Human Bite among Children
Citation: Ali AF, et al. Human Bite among Children. Ann Med Health Sci Res. 2018;8:1-3
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Bites inflicted by humans are often more serious than those inflicted by animals. A wide range of secondary consequences have been documented in the medical literature. The most common location was face and only 18%over hands and few cases reported in scrotum. Human bite wound presents a challenge to any emergency department given the many issues involved in their management. Here we report 1-year boy bitten in the scrotum by another boy of same age. The majority of infected human bite contain mixed organism. We also report current guidelines in management of human bite.
Keywords
Human bite; Children; Scrotum
Introduction
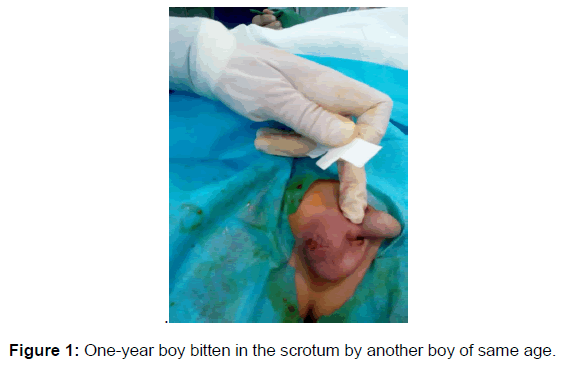
One-year-old boy was bitten by his younger brother on the right side of the scrotum. The boy had no past medical issue and both immunized for his age. The bite was nearly L-shaped clean lacerated deep wound measuring 3 cm, exposing testis partly. Suturing was done in layers; intra-operatively testis showed good colour with no breach in tunica layer and wound edges were clean. The wound was washed repeatedly with saline and diluted betadine-operatively one dose of piperacilline and tazobactam then continued two doses post-operatively with syrup for 5 days. Amoxicillin with clavulanate acid patient was followed up after 2 weeks, wound healed completely with no evidence of infection [Figure 1].
Discussion
Approximately 10-15% of human bite wounds become infected owing to multiple factors. The bacterial inoculum of human bite wounds contain as many as 100 million organisms per millilitres and are made up of as many as 190 different species. Many of these are anaerobes that flourish in the low redox environment of tartar that lie between teeth or in areas of gingivitis. [1] Human bites accounts for relatively low percentage 3% of the total bite encountered in the ED, but thy have the potential for severe morbidity due to challenges in identifying the injuries and late presentations complicated by established infection. The majority of infected human bite contain mixed organism, streptococcal species mostly alpha-hemolytic Streptococci frequent isolates from human bite wound. Anaerobic bacteria are commonly found in all types of infected bites.
Children aged 15-17 months had the highest overall injury rate before 15 yrs. This coincides with developmental achievements such as independent mobilities, exploratory behaviour and had to mouth activity. Compared with peers without disabilities children with disability are at a significantly higher risk of injury. [2]
The rate of infection after human bite is 10-30%. Streptococcus Sep. May cause serious infection, such as necrotising fasciitis. [3] Other species staphylococcus epidermidis and penicillinase producing staphylococcus aureus are the most common bacteria. Human bite to the scrotum is rare and can be associated with high morbidity rate if poorly managed. [4]
Human bite wound presents a challenge to any emergency department given the many issues involved in their management. In addition to local wound infection other complications may occur including lymphangitis, local abscess, septic arthritis, teno- synovitis and osteomyelitis. Rare complications include endocarditis, meningitis, brain abscess and sepsis with disseminated intra-vascular coagulation especially in immunecompromised individual. [5]
Children are not just small adults, their physical and cognitive abilities, degree of dependency need for supervision, activities and risk behaviours all change rapidly with their growth. As children develop their curiosity and with to explore the world increase significantly while they only have limited capability to understand and respond to danger. Children development and behaviour are therefore highly associated with injury risk. [6] It’s a way young children express anger, frustration and need for control and attention before thy have the words to do so says clinical psychologist Stanlay Goldstein. [7] Although evidence based practice guidelines have not been developed bite wounds warrant an organized standardized approach to care to help prevent complications. Such approach involves first eliciting a history of the circumstances surrounding the bite and patient medical history. Next basic bite wound care should be performed, including cleaning and irrigation of the wound. A good understanding of bite wound bacteriology and the situations in which antibiotics may be indicated is important. [8]
The following actions to reduce the infection risk associated with biting may include following [9]
• Take a history from parents to assess the blood born virus risks in children who bite repeatedly.
• Consider offering tests and possible immunization against hepatitis in children who bites repeatedly.
• Consider individual plans for children who bite repeatedly bite involving parents and the child GP.
• Agree a policy for immunizing teaches at risk for hepatitis-B.
• Consider immunity of classmates at school entry.
• Ensure staff wears long sleeved clothing if caring for a child who bites regularly.
Universal prophylaxis with antibiotics is not recommended. The comprehensive meta-analysis of Medeiros et al. in Cochrane database yielded no evidential basis for a reduction of infection rate by prophylactic antibiotics, except for bite wounds on the hand on hands.
Despite the poor state of evidence, most expert recommend early antibiotic treatment for three to five days for fresh, deep wounds and wounds in certain critical bodily areas (hands, feet, areas near joints, face and genitals) for persons at elevated risk of infection and for persons with implants e.g. artificial heart valve. In contrast, antibiotics need not be given if the patients 24 hrs or more after the bite and there are no clinical signs of infection.
Targeted antibiotic treatment is given for manifest bacterial infections.
Its varieties include:
• Aminopenicilline +a beta -lactamese inhibiter (oral/intravenous)
• Piperacilline /tazobactam (intravenous)
• carbapenem (IV)
• possibly moxifloxacilin +clindamycin
In case of penicillin allergy
Recommended duration of antibiotic treatment
• cellulitis or abscess one to two weeks
• Tenosynovitis two to three weeks
• Osteomyelitis, arthritis three to four weeks [10]
Infection rate of punctured wounds and wounds greater than 3 cm was 1.5 times higher than for all wounds. Total infection rates within 24 hrs antibiotic administration was 29.3% compared to 65%, <48 hrs and 81% <72 hrs. [11] If the bite appears to be consistent with human bite, the question typically asked by child protective services in whether the bite was caused by an adult or a child. In general, the most common guidelines are that the normal inter-canine distance of an adult is 2.5-4 cm. Any human bite marks with inter-canine distance more than 3 cm is most likely inflicted by an adult. [12]
Human bite injuries carry the risk of being infected with bacteria flora of the oral cavity. This often leads surgeons to consider initial debridement and delayed closure because of the fear of wound infection. Prophylactic antibiotic treatment and primary closure of bite wound remains controversy. Opinion tilt towards the fact that primary surgical repair is the treatment of choice for most clinically uninfected facial bite wounds, whereas delayed closure should be reserved for certain high risk or already infected wounds. [13]
Conclusion
Although rare, human bites have been shown to transmit clostridium tetani. According to the recommendation of the US centres for disease control and prevention (CDC) tetanus immune globulin and the 3-dose vaccine series should be administered to patients with an unknown tetanus vaccine history or those who have received fewer than 3 doses. For patients with a history of 3 or more doses of tetanus and diphtheria vaccine who received a booster less than 5 yrs ago, no tetanus booster is required
Acknowledgements
All authors disclose that there was no conflict of interest.
REFERENCES
- Barrett J. Human bites. Medscape, 2017.
- Agran PF, Anderson C, Winn D. Trent R. Pediatrics 2003; 111: e683-e692.
- Kkoe GA, Kil K, Karasalan A. Wounds 2015; 12: E20-E23.
- Kerins M, Greene S. Human bite to scrotum. European Journal of Emergency Medicine 2004; 11: 223-224.
- Brook Microbiology and management of wound infection in human and animal bite Prim care 2003; 30: 25-39.
- Shi X, Shi JX, Krista K. Unintentional injuries in children with disabilities: A systemic review and meta-analysis. Injury epidemiology 2015; 2: 21.
- Goldstein S. Troubled children /troubled parents the way out. Second edition. 2010.
- Tapliltz RA. Managing bite wounds. Post graduate med.2004; 116: 556-559.
- Public health England. Guidelines for the management of human bites in schools and other child care settings -2008.
- Henton J, Jain A. Cochrane corner: Antibiotics prophylaxis for mammalian bit J. Hand sur EUR Vol 2012; 37: 804
- Jaindl M. The Central European Journal of Medicine 2015.
- Kellong ND. American Academy of paediatrics committee on child abuse and neglect evaluation of suspected child physical abuse. Paediatrics 2007; 119: 1232-1241.
- Peter B, Antonia O. Management of human bites on the face. Afr. Health Sci. 2007; 7: 50-54.




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.