Hot Hypertonic Saline and Compression Device: A Novel Approach in Preventing Severe Hemorrhage during Extirpation of Deep Vascular Malformations of the Face
- *Corresponding Author:
- Dr. Uche Mgbeokwere
Department of Oral and Maxillofacial Surgery, UNTH, Enugu, Nigeria.
E-mail: uchemgbos@yahoo.com
Abstract
Background: Hemorrhage is a serious challenge in vascular malformations (VMs). This problem makes the surgical excision of the lesions difficult and sometimes impossible. Objective: The objective was to design a technique that will meet with the challenges of hemorrhage while performing surgery in such lesions in our environment. Patients and Methods: Seven patients with deep and moderately large VMs of the facial region were selected and treated with hot 7.5% hypertonic saline after compressing the feeder vessels. This was then complemented with surgical excisions. Results: There were successful surgical extirpations of the lesions without eventful hemorrhage. Conclusion: Hot 7.5% hypertonic saline injected into VMs after emptying their hematic content caused sclerosis of the anomalous vessels. This made bleeding during surgery uneventful.
Keywords
Compression device, Hot 7.5% hypertonic saline, Minimal blood loss, Surgery, Vascular malformations
Introduction
The incidence of patients with vascular anomalies is increasing, but finding surgeons to care for them may be difficult.[1] This is because the surgical removal of these lesions is often accompanied by hemorrhage that can be overwhelming and difficult to abate. Many specialties, including oral and maxillofacial surgery, have fashioned out different techniques that are directed at treating these lesions without the embarrassing event of massive hemorrhage. These methods include conservative treatment with circumferential ligation of the feeder vessels[2] and tobacco pouch suture technique of strangling superficial lesions of the lip.[3] Also, using sclerosants and embolizing agents, coagulation by laser therapy, and cryosurgery[4-7] have been variously used to achieve the same goal. In the superficial and relatively small lesions in the oro-facial region, these techniques may suffice alone without some other complementary procedures. This may not be the case in relatively large and deep lesions. Therefore, in moderately large and deep-seated lesions such as the ones encountered in our centers, there was a need for a more encompassing technique that would not only collapse and obliterate the abnormal blood vessels to avoid undue hemorrhage, but also extirpate the fibrosed moderately large tissues. The solution was found in hot 7.5% hypertonic saline and compression of the vessels with complementary surgery. In this paper, the seven cases treated with this method have been presented.
Patients and Methods
A total of seven patients who presented to us with seven vascular malformations (VMs) in the cheek and/or adjacent regions in the face were selected for this treatment and injected with hot 7.5% hypertonic saline after compressing the feeder vessels with compression devices secured at the periphery of the lesions. Patients whose lesions were discrete enough to be isolated within the embrasure of our compression device and were easy to achieve complete local anesthesia of the region were selected. Patients with lesions that occurred straddled on both sides of the face, with intervening healthy tissues between them, or lesions that occurred in more than one location on in the same region of the face were excluded. The patients were seen and treated either at Pilgrims Dental Clinic, Enugu, or Imo State University Teaching Hospital, Orlu, between September 2006 and March 2009. They were one male and six females in the age range of 14–37 years. Five patients had the lesion in the cheek [Table 1]. The cheek lesions were all in the lower third of the face and were circumscribed or dome shaped. They measured about 7 cm in diameter. The lesions were deep seated between the buccinator and facial muscles. The sixth patient had the lesion on the right side of the face, and this extended from the right half of the upper lip, including the cheek and the infra-orbital region. The seventh patient had the lesion in the chin–lip region and the swelling obliterated the lower labial sulcus. There were three different sites where the lesions were located and these were designated as lower-third, middle-third, and chin-lip regions of the face, respectively [Table 1].
| Sex | Age (years) | Duration of swelling (years) | Site |
|---|---|---|---|
| F | 24 | 4 | Left lower-third of face |
| F | 37 | 6 | Right lower-third of face |
| F | 22 | 8 | Right lower-third of face |
| M | 14 | 7 | Right mid-face |
| F | 16 | 10 | Chin–lip region |
| F | 25 | 3 | Left lower-third of face |
| F | 19 | 3 | Right lower-third of face |
Table 1: Biodata of patients, duration and sites of lesion on the face
The chief complaints in all the patients were persistent swelling and cosmetic disfigurement. The diagnoses were based mainly on clinical findings. Consistency on palpations was firm or rubbery. All the patients have had the lesions for a period between 3 and 10 years.
Needle on syringe aspirations yielded blood in all the cases. There was bruit on auscultation in four lesions and these four patients also had pulsatile vessels within the masses. Blood pressures and hematological indices in all the patients were normal. Angiography and ultrasonography were, however, not available. The diagnoses were based mainly on clinical findings. Histopathology results were not consistently available, but in three patients where they were available, they were contributory to the diagnoses. Patients or parent, in the case of a minor, gave consent before commencing the treatments. All the patients were injected with hot 7.5% hypertonic saline sclerosant after compressing the feeder vessels with compression devices and emptying the hematic contents. They were operated on the seventh day.
Compression device and sclerosant injection technique
Skin maps of the lesions were made with alcohol-based marker to isolate their locations on the skin, ensuring a distance of about 1 cm border away from the periphery of the swellings. The marked borders signified the sites for the placement of the compression devices. The skin and the deeper tissues were then infiltrated with 2% xylocaine with 1:80,000 adrenaline along the marked borders. It was ensured that the lesions including the adjacent tissues were adequately anesthetized. Then, following Popescu’s[8] ligation method, sutures were passed around the borders using strong nylon or silk sutures (1/0 size). Care was taken to ensure that deep cuts were made while passing the needles through the tissues so as to capture the deeper soft tissues including the feeder vessels. Several complementary intraoral ligations were also made where applicable so as to tie off more vessels that were associated with the lesions.[3]
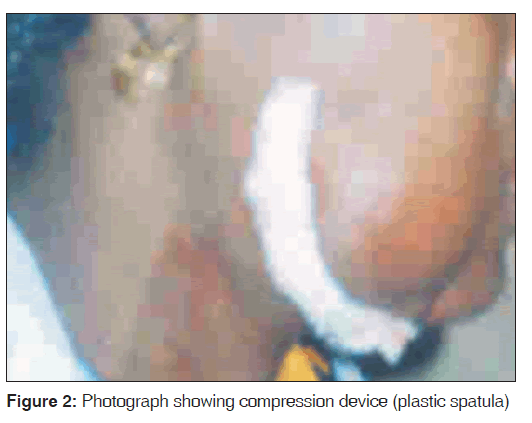
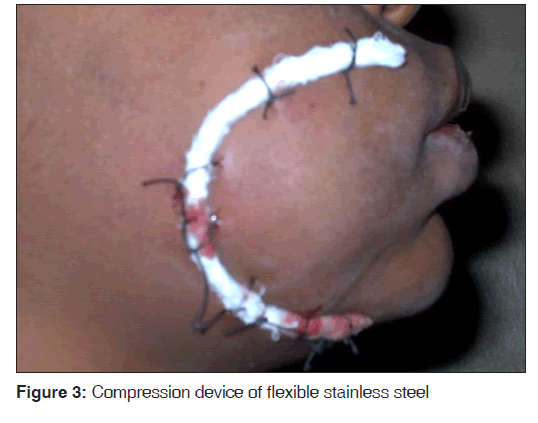
Figure 1 shows preoperative photograph of one of the patients with cheek lesion. Round plastic spatula of about 10 mm in diameter was softened in hot water and carefully kneaded to conform with the marked border of the lesion. The kneaded plastic spatula was then padded/bolstered with gauze and then secured on the border with the sutures. The sutures were secured as tight as possible over the compression device to compress or occlude the underlying vessels [Figures 2 and 3].
Later experiences included flexible stainless steel bars of similar diameter to the spatula because of the difficulty of kneading the plastic in hot water. The flexible stainless steel metal bar were found to be easily adjustable and it was easy to achieve the purpose [Figure 3].
After compressing the feeder vessels with the compression devices and ligation, blood was aspirated from the lesions with needle on syringe. This was followed by injecting into the lesions hot 7.5% hypertonic saline of equivalent volume of blood aspirated from the lesions. The hot hypertonic saline reached boiling point before injecting into the lesions. The patients were left for 5 days under antibiotics and analgesic cover before removing the skin sutures and the compression devices. Surgical extirpation of the lesions was done on the seventh day through the intraoral route.
Results
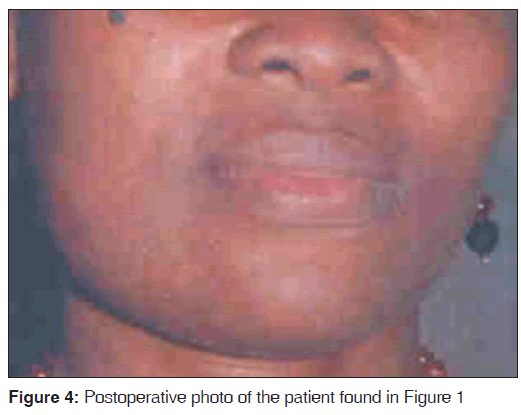
On palpation of the hitherto soft and compressible masses, hard swellings were found on the third day. Surgical extirpation of the lesions on the seventh day was associated with minimal hemorrhage and there was no need for blood transfusion in each patient. There were no suture or compression device marks found in the patients during the 1-month postoperative visit [Figure 4]. The five patients with lesions limited to the cheek and the patient with chin–lip lesion had complete resolution of their lesions during the 1-month postoperative visit. However, the patient whose lesion involved one side of the upper lip, cheek, and infraorbital region received a second operation under general anesthesia through an extra-oral approach. At the second month recall visits, only one patient was seen and the result was still satisfactory [Figure 4].
Discussion
Sclerotherapy is a procedure used to treat VMs including those of lymphatic system.[9] A wide range of chemicals in liquid or foam form have been used over time to perform this function. Usually the liquid is injected into the vessels and this makes them shrink or involute over time.
The use of hot or boiling water is not a novel concept in the management of VMs. Boiling water and warm hypertonic saline solutions have been variously used by Obuekwe et al.[10] and Oji et al.[3] in treating VMs. Water is bland, so also is saline. However, hot water and hot hypertonic saline release heat energy that causes disruption of the intima and eventually collapse and blockage of the channels in the anomalous angiomatous tissues. In our study 7.5% hot hypertonic saline sclerosant was used because small volume of 7.5% hypertonic saline solution is known to maintain intravascular volume in hypovolemic resuscitation and this does not easily escape from the intravascular space.[11-13] The 7.5% hot hypertonic saline in these treatments was, therefore, expected to be retained in the targeted vessels. The heat from the hot sclerosant destroyed the anomalous vascular tissues because it was retained longer in the sinusoids/caverns. More than boiling water, boiling saline retains heat energy which can adversely affect the vascular endothelial tissues and this leads to necrosis and obliteration of the vessels’ lumina. A certain amount of heat usually disrupts the endothelial linings of blood vessels and this usually promotes coagulation of blood and death of the vessels.[14] This explains our choice of 7.5% hot hypertonic saline. The sclerosis and obliteration of the lesions were evidenced by the change in their consistencies.
Compression of the vessels with ligatures and compression device was a presurgical complement that was aimed at controlling the blood flow in the lesions during sclerotherapy. The occlusion of the vessels further prevented the dilution of the sclerosant by the hematic volume in the lesions. A great hematic volume could otherwise mix with the sclerosant, cause self-dilution,[15] and obviously cause dissipation and loss of heat energy. The compression of the vessels also prevented reflux of the sclerosant and its escape into the systemic volume which could inflict some systemic upset. The ligation method has been reported by a number of authors to be effective in starving vascular lesions of blood and consequently strangled them.[2,3,8]
The compression devices were padded with gauze to protect the skin from abrasive injuries. The skin could easily be injured if allowed to make direct contact with the metal or plastic devices. Such abrasive injuries could cause unesthetic skin mark.
Aspiration of blood from the lesions emptied or reduced the volume of blood in their sinusoids or caverns and this further predisposed the endothelial linings of the vessels to direct contact with heat. This culminated in the disruption and collapse of the abnormal tissues and set the stage for their extirpation without abnormal hemorrhage and probable recourse to blood transfusion.
One of the patients who had lip, cheek, and infra-orbital lesion had a second surgery apparently due to the extensive size of his lesion. After the first operation, it was observed that there were remnants of the lesion around the infraorbital area and it was decided to tackle it through extra-oral route under general anesthesia. To avoid the failure of clearing these lesions at the first operation under local anesthesia, patients with extensive lesions had been excluded from the list of patients for these procedures. It was felt that poverty was responsible for the poor follow-up visits by the patients.
Considering the scarce resources in our disposal, the use of certain standard investigative tools to aid our work was utopia. For instance, angiography and magnetic resonance imaging, if available, would have aided us in identifying the feeder vessels and determining the extent of the mass, while duplex ultrasound would have been useful in guiding the injection of the hot sclerosant into the targeted malformed tissues. None of these was at our disposal.
Nevertheless, the compression and sclerosant method was able to occlude and seal off the vessels, and with this, it became possible to achieve the desired goal.
Conclusion
Compression of the vascular supply to the lesions obviously reduced their blood flow. Injecting the hot hypertonic saline caused sclerosis and obliteration of the vessels’ lumina. This patho-physiological event addressed the challenges of massive blood loss that these vascular lesions would have been associated with. The end-point of this process was the uneventful surgical extirpation of the lesions. This simple method of compression of vessels and sclerosant, complemented with surgery, can be used to take care of patients who have moderately large, deep-seated vascular anomalies in the facial region, even when sophisticated equipment are not available. The clinicians in centers with deficient facilities are advised to give this technique a trial.
Source of Support
Nil.
Conflict of Interest
None declared.
References
- Cheng V. Treatment of venous malformations, Klippel-Tenaunay Syndroms and other low-flow lesions. Ezine articles. http://ezine articles.com. Treatment of venous malformations. [Last accessed on 2011 Mar 28].
- El Abdin H, Zokair H. Hemangioma of the tongue: A conservative treatment with circumferential ligation. Saudi Dent J 1998;10:18-22.
- Oji C, Chukwuneke FN, Mgbor N. Tobacco-Pouch suture technique for the treatment of vascular lesions of the lip in Enugu, Nigeria. Br J Oral Maxillofac Surg 2005;44:245-7.
- Kaji N, Kurita M, Oraki M, Takushina A, Harii K, Narushina M, et al. Experience of sclerotherapt and embolosclerotherapyusing ethanolamine oleate for vascular malformations of the head and neck. Scand J Plast Reconstr Surg Hand Surg 2009;43:126-36.
- Schwarz DN, Kellman BM, Cacayorin ED. Treatment of a lingual haemangioma by super selective embolization. Arch Otolaryng Head Neck Surg1986;112:96-8.
- Bradley PF. A review of the use of the neodymium YAG laser in oral and maxillofacial surgery. Br J Oral Maxillofac Surg 1997;35:26-35.
- Bradley PF. The cryosurgery of bone in the maxillofacial region. In: Cryosurgery of the Maxillofacial Region. In: Bradley PF, editor. Vol. 11. Florida: CRC Press; 1985. p. 55-91.
- Popescu V. Intratumoral ligation in the management of orofacial cavernous haemangioma. J Maxillofacial Surg 1985;13:99-107.
- Wikipedia. The true encyclopedia. http://en.wikipedia.org/ wiki/sclerotherapy. [Last accessed on 2011 Mar 28].
- Obuekwe ON, Ojo MA, Akpata O, Saheb BD. Haemangioma of the maxillofacial region in Benin City, Nigeria. Ann Biomed Sci 2002;1:18-2.
- Freudenberg S, Palma P, Schuster K, Mkony C, Waschke K. Small volume resuscitation with 7.5% hypertonic saline solution – Treatment of haemorrhagic shock in the tropics. MERA. Trop Doct 2003;33:165-6.
- Kreimeier U, Bruckner UB, Niemezyk S, Messmer K. Hyperosmotic saline dextran for resuscitation from traumatic-haemorrhagic hypotension: Effect on regional blood flow. Circ Shock 1990;32:83-99.
- Vassar MJ, Fischer RP, O’Brien PE, Bachulis BL, Chambers JA, Hoyt DB, et al. A multicenter trial for resuscitation of injured patients with 7.5% sodium chloride – the effect of added dextran 70. Arch Surg 1993;128:1033-13.
- Ketan RB, Sunny S, Shahid MN. Histrory of bipolar coagulation. Neurrosurg Rev 2006;29:93-6.
- Cabrera J, Redondo P. Sclerosing treatment of vascular malformations. An Sist Sanit Navar 2004;27 Suppl 1:117-26.




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.