Fever of Unknown Origin: A Case of Post Obstructive Pneumonia Complicating Mature Teratoma
- *Corresponding Author:
- Dr. Devki Nandan
Department of Pediatrics, Dr. RML Hospital, New Delhi, India.
E-mail: devkinandan2002@yahoo.com
Citation: Bhatt GC, Nandan D, Sen A, Kanaujia P. Fever of unknown origin: A case of post obstructive pneumonia complicating mature teratoma. Ann Med Health Sci Res 2013;3:461-3.
Abstract
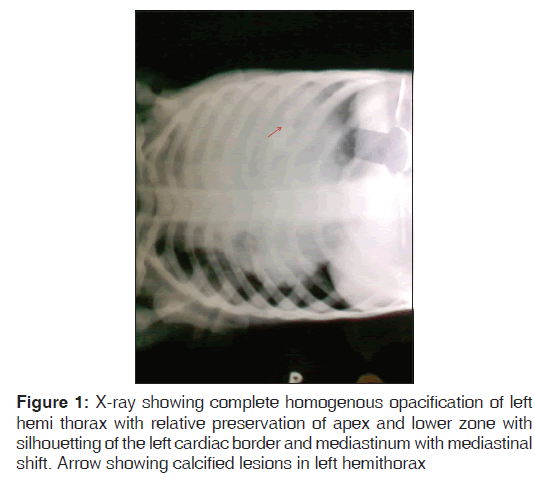
Mediastinal teratomas are rare germ cell tumors in children accounting for only 4.3% of all germ cell tumours. Here, we describe a three year old child who was misdiagnosed as a case of pulmonary tuberculosis at periphery despite of his chest X ray showing large homogenous opacification of left hemithorax with areas of calcifications and subsequently diagnosed as a case of benign mature teratoma with post obstructive pneumonia. Our case highlights the need for careful evaluation of chest X-ray (CXR) by the treating physicians, especially when CXR had a large homogenous opacity with shifting of mediastinum and presence of a few calcified shadows, which may clinch a rare diagnosis of an uncommon disorder.
Keywords
Left hemithorax, Mediastinal and Mature teratoma, Post obstructive pneumonia
Introduction
Mediastinal teratomas are rare germ cell tumors in children accounting for only 4.3% of all germ cell tumours.[1] Mature teratomas are neoplasms composed of tissues foreign to the site where they occur and typically had components derived from two or more embryonic layers. Patients with mediastinum tumours are usually asymptomatic (53%), and their masses are usually discovered incidentally on chest radiography.[2] Here, we describe a three year old child who was misdiagnosed as a case of pulmonary tuberculosis at periphery despite of his chest X ray showing large homogenous opacification of left hemithorax with areas of calcifications and subsequently diagnosed as a case of benign mature teratoma with post obstructive pneumonia.
Case Report
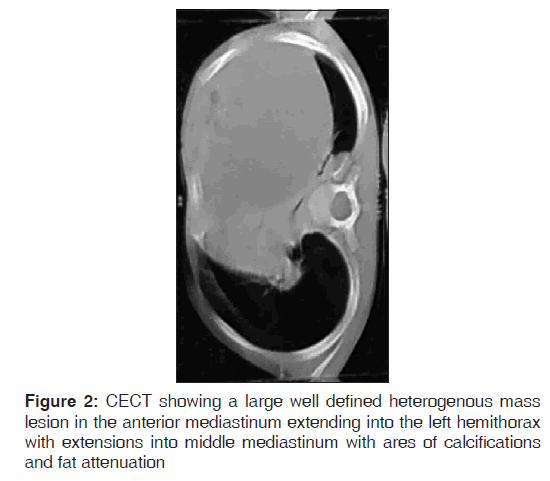
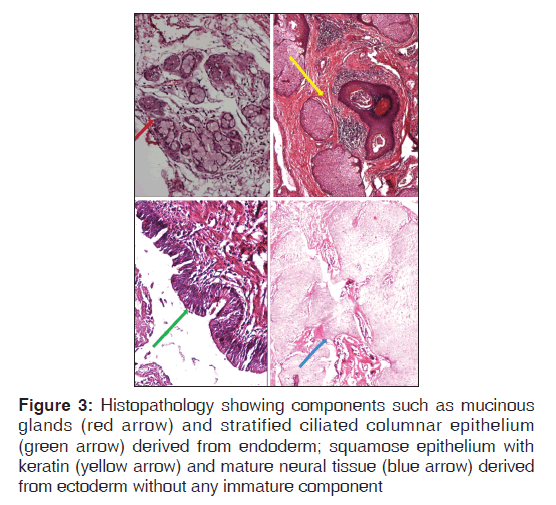
A three year old child presented with fever and cough for last one and a half months, respiratory distress and chest pain from last seven days. Prior to admission patient received 10 days of antibiotics and three weeks of adequate anti‑tubercular drug without significant improvement. There was no history of cyanosis, choking episodes, feeding difficulty, noisy breathing, swelling over the body, ear discharge, abnormal movements, headache, vomiting or urinary complaints. Examination revealed febrile child with heart rate of 130, respiratory rate of 50/min, blood pressure of 92/58 mm of mercury with mild pallor. Respiratory system examination showed right trail sign with minimal sub costal retractions with findings localized to left side of the chest such as diffuse bulge, decreased chest movements, decreased vocal fremitus, stony dull note, diminished breath sounds and vocal resonance. In cardiovascular system examination apex was shifted 2.5 cm medial to left midclavicular line. Rest of the examination was normal. Investigation revealed, hemoglobin of 10.7 gm %, total leukocyte count of 11,600/mm (Polymorphs of 52, Lymphocytes of 42) and ESR‑63. Liver function test, kidney function test, blood culture was negative and Chest X‑ray showed large almost complete homogenous opacification of left hemi thorax with relative preservation of apex and lower zone along with few areas of calcifications [Figure 1]. Contrast Enhanced Computed Tomography (CECT) of the chest was advised which showed a large well defined heterogeneous mass lesion is seen lying predominantly in the anterior mediastinum which was extending into the left hemithorax with extensions into middle mediastinum and areas of collapse consolidation in left lower lobe [Figure 2]. The lesion shows predominantly cystic component and centrally few irregular nodular, coarse calcifications as well as few areas of fat attenuation along with irregular soft tissue component seen in the center suggestive of mature teratoma. Patient underwent surgery and a 10 × 8 × 12 cm multiseptate cyst with areas of calcifications and solid tissue containing hairs and bone was resected out. Histopathology showed components such as mucinous glands and stratified ciliated columnar epithelium derived from endoderm; squamose epithelium and mature neural tissue derived from ectoderm without any immature component [Figure 3]. Alpha fetoproteins, lactate dehydrogenase and beta human chorionic gonadotropins were normal. The child was discharged and is well on two years follow up.
Discussion
A large percentage of mediastinal tumours and cysts produce no symptoms and are found on an incidental chest radiograph or other imaging study of the thorax performed for an unrelated reason.[3] Constitutional symptoms (e.g., weight loss, fever, malaise, vague chest pain) commonly occur with malignant tumours, but can be rarely observed in some benign tumours as well. Case report of mediastinal teratoma presenting as bronchopneumonia and pulmonary abscess are reported by Fuenmayor, et al. in two children.[4] Reports of mature teratoma simulating organized empyema in children have been reported by some authors.[5,6] Teratomas can get infected from contiguous foci in the lung parenchyma or via the bloodstream.[7] In our case as there was no obvious cause of fever, cough, breathlessness, chest pain and CECT chest showed areas of consolidation [Figure 2] which prompted us to consider bacterial infection of the large cystic teratoma. Patient was put on conservative treatment with intravenous ceftriaxone, following which fever, cough and chest pain subsided and complete surgical resection was done through left anterolateral thoracotomy.
Complete curative surgical removal of a mediastinal teratoma is the treatment of choice, as it establishes the diagnosis, besides preventing life threatening complications in many patients.[8] Adherent mediastinal pleura and pericardium can be dealt with by removal of the involved portions as was done in this case. As most mediastinal teratomas are benign, even a subtotal resection conserving adherent vital structures provides excellent results. In the era of modern surgery outcome is favorable.[9]
Conclusion
A benign teratoma may sometime behave as empyema or pneumonia or sometimes behave as its malignant counterpart. Our case highlights the need for careful evaluation of CXR by the treating physicians, especially when CXR had a large homogenous opacity with shifting of mediastinum and presence of a few calcified shadows, which may clinch a rare diagnosis of an uncommon disorder.
Source of Support: Nil.
Conflict of Interest: None declared.
References
- Tapper D, Lack EE. Teratomas in infancy and childhood: A 54-year experience at the Children?s Hospital Medical Center. Ann Surg 1983;198:398-410.
- Moeller KH, Rosado-de-Christenson ML, Templeton PA. Mediastinal mature teratoma: Imaging features. AJR Am J Roentgenol 1997;169:985-90.
- Chapman S, Robinson G, Stradling J, West S. Mediastinal abnormalities 1; Oxford Handbook of Respiratory Medicine (International Edition); Oxford: Oxford University Press; 2nd Impression 2008. p. 171-2.
- Fuenmayor-M CE, Garc�a RM, G�mez D, Quintiliani-Gamboa M, Altamiranda C. Mediastinal cystic teratoma. Review of two cases. Invest Clin 2007;48:509-14.
- Nmadu PT. I nfected teratodermoid tumour of the mediastinum. Ann Trop Paediatr 1992;12:225-7.
- Greif J, Schwarz Y, Sperber F, Jurgenson U. Benign cystic teratoma simulating organized empyema. Pediatr Pulmonol 1997;23:310-3.
- Meena GL, Jindal G, Rastogi R, Jindal K. A 22-year-old woman with fever, shortness of breath and chest pain. Ann Thorac Med 2009;4:4158-60.
- Verhaeghe W, Meysman M, Noppen M, Monsieur I, Lamote J, Op De Beeck B, et al. Benign cystic teratoma: An uncommon cause of anterior mediastinal mass. Acta Clin Belg 1995;50:126-9.
- Nichols CR. Mediastinal germ cell tumors. Chest 1991;99:472-9.




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.