Fine Needle Aspiration Cytology in Pediatric Age Group with Special Reference to Pediatric Tumors: A Retrospective Study Evaluating Its Diagnostic Role and Efficacy
- *Corresponding Author:
- Pasura Subbaiah Sujan Ganapathy
Centre for Vrikshayurveda, A Division of Centre for Advanced Studies in Biosciences, Jain University, Chamrajpet- 560019, Karnataka, India.
E-mail: sujan.ganapathy@gmail.com
Citation: Prathima S, Suresh TN, Harendra Kumar ML, Krishnappa J. Fine needle aspiration cytology in pediatric age group with special reference to pediatric tumors: A retrospective study evaluating its diagnostic role and efficacy. Ann Med Health Sci Res 2014;4:44-7.
Abstract
Background: Fine needle aspiration cytology (FNAC) is a well‑established diagnostic technique in adult mass lesions but a comparatively new technique to pediatric lesions. Aim: The current study aims to evaluate the role of FNAC in pediatric age with special reference to pediatric tumors. Subjects and Methods: A retrospective study of FNAC in children ≤ 18 years of age presenting with mass lesions was studied for 5 years. Distribution of cases in different age groups, sex, and site of lesion was analyzed. Pediatric lesions were categorized into non‑neoplastic, benign, and malignant conditions. Diagnostic efficacy was assessed by comparing subsequent histopathological examination wherever possible. Statistical Analysis: Epi info 07 (Centers for Disease Control and Prevention in Atlanta, Georgia (USA) 07) and values were presented as simple percentages. Results: FNAC was performed on 2903 cases in 5 years out of which 327 cases 11.3% (327/2903) were ≤ 18 years of age. Out of 327 cases, 180 cases 55% (180/327) were between 11 and 18 years. Male to female ratio was 1.15:1. The commonest site for FNAC was cervical lymph node swelling 48.3% (158/327). Reactive lymphadenitis was the commonest diagnosis among all mass lesions 38.8% (103/265), whereas Fibroadenoma 20.8% (10/49) was commonest diagnosis among benign lesions and among malignant lesions there were two cases 15.3% (2/13) each of Hodgkins and non‑Hodgkins lymphoma and one case of chondrosarcoma. The positive predictive value of diagnosing malignant lesions on FNAC was 100%. Conclusions: The ease of FNAC along with its high diagnostic accuracy makes it a desirable method for diagnosing lesions in children.
Keywords
Fine needle aspiration cytology, Histopathology, Pediatric, Tumors
Introduction
Fine needle aspiration cytology (FNAC) is a well-established diagnostic technique for evaluating mass lesions in adult patients.[1] FNAC is a safe, minimally invasive rapid procedure with good patient acceptance and low morbidity.[2] However, it has been slow in gaining popularity in pediatric patients compared with its utilization in adult patients.[1] Pediatric lesions varies from country to country and region to region. In literature, there are only few Indian studies of FNAC in pediatric population.[3-5]
Hence, this study was undertaken to review the cytomorphological spectrum of pediatric lesions in Kolar region with respect to age, sex, and site of involvement with special reference to pediatric tumors and to assess the diagnostic efficacy of FNAC.
Subjects and Methods
A total of 327 pediatric patients aged 0-18 years with palpable or deep seated lesions were included in the study period extending from January 2007 to December 2011. The cases included both inpatients and outpatients referred to the cytology section at our hospital. Ethical clearance certificate from institutional ethical committee was taken for conducting the study.
After obtaining consent from parent or guardian, routine FNAC procedure was done using 21-24 gage needle attached to 10 ml syringe by a cytopathologist or by an invasive radiologist if guided aspiration was required. Wet fixed smears in absolute alcohol were stained by Hematoxylin and Eosin, Papanicolau stain and air dried smears were stained with May Grunwald Geimsa stain. Special stains were done wherever necessary. Histopathological examination was done in 31 cases. Patients above 18 years of age and children with hematological malignancies were excluded from the study. Data was entered into a spread sheet and analyzed using Epi info 07.
Results
FNAC was performed on 2903 cases in 5 years out of which 327 cases 11.3% (327/2903) were ≤ 18 years of age. Out of 327 cases, maximum number of pediatric patients i.e., 180 cases 55% (180/327) were between 11 and 18 years [Table 1]. Male to female ratio was 1.15:1. The most common site for FNAC was cervical lymph node swelling 48.3% (158/327) followed by thyroid swelling. Ultrasonography guided aspiration was performed in six cases 1.8% (6/327). Reactive lymphadenitis was the most common among non-neoplastic lesions 38.8% (103/265) followed by acute suppurative lesion 16.22% (43/265) and colloid goiter 7.2% (19/265). Among cervical lymph node lesions, maximum cases were of reactive lymphadenitis 65.2% (103/158), followed by acute suppurative lymphadenitis 12.6% (20/158), granulomatous lymphadenitis 10.7% (17/158), and tubercular lymphadenitis 10.1% (16/158). The smears of reactive lymphadenitis showed a polymorphous population of lymphocytes and tingible body macrophages. Tubercular lymphadenitis cases were diagnosed on smears showing epitheliod granulomas in a background of necrosis, lymphocytes and presence of acid fast bacilli on Ziehl Neelsen (ZN) stain. Seventeen cases were diagnosed as non-specific granulomatous lymphadenitis where Periodic acid Schiff stain (PAS) and ZN stain showed no organisms.
| Age group (years) | Male (n=175) | Female (n=152) | Total (n=327) | |||
|---|---|---|---|---|---|---|
| Frequency | % | Frequency | % | Frequency | % | |
| ≤1 | 5 | 2.8 | 6 | 3.9 | 11 | 3.3 |
| 2‑5 | 36 | 20.5 | 14 | 9.2 | 50 | 15.2 |
| 6‑10 | 55 | 31.4 | 31 | 20.3 | 86 | 26.2 |
| 11‑18 | 79 | 45.1 | 101 | 66.4 | 180 | 55.0 |
Table 1: Age and sex distribution of study population
Among benign tumors, fibroadenoma amounted for 10 cases 20.8% (10/49) followed by lipoma 18.3% (9/49), pleomorphic adenoma (n = 4) and spindle cell tumor (n = 4).
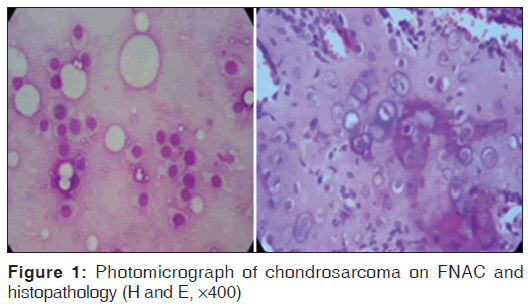
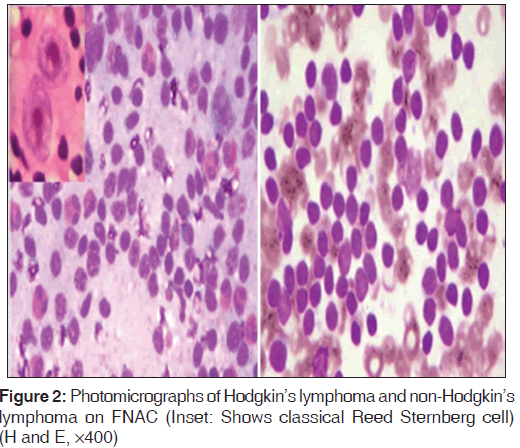
Among malignant lesions, there were two cases each of Hodgkins and non-Hodgkins lymphoma amounting to 15.3% (2/13) and one case of chondrosarcoma which were confirmed on subsequent histopathological examination. Smears from a case of chondrosarcoma showed a highly cellular smear consisting of large oval tumor cells with well demarcated eosinophilic cytoplasm against amorphous eosinophilic background [Figure 1]. Two cases of non-Hodgkins lymphoma demonstrated similar cytologic features, consisting of highly cellular samples of poorly cohesive monotonous lymphoid cells with slightly irregular nuclear membranes and inconspicuous nucleoli. Smears of Hodgkins lymphoma showed mixed population of lymphoid cells consisting of eosinophils, neutrophils and small lymphocytes and classical Reed-Sternberg cells [Figure 2].
The positive predictive value of diagnosing malignant lesions on FNAC was 100%.
Forty-nine children 15% (49/327) presented with thyroid lesions of which 38.7% (19/49) cases were diagnosed as colloid goiter, followed by 22.4% (11/49) cases of lymphocytic thyroiditis and 14.2% (7/49) cases of thyroglossal duct cyst.
Comparison of cytological and histological diagnosis was possible in 9.4% cases (31/327), the cytological diagnosis was concordant with the histopathological diagnosis in 81.6% (25/31) cases. In 19.4% (6/31) cases, there was discrepancy between cytology and histopathology diagnosis [Table 2].
| Age(years) | Sex | Cytologydiagnosis | Histopathologydiagnosis |
|---|---|---|---|
| 16 | M | Granulomatous lymphadenitis | Reactive lymphadenitis |
| 11 | F | Colloid goitre | Follicular adenoma |
| 12 | F | Reactive lymphadenitis | Granulomatous lymphadenitis |
| 14 | F | Sialadenitis | Granulomatouslymphadenitis |
| 15 | F | Thyroglossal cyst | Branchial cyst |
| 12 | F | Keratinous cyst | Infected parasitic cyst |
Table 2: Nature of cytological misdiagnosis
Discussion
FNAC has been a very popular initial diagnostic tool in evaluating both superficial and deep seated lesions in adult patients.[1] However, FNAC has received limited acceptance in pediatric cases possibly because of desire for diagnostic technique of low morbidity but high accuracy. In children, there are only few studies done mainly in head and neck lesions, lymphadenopathy, renal, and liver space occupying lesions.[3-8]
A study by Jain, et al., reported 6% of unsatisfactory aspirates and attributed them to small size of the lesions and poor handling of aspirated material, however, in the present study no unsatisfactory aspirates were obtained as repetition of the procedure was done if the first specimen was found inadequate on rapid methylene blue stain screening technique. This was supported by study done by Taylor et al.[3,9]
In a study by Maheshwari, et al., majority of cases (40.82%) were in the age group of 11-14 years, male dominated the study population (66.67%) with male:female ratio being 2:1.[10] In the present study, maximum number of patients 55% (180/327) were in the age group of 11-18 years, male preponderance was observed 53.5% (175/327) with male:female ratio of 1.15:1.
In our study the commonest site for FNAC was cervical region swelling 48.3% (158/327). Shonubi, et al., also reported similar finding in 70% (14/20) cases.[11]
In the present study, the commonest cytopathological finding among cervical lymph node lesions was reactive lymphadenitis in 38.8% (103/158), followed by suppurative lymphadenitis 12.6% (20/158), granulomatous lymphadenitis in 10.75% (17/158) and tubercular lymphadenitis in 10.1% (16/158). Annam, et al., also noted that the most common cytopathological finding as reactive lymphadenitis in 58.08%, followed by granulomatous lymphadenitis and tubercular lymphadenitis in 30.55% and 29.01% respectively.[12] Tuberculosis is still one of the leading cause of cervical lymphadenopathy in India. Diagnosis of tuberculosis in lymph nodes can be established by demonstrating acid fast bacilli in FNA smears with ZN stain or Auramine-rhodamine stain, mycobacterial culture or by amplification of bacterial DNA by polymerase chain reaction. But, the cost, time required and frequent negative results are important limitations.[13] In 17 cases of granulomatous lymphadenitis, the etiological agent was not identified.
In our study, one case of reactive lymphadenitis was falsely diagnosed as granulomatous lymphadenitis on FNAC as the endothelial cells were misinterpreted as epitheliod cells. Two cases of granulomatous lymphadenitis, one case of parasitic cyst, branchial cyst, and follicular adenoma were missed on cytology due to lack of representative sample. Ultrasonography guided FNAC improves the accuracy of FNAC diagnosis because of representative samples and radiological correlation.
Fibroadenoma 20.8% (10/49) formed the majority among benign tumors in our study. Maheshwari et al., noted soft tissue tumors (64%) were predominant among benign tumors.[10]
The largest malignant group was formed by lymphomas (25.1%), followed by small round cell tumors (21.3%), and Wilms’ tumor (12.6%) in a study by Maheshwari et al.[10] In the present study, there were two cases each of non-Hodgkin’s lymphoma and Hodgkin’s lymphoma 15.3% (2/13) and one case of chondrosarcoma. Earlier study by Mobley et al., has shown the predictive value of cytologically malignant FNAC to be 89.4% whereas in the present study it was 100%.[14]
To conclude, FNAC is a safe and cost-effective procedure with good patient acceptance, no essential morbidity and can be used as an initial screening tool in superficial and deep seated lesions in pediatric age group. Although, the number of cases with histopathological correlation was less, the role of FNAC as an initial investigative procedure is undisputed, because of its high diagnostic accuracy.
References
- Saad RS, Singh HK. Silverman FJ. Fine needle aspiration cytology. In: Orell SR, Sterett GF, editors. 5th ed. Pediatric Tumors. New Delhi: Churchill Livingstone Elsevier Ltd.; 2012. p. 445-67.
- Rapkiewicz A, Thuy Le B, Simsir A, Cangiarella J, Levine P.Spectrum of head and neck lesions diagnosed by fine-needle aspiration cytology in the pediatric population. Cancer 2007;111:242-51.
- Jain M, Majumdar DD, Agarwal K, Bais AS, Choudhury M. FNAC as a diagnostic tool in pediatric head and neck lesions. Indian Pediatr 1999;36:921-3.
- Dey P, Mallik MK, Gupta SK, Vasishta RK. Role of fine needle aspiration cytology in the diagnosis of soft tissue tumours and tumour-like lesions. Cytopathology 2004;15:32-7.
- Khan RA, Wahab S, Chana RS, Naseem S, Siddique S.Children with significant cervical lymphadenopathy: Clinicopathological analysis and role of fine-needle aspiration in Indian setup. J Pediatr (Rio J) 2008;84:449-54.
- van de Schoot L, Aronson DC, Behrendt H, Bras J. The role of fine-needle aspiration cytology in children with persistent or suspicious lymphadenopathy. J Pediatr Surg 2001;36:7-11.
- Iyer VK. Role of fine needle aspiration cytology in management of pediatric renal tumors. J Ind Assn Paediatr 2007;12:116-9.
- Bakshi P, Srinivasan R, Rao KL, Marwaha RK, Gupta N, Das A, et al. Fine needle aspiration biopsy in pediatric space-occupying lesions of liver: A retrospective study evaluating its role and diagnostic efficacy. J Pediatr Surg 2006;41:1903-8.
- Taylor SR, Nunez C. Fine-needle aspiration biopsy in a pediatric population Report of 64 consecutive cases. Cancer 1984;54:1449-53.
- Maheshwari V, Alam K, Jain A, Agarwal S, Chana RS. Diagnostic utility of fine needle aspiration cytology in pediatric tumors. J Cytol 2008;25:45-9.
- Shonubi AM, Akiode O, Salami BA, Musa AA, Ntele LM. A preliminary report of fine- needle aspiration biopsy in superficially accessible lesions in children. West Afr J Med 2004;23:221-3.
- Annam V, Kulkarni MH, Puranik RB. Clinicopathologic profile of significant cervical lymphadenopathy in children aged 1-12 years. Acta Cytol 2009;53:174-8.
- Raviglione MC, O’Brien RJ. Tuberculosis. In: Longo DL, Kasper DL, Jameson J, Fauci AS, Hausen SL, Loscalzo J, et al. editors. Harisson’s Principles of Internal Medicine. 18th ed. New York: McGraw-Hill; 2012. p. 1340-59.
- Mobley DL, Wakely PE Jr, Frable MA. Fine-needle aspiration biopsy: Application to pediatric head and neck masses. Laryngoscope 1991;101:469-72.




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.