Development of the Local Urban Family Physician Model
2 Health Services Management, Social Determinants of Health Research Center, Health Research Institute, Babol University of Medical Science, Babol, Iran
3 Infectious Diseases and Tropical Medicine Research Center, Health Research Institute, Babol University of Medical Sciences, Babol, Iran
4 Social Determinants of Health Research Center, Health Research Institute, Babol University of Medical Sciences, Babol, Iran, Email: khadijehezoji2@gmail.com
Received: 03-Mar-2022, Manuscript No. AMHSR-22-50564; Editor assigned: 04-Mar-2022, Pre QC No. AMHSR-22-50564; Accepted Date: Mar 31, 2022 ; Reviewed: 21-Mar-2022 QC No. AMHSR-22-50564; Revised: 28-Mar-2022, Manuscript No. AMHSR-22-50564; Published: 31-Mar-2022, DOI: 10.54608.annalsmedical.2022.32
Citation: Roudbari JA, et al. Development of the Local Urban Family Physician Model. Ann Med Health Sci Res. 2022;12:101-111.
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Background: Urban family physician program is a health-based plan based on disease prevention. This plan began in Mazandaran province as one of the pilot provinces; so far, the implementation of this project has not been possible in all cities in the country. The purpose of this study was to design the native model of urban family physician using the research method. Materials & Methods: In the current qualitative study, data was collected using semi-structured interviews of 40 people including urban family physicians, health care providers, experts and recipients. Questions included the strengths or achievements, weaknesses or challenges of implementing a family physician program and suggestions. With the aim of extracting the components of the model, this information was categorized and analyzed based on the thematic analysis. Results: In this study, achievements, design challenges and strategies were coded separately. Qualitative data analysis in the coding process led to the emergence of 5 main code and 15 sub codes. The main 5 code were named: Financing, financial payments, regulations, organizing and behavioral. Conclusion: The results revealed that each of the main areas obtained in this study requires changes that will allow better implementation and development of this valuable plan to other cities.
Keywords
Primary health care; Family physician program; Iran
Introduction
In recent years, there have been significant changes in the country's health system and the provision of health services to the population of rural and urban areas through the implementation of family physician program and the establishment of health teams in health centers. By global definitions, the family physician should be at the heart of governments' efforts to improve the quality of health care, reduce costs, and establish justice in health care systems. Health is the axis of social, economic, political and cultural development of all human societies and has a special importance in the development of infrastructure of different sections of society. Therefore, the establishment of a health care system in the basic principles of development is inevitable. The health care system, which includes all organizations, institutions and individuals providing health services, has been formed in different countries in order to improve the level of health of individuals and being affected by economic, political and social conditions in different ways. [1-3] Studies showed that despite the fundamental role of the health system in all-round development, many of the world's health systems are still poorly managed and many countries still have many problems in making decisions in their health sector. [4] The structure of health care systems and the coordination between affairs can determine the efficiency and the rate of achievement of goals. According to the World Health Organization, the United States ranks 37th in the world with 13% of gross national income invested, Singapore ranks 6th with an investment of 3.1% and Iran ranks 93rd in the world with 4.4%. [5]
Therefore, the structure of the health care system in many countries is changed and reformed from time to time in order to achieve greater efficiency, as well as to create justice and access for individuals. The most common changes and reforms made in the health care system in many countries have been the leveling of health system organizations, which are mainly organized into the first, second and third levels. In a graded system, lower-level staff must refer patients to more specialized services, if they are unable to diagnose or treat their patients. Therefore, individuals have access to specialized services through a referral system.
Establishing and strengthening a referral system should reflect the two-way exchange of information and the patient's return to where they were referred from. As a matter of fact, the first level of referral recipient returns the patient to the referring unit by announcing their condition and instructing local staff on how to follow up and care for the patient. In this case, the referral system is not only helpful in prioritizing patients to receive more specialized services, but can also be effective in training and guiding local staff in order to properly deal with issues and referrals. [6]
The Iranian health system has experienced its biggest structural reforms in 1984. In these extensive reforms, the health care network has been gradually established in all cities and a considerable population of urban areas and a large population of rural areas were covered by the first level of the health network. Although these reforms have increased public access to first-level services, followed by significant gains in health indicators, [7,8] public access to second- and third-level services has always been fraught with difficulties, one of which is the lack of a health-oriented approach and attention to prevention compared to treatment in the country's health system. Unfortunately, this problem has also become a culture among the people to go to a specialist or subspecialist with the first pain they feel, while this situation does not exist in most countries, especially in developed countries. Due to this inadequacy in the health care system and misconduct of a significant percentage of people, meeting the needs related to public health is still an important concern of officials and policy makers.
Article 90 (Chapter 7) of promoting health and improving the quality of life of the people stipulates that the share of people in medical expenses should increase from 54% at the beginning of the program to 30% at the end of the program in the fourth development plan, but the evidence shows that the share of people's expenses in providing the required health services has not been reduced to the desired level yet.
In Iran, a lot of efforts have been made to establish a good system that can fully meet the needs of the community. The rapid progress of the country's health system and a huge number of achievements were the result of the establishment of the health care network system in the country. [9] Services were leveled and a referral system was formed to manage them. Inadequate realization of the referral system in the design of the health care network and leveling of services can be considered as a clear weakness of the health system. [10]
The rural family physician and rural insurance program has been implemented in rural-nomadic areas and cities with a population of less than 20,000 since the beginning of 2005 to achieve public health coverage, which is very important in forming a referral system and improving service quality and efficiency in health care systems as well as reducing costs. [11]
Nearly three years after the implementation of the rural family physician program, the implementation of the urban family physician program was emphasized by the then government. Finally, after many years, the urban family physician project started in 2012 in Mazandaran and fars as two pilot provinces. Education and prevention was the main priority of the project in order to reduce the costs of the medical sector in the country.
Materials and Methods
This research has been done qualitatively using a participatory approach. Forty people were surveyed in four separate panels (10 people per panel) by purposive sampling method. Data were collected using semi-structured and interactive interviews to obtain the required information.
Four separate expert panels with specific key questions included: A panel of urban family physicians with at least one year of experience, several family physician representatives, of all ages and genders, willing to continue serving in the program.
The second panel was about health care providers who were in the same situation as family physicians.
The third panel was related to the managers and staff experts of the councils of the city health center who had at least one year of experience in monitoring the program or involved in the implementation of the program (from different technical units).
The fourth panel was about recruiters, who were secretaries, office workers, businessmen and housewives who had seen a family physician at least twice in the past year.
Key questions for a semi-structured interview: What are the strengths or achievements and weaknesses or challenges of implementing a family physician program?
Where do you think the family physician program needs to be changed to make it more effective? What is your suggestion?
Content analysis method is a widely used qualitative research technique. To analyze the data. Content or thematic analysis is a way to analyze, and articulate patterns within some given qualitative data. This method organizes the data and describes it in detail; but it can go beyond this and interpret different aspects of the research topic. The contents of the first session were carefully implemented and the notes were read several times to gain a general understanding of the text, then the initial coding was done and then a theme was given to the main concepts in these sentences. After reviewing all the panels, a list of main and sub-themes was obtained.
The main themes, sub-themes and second level coding were read and the main themes of the same sub-codes with similar meanings were formed and the main codes were formed. To validate the results, the opinions of colleagues were used and interviews were read frequently. External monitoring was also used to increase its reliability, and part of the data was given to a researcher who was not part of the research team to determine whether he or she, as an external observer, had a similar understanding of the data.
Results
The answers of the four groups including urban family physicians, health care providers, experts and staff and service recipients on questions related to the strengths or achievements, weaknesses or challenges of implementing the family physician program and suggestions from their own point of view, were categorized as follow.
Achievements of the implementation of the program
In response to the question "What are the strengths or achievements of the implementation of the family physician program?" The different groups involved in the study had a different perspective, which is shown in Table 1.
Challenges of the program: In response to the question "What are the weaknesses or challenges of implementing the family physician program?" the opinions of the groups were different [Table 2]. Policies in recruitment, management, insurance coverage, payment system problems and service delivery were among the challenges outlined.
| From the point of view of family doctors | From the point of view of health care providers | From the point of view of experts and staff officials | From the point of view of service recipients |
|---|---|---|---|
| Increasing the employment of doctors, especially young physicians | The possibility of employing midwives in this plan | The possibility of employing midwives in this plan | Free of charge is a large part of the service |
| Identification of a large number of people with high blood pressure or diabetes | Reduction of treatment and health costs | Further training of the staff of the Comprehensive Urban Health Services Center | Easy access to services |
| Reduction of elf-medication behaviors | Increasing access to services | Division of the entire urban population between the implementing centers | Follow up patients |
| Reduction of treatment costs | Fewer referrals to level two and three specialists | ||
| Increasing access to services | Reducing health costs | ||
| Increasing service access |
Table 1: Achievements of the program from the perspective of experts.
| Original codes | Sub codes | |||
|---|---|---|---|---|
| rom the point of view of family doctors | From the point of view of health care providers | From the point of view of experts and staff officials | From the point of view of experts and staff officials | |
| Financing | Lack of insurance for doctors | Lack of insurance for health care providers | Financing by the insurance system is a factor for creating problems and lack of coordination | |
| Non-implementation of the program in the whole country and in all insurance funds | Lack of insurance coverage in health prevention and promotion services | |||
| Not all insurances are in the plan | ||||
| Financial payments | Current payment depending on the rating 50:50 instead of the payment in the recipe in the form of 80:20% | Non-separation of health care providers' receipts from physicians | ||
| Non-compliance of receipts based on variable economic conditions | ||||
| Delayed payments to doctors | ||||
| Lack of incentives for doctors and the existence of deductions | ||||
| Raising per capita in line with current inflation | ||||
| Organizing | Private hospitals are not accountable to the referral system | Doctors and midwife have become computer operators instead of doing the main job of caring for clients | The treatment-oriented nature of this program in implementation rather than health-oriented | Doctors move from place to place and confuse patients |
| Lack of support from level two experts for feedback in the referral system | Employer physician is an obstacle to doing the right team work | More policymakers pay attention to the need for a family doctor and keep decisions consistent | ||
| Inefficient monitoring by insurance | ||||
| Regulation | Of course, the lack of work or good work of the health care provider should not affect the doctor's income | Non-implementation of prevention and health promotion services | Absence of some family physicians during working hours | |
| Sometimes the expected work is out of the family doctor's job description and without paying more, such as setting up 16-hour centers. | Integration of high health services in the health team and high workload that is not commensurate with the staff and time | Sometimes there is no alternative doctor | ||
| The necessity of some plans, many doctors may not want to participate in the plan | Apple system bugs | Lack of access to a family doctor during non-office hours and holidays | ||
| Free of charge services is the cause of patients' unnecessary demands | ||||
| Apple system bugs | ||||
| Reply to the doctor's consent SMS even if the doctor does not respond to the patient's unusual requests | ||||
| Heavy monitoring by the network and insurance companies | ||||
| Focus on quantitative questions in monitoring and lack of quality questions to monitor service quality | ||||
| The addition of bulky programs. The burden of programs is getting heavier day by day | ||||
| The patient's stay in the room increases due to the questions of the apple system is extensive | ||||
| High patient volume and impossibility of performing health-oriented tasks | ||||
| Behavior | Culture building and advertising about the family physician. | Inadequate training plan for health care providers | Frequent referrals to doctors | |
| People's professionalism. People think that the knowledge of a general practitioner is low | Lack of justification of general practitioners about the role of family physician | |||
| Request a referral from the people themselves | ||||
Table 2: Challenges of program implementation from the perspective of experts classified according to "health system control levers"
| Financing | Financial payments | Organizing | Regulation | Behavior |
|---|---|---|---|---|
| Further studies on project costs | Implementation of a new payment plan (Authors' suggestion: DRG) | Do more studies, such as studying the benefits of a family doctor's health services | Designing a model for people to intervene in health services; designing a model for cross-sectoral coordination | Ongoing health team training: Health team training on health information system |
| Develop a new financing model (with the ability to adapt to economic conditions) | Attention to improvement of the referral system:Coordinate the three levels of service delivery by requiring subspecialists and hospitals for accepting referrals and sending feedback | Amending the rules and regulations related to the family doctor | Educating family physicians about clinical medicine guides and non-clinical skills guides | |
| Consolidation of insurance and full insurance coverage | Using the private sector in the referral system and making private hospitals accountable to the referral system | Consistency of decisions and policies | Training of general practitioners by reviewing the general medicine curriculum in accordance with the goals of the family physician and / or setting up a family physician training course for physicians who will become family physicians | |
| Redesigning a plan for comprehensive health services with the participation of all stakeholders | Training and education of nurses and midwives in accordance with their nature and job performance in the family physician team | |||
| Establishing a coherent and efficient health information system for evidence-based decision making |
Table 3: Suggestions categorized by "health system control levers".
After extracting the main and sub-classes obtained from the interviewees' descriptions in the challenges and suggestions section, it seemed that the five main extracted classes are very similar to the five health system control levers mentioned by professor Xiao. [12] Therefore, the extracted main classes were named by the names of these five control levers.
The suggestions are expressed in Table 3 in the form of health system control levers.
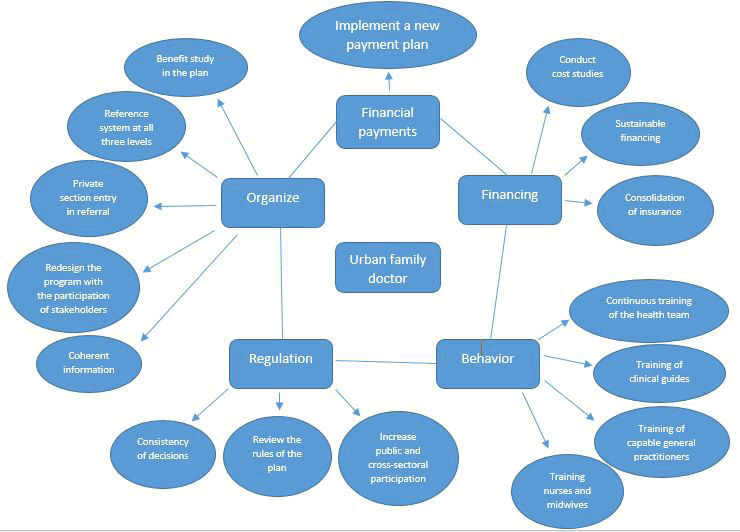
By drawing a network of extractive codes, the native proposed model of the urban family physician was drawn in the form of 5 main codes and 15 sub-codes [Figure 1].
Discussion
Based on the findings of the present study, the achievements of the project in all four groups were jointly to reduce health costs and increase access to services. Nasrollahpour et al. reported in their research that increasing people's access to health services has been a result of the implementation of the urban family physician plan. [9]
Research by Torabi et al. revealed that the temporal and spatial access of people to services has increased with the implementation of the family physician program. In this study, the reduction of treatment costs is also one of the desirable results of the implementation of the family physician plan. [13]
Increasing the number of diagnoses in urban society is one of the achievements of the plan, especially the increase in the number of diagnoses in hypertension and diabetes was one of the issues raised from the perspective of family physicians. Diagnosis and follow-up and monitoring of patients will reduce the complications of the disease and reduce disabilities and increase the quality of life, and the importance of diagnosis in non-communicable diseases is not hidden from anyone. [14]
The possibility and increase of employment for family physicians and health care providers was expressed in the view of both groups of service providers (family physicians and health care providers), which was especially important for young physicians and newly graduated midwives, as in previous studies. Increasing the number of diagnoses in urban society is one of the achievements of the plan, especially the increase in the number of diagnoses in hypertension and diabetes was one of the issues raised from the perspective of family physicians. Diagnosis, follow-up and monitoring of patients will be capable of reducing the complications of the disease, reducing disabilities and increasing the quality of life. The importance of diagnosis in non-communicable diseases is not hidden from anyone. [14]
The possibility of increasing employment for family physicians and health care providers was expressed in the view of both groups of service providers (family physicians and health care providers), which was especially important for young physicians and newly graduated midwives, as stated in previous studies. Coverage of the urban population and improvement of the physical structure of comprehensive urban health service centers are some of the achievements of this project. In the study of Kabir et al. the improvement of physical resources, the improvement of medium level and the provision of desirable services were reported as the achievements of this project. [1] Looking at the extracted codes, it can be seen that the number of challenges expressed is more than the achievements and the service recipients had less challenges in the plan than the service providers, which can be associated with more satisfaction of the service recipients from the plan compared to the providers. Mafton et al. reported that service recipients had a higher level of satisfaction than service providers.
The participants of the family physician plan stated that the non-implementation of the plan in all insurance funds and the non-insurance of physicians were among the challenges of implementing the program.
In the view of health care providers, the uncertainty and lack of serious obligation of health care providers to be insured has caused some health care providers not to be insured by physicians as employers. From the point of view of experts and staff officials, the financing of the project by the insurance system has created a problem for the insurance itself and for the service providers.
Poor cooperation of insurance companies and unwillingness of insurance companies to pay part of the project budget have also been mentioned in other studies. The family physicians participating in the study mentioned several problems in financial payments, which were classified into 5 sub-categories. There seems to have been no satisfaction with the payments. There was also this dissatisfaction among health care providers, which was due to the lack of separation of the health care provider from the relevant family physician. Physicians' dissatisfaction with the current payment system has been reported in other studies. [13]
One of the challenges posed by family physicians was the problems of the referral system, including the lack of feedback from Level 2 and the lack of private sector involvement with the referral system. It seems that the family physician plan, of which the referral system is one of the most important pillars of this plan, has only been implemented at level one so far. We know that the implementation of the referral system can be capable of the reducing unnecessary costs and improving patients' access to specialized treatments.
Nasrollahpoor et al. study showed that only 40% of the patients referred to level 2 used the referral system. Obstacles to establishing a favorable referral system from Palmer's point of view are insufficient skills of personnel, poor quality of service delivery at the level of a transportation problem, high cost of services and lack of medicine. Tawfik et al. stated that an excellent referral system is not possible without a strong link between primary health centers and hospitals.
Challenges of the project from the perspective of health care providers include the high volume of electronic records and the employer role of physicians (as an obstacle to teamwork in terms of payment and non-division of labor between physician and health care provider). The high volume of referrals and other system problems caused the care information to be recorded in the system by health care providers at another time, and they complained about the constant presence behind the computer. This issue has also been expressed in the study of Caldera et al.
From the point of view of family physicians, the request for measures outside the defined service package without paying more wages, such as setting up centers with 16-hour work in COVID-19 pandemic and increasing the volume of programs, has prevented them from providing health services. Najafi et al. also noted the high burden of patient referrals by service providers.
Free service has been identified as a cause for unusual patient demands. Dissatisfaction response to the physician's consent SMS is also stated if the physician does not respond to the patient's unusual requests such as a reverse referral. Torabi et al. considered the free services as one of the problems of the payment system in the family physician program and the reason for the increase in unnecessary demands from patients, which was in agreement with our study. Heavy monitoring by the network and insurance, focus on quantitative questions in monitoring and lack of quality questions for monitoring the quality of services were also raised by family physicians.
In the study of Kabir et al., the monitoring of the plan of the family physician was considered to be desirable. Of course, the evaluation performed in this study was an external evaluation. Apple system problems such as web problems, widespread apple system questions increased the patient's stay in the room and increase the waiting time of other clients. The problems of the apple system have been expressed in different studies from different points of view. For example, data entry into the system took time, resulting in a lack of time to treat other patients. The reason for requiring data entry into the system has been performance appraisal and payment for registered information.
The lack of a replacement physician and the lack of access to a family physician during non-office hours and holidays were considered as challenges and one of the weaknesses of this plan from the point of view of service providers.
Among the issues raised by family physicians are the lack of culture-building about family physicians and the specialization of the people, and the lack of trust in the knowledge of general practitioners, which leads to requests for referrals from the people themselves. These cultural issues, which were among the sub-codes of the study, could be one of the important reasons for the shortcomings of the referral system in this design. Inadequate training of health care providers and general practitioners regarding this plan is also one of the issues that have been addressed in other studies as well as in this study. Lack of training of physicians and health care providers on the role of family physicians in this plan can be the most important cause of many of the challenges of this plan. Of course, the role of educating and informing the people should not be overlooked.
After about 9 years from the beginning of the family physician program in Mazandaran province, the information obtained from the implementation of this plan can be used to evaluate the indicators and consequences of the implementation of the program for producing evidence.
Finally, it is proposed to reform the existing program in the field of financing with sustainable financial resources, Furthermore, implementation of a new payment strategy, and a referral system at all three levels of health services in the public and private sectors are of great importance. Providing solutions for more public participation, the participation of other organizations with the support of policy makers of this plan and developing a suitable educational system for improving the performance of the health team regarding the family physicians should also be among the goals of changing this system.
An important limitation of this study was the lack of physical presence of experts predicted due to the COVID-19 pandemic, which created problems in scheduling data collection. Another limitation of this study was that this study was not performed in fars province as one of the two provinces implementing the urban family physician program.
Acknowledgments
The authors would like to thank the National Center for Strategic Research in Medical Education for its financial support of this project and the Secretary of the House of Transformation and Innovation of the Vice Chancellor for Education and Health of Babol University of Medical Sciences for their full support of this research. This study has been approved by the Committee for Macro-Plans of Healthy Areas in the National Center for Strategic Research in Medical Education (No. 972920).
Conflict of Interest
The authors declare that there is no conflict of interest.
References
- Park K. Park's textbook of preventive and social medicine. Jabalpur. 20th ed. 2009.
- Shirvani SDN. Implementing a family physician program in Iran: Achievements and challenges. J Babol Univ Medical Sci. 2014;16:15-26.
[Crossref], [Google Scholar]
- Sans CM, Pujol RE, Gene BJ, Pasarin RMI, Iglesias PB, Casajuana BJ. Family medicine attributes related to satisfaction, health and costs. Fam Pract. 2006;23:308-16.
[Crossref], [Google Scholar], [Indexed]
- Roberts M, Hsiao W, Berman P, Reich M. Getting health reform right: A guide to improving performance and equity: Oxford university press. Oxford Scholarship Online.2008.
[Crossref], [Google Scholar]
- Torabi AA, Hosseini S, Nadia O, Mirzaee S. Study perception, knowledge and expectations from population and physicians points of view about implementation of family physician program: A case study in Shiraz. J Iran Med. 2015.
[Crossref], [Google Scholar]
- Omidvar S, Aghajani DM. Employment status of midwifery graduates of babol university of medical sciences. ACECR. 2004;4:1-11.
[Crossref], [Google Scholar]
- Mehrolhassani MH, Jafari SM, Poorhoseini SS, Yazdi FV. The challenges of implementing family physician and rural insurance policies in Kerman province, Iran: A qualitative study. Health and Development Journal. 2012;1:193-206.
[Crossref], [Google Scholar],
- Hafezi Z, Asqari R, Momayezi M. Monitoring performance of family physicians in Yazd. TOLOO-E-BEHDASHT Journal. 2009;8:1-26.
[Crossref], [Google Scholar]
- Tawfik AMK, Abdul Aziz FAA, Khwaja MS A. Patterns of referral from health centres to hospitals in Riyadh region. Eastern Mediterranean Health Journal. 1997;3.
[Crossref], [Google Scholar]
- Kaskaldareh M, Najafi L, Zaboli R, Roshdi I. Explaining the barriers and deficiencies of a family physician program based on electronic health record: A qualitative research. Tolooebehdasht Journal. 2021;20:12-26.
[Crossref], [Google Scholar]
- Najafi L, Faraji A. Satisfaction survey service providers and recipients of health care insurance program for rural and city families Tuyserkan. Seminar of Hamandishi. 2008.
[Crossref], [Google Scholar]
- Abedi G, Marvi A, Soltani KSA, Abedini E, Asadi AM, Safizadehe CK, et al. SWOT analysis of implementation of urban family physician plan from the perspective of beneficiaries: A qualitative study. Majallahi Danishgahi Ulumi Pizishkii Mazandaran. 2017;27:79-93.
[Crossref], [Google Scholar]
- Damari B, Vosoogh MA, Rostami GN, Kabir MJ. Evaluation of the urban family physician and referral system program in fars and mazandran provinces: History, achievements, challenges and solutions. 2016;14:17-38.
[Crossref], [Google Scholar]
- Golalizadeh E, Amir EM, Ahangar N. The challenges of second level referral of family physician program. MJIRI. 2011;29:309-21.
[Crossref], [Google Scholar]




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.