Pattern and Presentation of Tongue Lesions in Kaduna, Nigeria: A 10 Year Review
2 Surgery Department, Jos Unversity Teaching Hospital, Jos, Nigeria
3 Dental and Maxillofacial Surgery Department, University of Calabar Teaching Hospital, Calabar, Nigeria
4 Dental and Maxillofacial Surgery Department, State house Clinic, Abuja, Nigeria
5 Department of Anesthesia, Ahmadu Bello University, Teaching Hospital Zaria, Nigeria
Citation: Fomete B, Agbara R, Osunde OT, Bello SA, Yunus AA, Goni BAM. Pattern and Presentation of Tongue Lesions in Kaduna, Nigeria:a 10 Year Review. Ann Med Health Sci Res. 2017; 7:157-161
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Introduction: The tongue is a complex of muscle groups with a fibrous scaffold consisting of the hyoglossal membrane and midline lingual septum and covered by epithelium. The musculature of the tongue is separated into intrinsic and extrinsic groups. The tongue may be involved with lesions similar to those in other parts of the oral cavity, or as an oral manifestation of systemic diseases. Materials and Methods: A retrospective study of all consecutive patients that presented with tongue lesions at the Oral and Maxillofacial Clinic of the Ahmadu Bello University Teaching Hospital, Zaria between January 2006 and December 2014 was undertaken. The data were analyzed using Statistical Package for Social Sciences (SPSS) version 13, Illinois USA. Results: A total of 93 patients presented with tongue lesions within the years reviewed. There were 51 males and 42 females giving a male to female ratio of 1.2:1. Carcinoma of the tongue was the commonest lesion accounting for 18/93 (19.35%) of all the cases. This was followed by ankyloglosia and trauma with 12.9% (12/93) each. Condylomas and hemangiomas had the least frequency. Conclusion: A vast variety of tongue lesions were seen in the present study.
Keywords
Maxillofacial Surgery, Tongue lesions, Orofacial structures, Carcinoma, Metastasis
Introduction
The tongue is a complex of muscle groups with a fibrous scaffold consisting of the hyoglossal membrane and midline lingual septum and covered by epithelium. The musculature of the tongue is separated into intrinsic and extrinsic groups [1,2]. It is the most motile and accessible organ in the oral cavity and performs many functions like swallowing, sucking, phonation and perception of sensations such as thermal changes, taste, pain stimuli and general sensations, as well as development of the jaws and orofacial structures [2,3]. These functions may be affected by changes in the oral cavity environment or by lesion affecting the tongue, impacting greatly on the patients’ quality of life [2].
The tongue may be involved with lesions similar to those in other parts of the oral cavity, or as an oral manifestation of systemic diseases. However, certain lesions are confined exclusively to the tongue and these may include fissuring, median rhomboid glossitis, and atrophy of the epithelium, hairy and geographic tongue among other [2].
The dorsal surface of tongue is peculiar in that it contains large number of specialized epithelial structures, also known as the papillae with many of the exclusive tongue lesions believing to arise from these papillae. Moreover, the extreme mobility of the tongue and its rich supply of sensory nerve endings make the tongue particularly liable to minor trauma and functional disability, with the resulting damage being rapidly brought to the notice of the patient [2].
it was observed that the tongue may be targeted by a wide range of pathological conditions, the recognition of which may be helpful in the early diagnosis of some systemic disorders, including those of allergic or hormonal origin, where the tongue lesions may be the first clinical sign of the disorder [2].
The aim of the present study is to analyze various lesions of the tongue seen over an eight- year period in a Nigerian tertiary health care facility.
Patients and Methods
A retrospective study of all consecutive patients that presented with tongue lesions at the Oral and Maxillofacial Clinic of the Ahmadu Bello University Teaching Hospital, Zaria between January 2006 and December 2014 was undertaken. Information was sourced from patients’ case notes and theatre records. Data collected included age, sex, site of lesion, type of lesion as well as histopathological report. The data were analyzed using Statistical Package for Social Sciences (SPSS) version 13, Illinois USA and the results presented as frequencies and percentages for categorical variables and continuous variables presented as mean and standard deviation. Verbal consent was obtained from the patients for used of photographs
Results
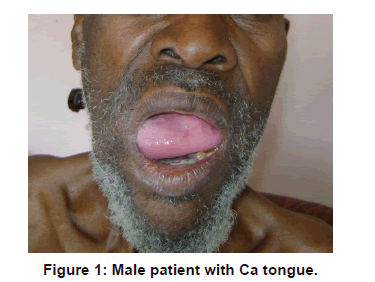
A total of 93 patients presented with tongue lesions within the years reviewed. There were 51 males and 42 females giving a male to female ratio of 1.2:1. Carcinoma of the tongue [Figure 1] was the commonest lesion accounting for 18/93 (19.35%) of all the cases. This was followed by ankyloglosia and trauma with 12.9% (12/93) each. Condylomas and hemangiomas had the least frequency [Table 1].
| Lesions | No of patients | % |
|---|---|---|
| Ca tongue | 18 | 19.35 |
| Trauma | 12 | 12.9 |
| Ankyloglossia | 12 | 12.9 |
| Ulcer | 9 | 9.67 |
| Geographic tongue | 6 | 6.45 |
| Harmatoma | 4 | 4.30 |
| Pyogenic Granuloma | 4 | 4.30 |
| Neurological Disorder | 3 | 3.22 |
| Fissured tongue | 3 | 3.22 |
| Coated tongue | 3 | 3.22 |
| Macroglossia | 3 | 3.22 |
|  Squamous papilloma | 3 | 3.22 |
| Lymphangioma | 2 | 2.15 |
| Cystic lesion | 2 | 2.15 |
| Adenocystic Ca | 2 | 2.15 |
| Condyloma | 1 | 1.07 |
| Diffused small cell lymphoma | 1 | 1.07 |
| Pigmented | 1 | 1.07 |
| Fibroma | 1 | 1.07 |
| Hemangioma | 1 | 1.07 |
| Kaposi Sarcoma | 1 | 1.07 |
| NFL | 1 | 1.07 |
| Total | 93 | 100 |
Table 1: Distribution and prevalence of various tongue lesions.
Majority (33.3%, 31/93) of patients in this study was in the first decade of life, followed by patients in the 3rd decade of life (12.9%, 12/93) [Table 2]. The 2nd and 5th decades were equally represented with 11.8% (11/93) each. Trauma induced tongue lesions had its highest occurrence in children (first decade), while Ca tongue occurred more frequently in adult patients (6th decades and above) [Table 2]. All the cases of ankyloglosia presented in children (first decade of life). The presentation of the other tongue lesions according to age is shown in Table 2.
| Lesion | 0-10y | 11-20 | 21-30 | 31-40 | 41-50 | 51-60 | 61-70 | 71-80 | 81-90 | Total |
| SCCa | 1 | 2 | 2 | 5 | 2 | 5 | 1 | 18 | ||
| Traum | 8 | 3 | 1 | 12 | ||||||
| Ulcer | 3 | 3 | 1 | 2 | 9 | |||||
| GT | 3 | 1 | 2 | 6 | ||||||
| L/G | 2 | 2 | ||||||||
| H/G | 1 | 1 | ||||||||
| Harm | 1 | 1 | 1 | 1 | 4 | |||||
| M/G | 2 | 1 | 1 | 4 | ||||||
| Ank/g | 12 | 12 | ||||||||
| NFL | 1 | 1 | ||||||||
| Fibrom | 1 | 1 | ||||||||
| PG | 1 | 1 | 1 | 1 | 4 | |||||
| SP | 2 | 2 | ||||||||
| Condyl | 1 | 1 | ||||||||
| Pigm | 1 | 1 | ||||||||
| Fissur | 1 | 1 | 1 | 3 | ||||||
| Coated | 1 | 2 | 3 | |||||||
| ACC | 1 | 1 | 2 | |||||||
| Kaposi | 1 | 1 | ||||||||
| DSCL | 1 | 1 | ||||||||
| Cyst | 2 | 2 | ||||||||
| Neuro | 2 | 1 | 3 | |||||||
| Total | 31 | 11 | 12 | 10 | 11 | 7 | 4 | 6 | 1 | 93 |
Table 2: Age distribution of the lesions.
Table 3 shows the gender distribution of tongue lesions. Ca tongue was slightly more in males (10/93; 10.8%) than in females (8/93; 8.6%). Similarly, more tongue lesions due to trauma were more frequently observed in males (7/93; 7.5%) than in females (5/93; 5.4%). In contrast, pyogenic granuloma were more females (3/93; 3.2%) than in males (1/93; 1.1%) [Table 3].
| Lesions | M | F | Total |
|---|---|---|---|
| Ca tongue | 10 | 8 | 18 |
| Adeno cystic | 2 | 2 | |
| Kaposi | 1 | 1 | |
| Geographic tongue | 4 | 2 | 6 |
| Squamous papilloma | 2 | 1 | 3 |
| Pyogenic granuloma | 1 | 3 | 4 |
| Harmatoma | 4 | 4 | |
| Lymphangioma | 2 | 2 | |
| Hemangioma | 1 | 1 | |
| Condyloma | 1 | 1 | |
| Diffused small cell lymphoma | 1 | 1 | |
| Trauma | 7 | 5 | 12 |
| Ulcer | 6 | 3 | 9 |
| Neurological disorder | 3 | 3 | |
| Fissured tongue | 1 | 2 | 3 |
| Coated tongue | 2 | 1 | 3 |
| Cystic lesion | 1 | 1 | 2 |
| Pigmented | 1 | 1 | |
| Fibroma | 1 | 1 | |
| Macroglossia | 1 | 2 | 3 |
| Ankyloglosia | 8 | 4 | 12 |
| NFL | 1 | 1 | |
| Total | 51(54.8) | 42(45.2) | 93 |
Table 3: Sex distribution of various tongue lesions.
Discussion
The tongue is considered a mirror which may reflects the general health status of the human body and its disorders could result from local causes or as a manifestation of systemic disease [2].
The result of the gender distribution of this study, while it contrasts that of Sura Ali Fouad [2] who had more females than males, agrees with those of Patil et al. [3] that found more males than females with tongue lesions in their study.
In the present study, Ca tongue (19.35%) was the commonest lesion encountered followed by trauma and ankyloglosia. This was different from the result of a previous study from India, where coated tongue (28.0%) dominated followed by geographic tongue (16.4%) [3]. In Iraq Ulcers (24.6%) were the commonest followed by atrophy of papillae (14.6%) [2], while in America vascular/ lymphatic lesions (26.6%) predominated [4].
The prevalence of Ca tongue (19.35%) was by far greater than the 0.3% and 7.7% in both Indian and Iraqi population [2,3].
Ca of the tongue is regarded as a biologically different entity compared to cancer affecting other oral sites. It is more aggressive and generally associated with a higher rate of metastasis. It commonly involves the mobile tongue i.e., anterior two-thirds of the tongue, lateral borders followed by dorsum. It may arise de novo or from an existing leukoplakia or irritation from a sharp tooth or prosthesis. In our cases none of the patients gave a history of trauma or used prosthesis. It is clinically silent as there is laxity of the tissue planes separating the intrinsic tongue musculature, which helps cancer cells to spread easily and becomes symptomatic only when tumor size interferes with tongue mobility [5].
Cancer of the tongue is the second most common type of cancer arising in the upper digestive tract, with approximately 40% arising from the tongue base. In addition, lesions located in the base of tongue are more likely to be malignant (85%) than those located in the oral tongue (20%). Most tongue cancers (more than 95%) are histologically characterized as squamous cell carcinoma; adenocarcinoma of the tongue, often arising from minor salivary glands, occurs in fewer than 2% of all tongue malignancies [6].
Risk factors for squamous cell carcinoma include older age, tobacco use, and alcohol use. Intraoral squamous cell carcinoma commonly involves the lateral surface of the tongue. Patients younger than 40 years who develop intraoral squamous cell carcinoma often do not have risk factors. Initially, lesions appear as a slight thickening over a red or white base. This may lead to nodularity or ulceration, causing pain and discomfort. Biopsy is critical to confirm the diagnosis and allow for prompt treatment before extensive local invasion occurs. Treatment typically requires surgery and radiation therapy [7]. About 90% of our patients were referred for radiation therapy.
The prevalence of trauma was 12.9% which was higher than the 4.8% and 1.6% in Indian and Libyan populations respectively [3]. Injuries to the tongue are seen as lacerations or ulcerations and are caused by physical, chemical and thermal injury, the most common causes being physical. Injuries may result from accidental biting while talking, sleeping, secondary to mastication, self-induced by patients or secondary to seizures.
In addition to these causes, fractured, carious, malposed or malformed teeth and premature eruption of teeth, poorly maintained and ill, fitting dental prosthetic appliances may cause trauma [3,5]. The major cause in this study was road traffic accident followed by bite. Treatment is largely based on the withdrawal of agents causing the injury, trimming sharp teeth, correcting the prosthetic appliance, stopping intake of caustic chemicals or drugs. A soft diet should be advised along with appropriate analgesics and topical anesthetics. Sipping ice cold water every few minutes will reduce the thermal injury. Soft mouth guard may be given to the patients. Oral hygiene should be maintained using saline mouthwashes to prevent secondary infections [5].
Oral ulceration including tongue ulceration especially traumatic ulcer was the commonest finding, because the tongue is moving frequently during speech and eating, moreover recurrent aphthous ulceration considered the second most common oral ulcerative lesion, both ulcers can occur in any age without gender predilection, while leukoplakia, neoplasms, lingual varicosities commonly occur in old age [2]. The prevalence of ulcers was 9.67% which is higher than the 1.8% and 1.6% in the Indian and Libyan populations [3,8].
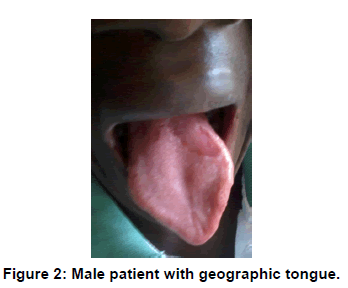
The prevalence of geographic tongue [Figure 2] in this study was 6.45% which was lower than the 6.8% in Jordan, 10% in Iraq, 16.4% in India, 21% and 17.4% in Brazil and Libya respectively [2,3,9]. The results of the present study was higher than the 4.8% previously reported in the Jordanian population [10], 0.6% in the American population [11] and 1.6% in the South African population [12]. Patil et al. [3] in his review of the literature reported a high female preponderance but this study had more male (4, 66.7%) than female (2, 33.3%), and this agreed with those of Voros-Balog et al. [13] who had more male than females. Geographic tongue is associated with spontaneous remission and recurrences. No treatment is usually required; symptomatic lesions may be treated with topical corticosteroids [5].
Ankyloglossia or tongue-tie is a congenital developmental anomaly that limits tongue protrusion due to an abnormally short lingual frenulum [7]. The prevalence of ankyloglosia in various studies has been estimated to be 0.1% to 3.7% [3,14]. Ankyloglosia (12.9%) in this study was higher than the previously reported values [3].
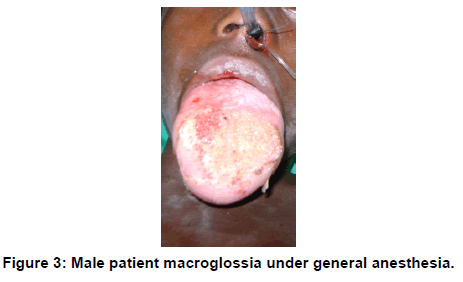
Macroglossia [Figure 3] is the abnormal enlargement of the tongue in relation to the jaws and the oral cavity. It is associated with Down’s syndrome, tuberculosis, sarcoidosis, hypothyroiddism, amyloidosis, multiple myeloma, neurofibromatosis, infection and allergic reaction [3]. The prevalence of macroglossia in the present study was 3.22% which is much higher than that reported in Indian and Turkish populations [3,15] (Ugar-Cankal et al. and Patil et al. All our patients had excision. This condition causes problems in feeding, breathing, swallowing, normal jaw development. It interferes with teeth positioning and causes malocclusion and hence the lateral borders of the tongue show scalloping corresponding to the spaces between teeth and gingival [5].
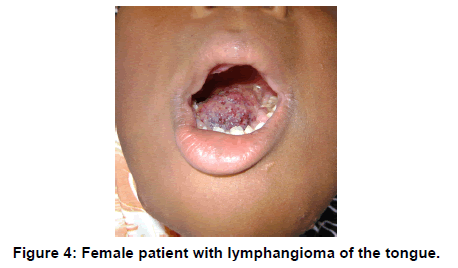
Fibroma due to chronic irritation, can be differentiated by excisional biopsy. Our study recorded 1.07%. Hemangioma also was 1.07% and lymphangioma [Figure 4] 2.15%. These values were higher than 0.3% in Indian populations [3] who however had no case of lymphangioma but lower than 26.6% in America [4]. Also, neurofibrolipoma and Condyloma were 1.07% respectively in this study while harmatoma represented 4.3%. This was far lower than the 13.3% of Kreiger et al. [4] and while all their patients were children, only one out of the four in this study was a child (4 years).
Papilloma associated with human papilloma virus (HPV) is a common lesion seen in 1% individuals [7]. In this study, it constituted 3.22% which was higher than the 0.6% in India [3].
Pyogenic granuloma (PG) is a non-neoplastic inflammatory hyperplastic response which could be due to inflammation, poor oral hygiene, trauma or hormonal factors [3,5]. The prevalence in this study was 4.3% which was lower than the 6% in Iraqi population [2]. PG commonly affects females in the second decade [5]. Three (75%) out of the four patients in this group were female but the age range was second to fifth decade. The reason for the relatively higher occurrence in females may be explained in terms of the influence of females hormones. The growth of pyogenic granulomas is known to be exacerbated during pregnancy and regresses markedly postpartum. PG occurs commonly on skin and oral mucosa as smooth or lobulated exophytic hemorrhagic and compressible lesion, which is usually pedunculated but sometimes sessile. The lesion is usually asymptomatic, may grow rapidly in size and may vary in size from few millimeters to centimeters [5]. This was the experience in our cases some were misdiagnosed for malignancy. These lesions are treated successfully with removal of local irritants and conservative surgical excision. Latest techniques like laser, cryosurgery and electro-dissection cause less bleeding and are well-tolerated by patients with no adverse effects [5].
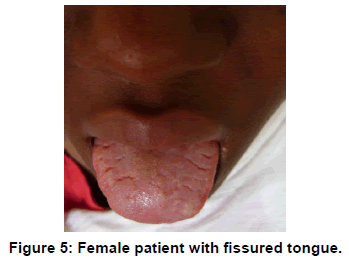
In this study, while cystic lesions represented 2.15% which was by far lower than the 16.2% of Kreiger et al. [4]. Fissured tongue constituted only 3.22%. The prevalence of fissured tongue [Figure 5] obtained in this study was lower than the 10%,14.9%, 27.3%, 48.4% in Iraqi, Indian, Brazilian and Libyan populations but higher than the 1.4% in Saudi and Turkish populations [2,3,8]. This lesion has been suggested to be genetically determined. Various contributory factors to the development of fissured tongue include hyposalivation, diabetes mellitus, candidiasis, vitamin B deficiency and lichenoid reactions [8]. With advancing age, the prevalence of fissured tongue increases. This can be explained by the fact that increasing age is associated with hyposalivation, which is one of the prime contributing factors [10]. Fissured tongue has been seen in patients with Down’s syndrome, acromegaly, psoriasis, and Sjögren syndrome. Melkersson-Rosenthal syndrome is characterized by a triad of severe fissuring, relapsing orofacial edema, and facial nerve palsy [7]. Most of the patients with fissuring of the tongue present with no symptoms; however, symptoms such as soreness with acidic food and beverages may be seen if the fissures are deep. The deep fissures act as reservoir for food particles and accumulate bacteria leading to the inflammation of the tongue [3]. No definitive treatment or medication is required. The grooves have to be maintained clean to avoid secondary infection [5].
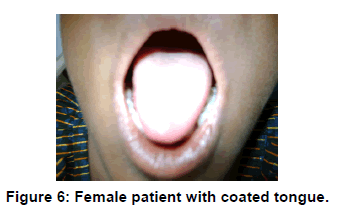
The prevalence of coated tongue [Figure 6] in the present study was 3.22% which was lower than the 9.2%, 11.0% and 28.0% in Jordan and India respectively the highest [3,9,10] but higher than the 2.1% in Turkish [1].
Conclusion
A vast variety of tongue lesions were seen in the present study, and the pattern of distribution of the lesions seen were somewhat similar to previously documented findings in the literature.
REFERENCES
- Wayne SF, Richard HW, Anna I, Bronwyn EH, Gary LH, Jason PH, et al. Primary lesions of the root of the tongue. Neurologic/Head and Neck Imaging. RadioGraphuics.2011;31.
- Sura Ali Fuoad. A clinical study on tongue lesions among Iraqi Dental Outpatients. RRJDS. 2014; 2:100-106.
- Patil S, Kaswan S, Rahman F, Doni B. Prevalence of tongue lesions in the Indian population. J ClinExp Dent. 2013;5:128-132.
- Kreiger, PA, Ernst LM,Elden LM,Kazahaya K, Alawi F, Russo PA. Hamartomatoustongue lesions in children. Abstract. Amer J SurgPathol. 2007;31:1186-1190.
- Sunil A, Kurien J, Mukunda A, Bin Basheer A, Deepthi.Common superficial tongue lesions. Indian J Clinic Pract. 2013;23:534-542.
- Market BA, Louie AV, Velker VM, Kwan KF, Franklin JH, Venkatesan VM. Adenocarcinoma not otherwise specified on dorsum of tongue: case report and literature review. Current Oncology.2012;19.
- Brian VR; Richard D; And Christopher W. Common tongue conditions in primary care. Am Fam Physician. 2010;81:627-634.
- Byahatti SM, Ingafou MSH. The prevalence of tongue lesions in Libyan adult patients. J ClinExp Dent. 2010;2:163-168.
- Darwazeh AM, Pillai K. Prevalence of tongue lesions in 1013 Jordanian dental outpatients. Community Dent Oral Epidemiol. 1993;21:323-324.
- Darwazeh AM, Almelaih AA. Tongue lesions in a Jordanian population. Prevalence, symptoms, subject’s knowledge and treatment provided. Med Oral Patol Oral Cir Bucal. 2011;16:745-749.
- Kleiman DV, Swango PA, Pndborg JJ. Epidemiology of mucosal lesions in United States school children: 1986-1987. Community Dent Oral Epidemiol. 1994;22:243-253.
- Arendorf TM, Van der Ross R. Oral lesions in a black preschool South African population. Community Dent Oral Epidemiol. 1996;24:296-297.
- Voros-Balog T, Vincze N, Bánóczy J. Prevalence of tongue lesions in Hungarian children. Oral Dis. 2003;9:84-87.
- Salem G, Holm SA, Fattah R, Basset S, Nasser C. Developmental oral anomalies among schoolchildren in Gizan region, Saudi Arabia. Community Dent Oral Epidemiol. 1987;15:150-151.
- Ugar-Cankal D, Denizci S, Hocaogglu T. Prevalence of tongue lesions among Turkish school children. Saudi med J. 2005;26:1962-1967.




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.