola KT, Fatusi AO. Determinants of adherence to antiretroviral drugs among people living with HIV/AIDS in the Ife-Ijesa of Osun State, Nigeria. African Journal of Primary Health Care and Family Medicine. 2006;1.
- Falang KD, Akubaka P, Jimam NS. Patient factors impacting antiretroviral drug adherence in a Nigerian tertiary hospital. Journal of Pharmacology and Pharmacotherapeutics. 2012;3:138-142.
- Boateng D, Kwapong GD, Agyei-baffour P. Knowledge, perception about antiretroviral therapy (ART) and prevention of mother-to-child-transmission (PMTCT) and adherence to ART among HIV positive women in the Ashanti Region, Ghana: a cross-sectional study. BMC Womens Health. 2013;13:2.
- Amberbir A, Woldemichael K, Getachew S, Girma B, Deribe K. Predictors of adherence to antiretroviral therapy among HIV-infected persons: a prospective study in Southwest Ethiopia. BMC Public Health. 2008;8:265.
- Sekoni AO, Obinna RO. Stigma, medication adherence and coping mechanism among people living with HIV attending General. Afr J Prm Health Care Farm Med. 2012;4:1-10.
- Kasumu LO. Knowledge and attitude towards antiretroviral therapy and adherence pattern of HIV patients in southwest Nigeria. International Journal of Infection Control. 2014;10:1-8.
- Carlucci JG, Kamanga A, Sheneberger R, Shepherd BE, Jenkins CA, Spurrier J. Predictors of adherence to antiretroviral therapy in rural Zambia. J. Acquir. Immune Defic Syndr. 2008;47:615-622.
- Nachega JB, Michael H, Dowdy DW, Lo M, Omer SB, Leon P. Adherence to highly active antiretroviral therapy assessed by pharmacy claims predicts survival in HIV-infected South African Adults. J. Acquir. Immune Defic. Syndr., 2006;43:1-7.
- Ezechi OC, Gab-Okafor C, Onwujekwe DI, Adu RA, Amadi E, Herbertson E. Intimate partner violence and correlates in pregnant HIV positive Nigerians. Archives of Gynecology and Obstetrics, 2009;280:745-752.




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.