Prolonged Retention of Foetal Bones Following Induced Abortion as a Possible Cause of Secondary Infertility: A Case Report
2 Units of Radiology of The Light Specialist Hospital and Maternity, Nnewi, Nigeria
3 Department of Histopathology, Nnamdi Azikiwe University Teaching Hospital, Nnewi & Nnamdi Azikiwe University, Nnewi Campus, Nigeria, Email: co.ukah@unizik.edu.ng
Citation: Okafor CI, et al. Prolonged Retention of Foetal Bones Following Induced Abortion as a Possible Cause of Secondary Infertility: A Case Report. Ann Med Health Sci Res. 2017; 7: 432-434
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Objective: To create awareness of the possibility of this uncommon cause of infertility among caregivers and Teachers in Gynecology and Ultrasonography and to also emphasize the need for proper evaluation of patients with secondary infertility. Clinical Presentation and Intervention: 37-year old P 0+1 with 7 years secondary infertility and history of induced mid-trimester abortion 20 years previously. Vaginal ultrasound scan and saline infusion sonohysterography suggested retained foetal bones, which were confirmed by histology. Retained foetal bones acting like an intrauterine contraceptive device, may cause secondary infertility. Conclusion: Prolonged retained foetal bones in a case of secondary infertility. When there is a history of mid-trimester abortion, the possibility of retained foetal bones should be borne in mind.
Keywords
Foetal; Bones; Abortion; Secondary; Infertility; Retention
Introduction
The incidence of retained foetal bones was shown to be 3 out of 2000 (0.15%) diagnostic hysteroscopies done in women with abnormal uterine bleeding. [1]
The incidence is likely to be higher in countries like Nigeria with restrictive abortion laws, leading to high incidence of unsafe abortions with increased morbidity and mortality. [2]
Apart from secondary infertility, retained foetal bones may also present with irregular vaginal bleeding, dysmenorrhea, dyspareunia, chronic pelvic pain, spontaneous passage of foetal bones and vaginal discharge. [3,4] Vaginal ultrasound scan, Saline infusion Sonohysterography (SIS) and hysteroscopy are possible diagnostic modalities. [4-6]
Retention of foetal bone following abortion is not normally mentioned as a possible cause of secondary infertility during lectures and in many standard text books of Gynecology. Consequently, this knowledge gap created low awareness of this condition among clinicians.
We are reporting this rare event to create awareness among caregivers especially gynecologists and ultrasonologists and to emphasize the need for proper evaluation of patients with secondary infertility.
Case Report
A 37-year-old Para 0+1, presented to our facility with history of inability to conceive for 7 years despite adequate unprotected intercourse.
She had a regular 28 days menstrual cycle with premenstrual syndrome. The husband’s seminal fluid analysis was normal.
There was a history of induced abortion of a 14-15 weeks old pregnancy when she was a student 20 years previously. There were no major post-abortal complications necessitating further intervention.
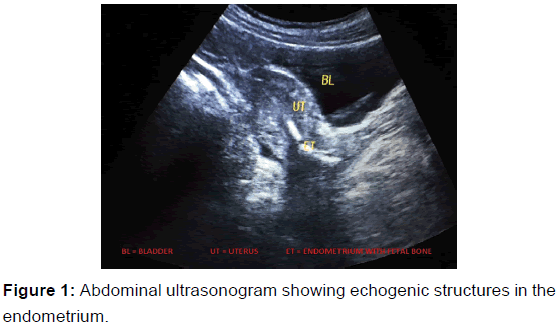
Physical examination was unremarkable. Abdominal and Transvaginal ultrasound revealed two linear echogenic structures in the uterine cavity measuring 1.5 cm × 0.34 cm and 1.1 cm × 0.3 cm [Figure 1].
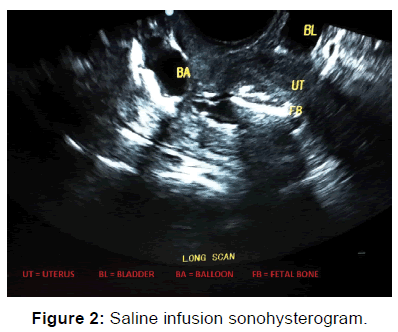
Saline infusion sonohysterography was done, [Figure 2] the structures were better elucidated. Evidence of fluid in the pouch of Douglas (which was not found during the transvaginal scan) suggested patency of at least one fallopian tube.
Following proper counseling and preparation, dilatation and curettage was done.
She observed 8 hours fasting prior to anesthesia. Misoprostol (prostaglandin E1 analogue) 400microgram was inserted into the posterior vaginal fornix to soften and possibly dilate or make dilatation of the cervix less traumatic.
The patient was placed in lithotomy position; cleaned and draped. Sims speculum was used to expose the cervix. Vulsellum forceps was used to grab the anterior lip of the cervix. Gentle curettage was done.
Plastic manual vacuum aspirator was used to complete the collection of the products. The procedure was well tolerated. The patient was discharged the same day on oral paracetamol tablets, amoxyclav and metronidazole. The pathologist’s reports are as follows
Macroscopy
Received predominantly blood clot with some grayish white soft tissue, altogether measuring 4.0 × 3.0 × 1.0 cm.
Microscopy
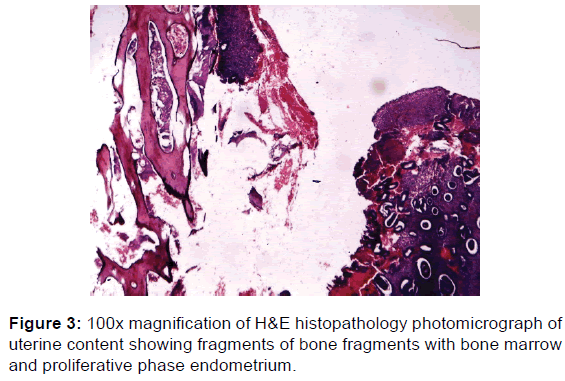
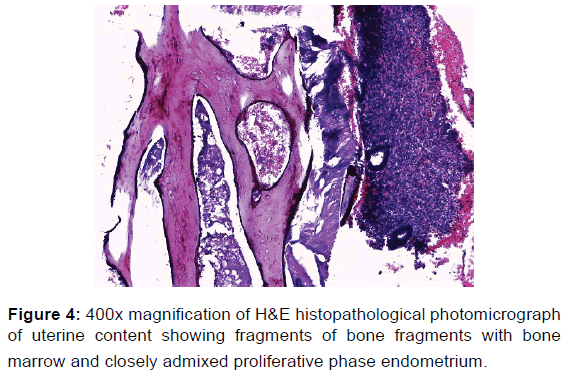
Sections of endometrial biopsies show irregular fragments of proliferative endometrial tissue admixed with dead and degenerate bone spicules, and pools of fresh haemorrhages. However, no chorionic villus, trophoblastic cell or decidual tissue is seen.
Overall features are those of retained products of conception (foetal bones).
Endometrial biopsies
Retained Product of Conception (Foetal Bone). The photo micrograms are shown [Figures 3 and 4].
The patient visited our facility last 6weeks after dilatation and curettage, and had no new complaints. She was eventually lost to follow-up.
Discussion
Complications of unsafe abortion are known to be major contributors to the etiology of infertility in developing countries. [2]
It is estimated that 97% of about 20 million unsafe abortions that take place globally every year, occur in developing countries. [7]
The incidence is so high in developing countries because of restrictive abortion laws and very low level of awareness and use of contraception. [7]
Graham O et al. of the assisted conception unit king’s college hospital London found eleven West African women (between 1989 and 1995) who had retained intrauterine bone as the cause of secondary infertility. All had termination of pregnancies in their country of origin. Following there moval of the bones eight (72.7%) conceived spontaneously. [8]
Tubal occlusion from pelvic inflammatory disease resulting from unsafe abortion and endometrial trauma (Asherman’s syndrome) are more common. Retention of foetal bones is rare. [7]
In a study on the pattern of hysterosal pingo graphic findings among women being investigated for infertility in Nnewi Nigeria, Okafor et al. found that of the 330 patients studied, 18.7% had bilateral tubal occlusion while 14.8% had endometrial adhesions, none of the patients had evidence of retained foetal bones. [9]
The patient presented had induced abortion at the age of 17 years, which was consistent with the findings in a study in Lagos, Nigeria where majority (21.7%) of those who presented with complications resulting from unsafe abortion were teenagers aged 14-19 years. [10]
Transvaginal ultrasonography has markedly improved the evaluation of pelvic pathologies without recourse to invasive procedures. The initial diagnosis of retained foetal bones in our patient was made by transabdominal and transvaginal ultrasound scan, as was reported by other workers. [2]
We carried out saline infusion sonohysterography to elucidate the lesion further. Our findings also suggested patency of at least one fallopian tube. Hysteroscopy, where the skill and equipment are available is very useful for the diagnosis and treatment of this condition. [1]
Osseous metaplasia is a rare disorder of the endometrium which may cause primary or secondary infertility. Hence, even in the absence of the history of previous pregnancy loss the condition should be suspected when a hyperecoic structure is found in the endometrium during pelvic ultrasonography. [11]
The treatment for retained foetal bone is the removal of the bone either through hysteroscopic resection or evacuation. Relief of symptoms and resumption of fertility are often dramatic. [2,3,4,8] We saw our patient last 6 weeks post treatment. In our clime where majority of the patients pay their Hospital bills out of pocket, they freely change from one facility to another. We planned to evaluate her further and to consider referral for assisted reproduction if she did not conceive after 3 cycles.
Conclusion
Complications of unsafe abortion remain important etiological factors for secondary infertility in our country. Good history and proper investigations are vital in managing these patients. When there is a history of mid trimester abortion, the possibility of retained foetal bones should be borne in mind.
Conflict of Interest
All authors disclose that there was no conflict of interest.
REFERENCES
- Makris N, Stefanidis K, Antaklis A. The incidence of retained fetal bones revealed in 2000 diagnostic hysteroscopies. Journal of the Society of Laparoendoscopic Surgeons. 2008; 10: 76-77.
- Oye-Adeniran BA, Umoh AV, Nnatu SN. Complications of unsafe abortion law reform in Nigeria. Reproductive Health Matter. 2002; 10: 18-21.
- Xiao S, Tian Q, Xue M. Infertility caused by intrauterine fetal bone retention: A case report. J Med Case Rep. 2014; 8: 177.
- Srofenyoh EK, Addison M, Dortey B, Kuffour PA. intrauterine retained fetal bones as a cause of secondary infertility. Ghana Medical Journal. 2006; 40: 105-109.
- Geeta D, Ramachandra G, Ravikanth G, Tanushree R. Retained fetal bone as a cause of post abortal failure to conceive. Int J Gynecol Obstet. 2011; 15.
- Moon HS, Park YH, Kwon HY, Hong SH, Kim SK. iatrogenic secondary infertility caused by residual intrauterine Fetal Bones after Mid-trimester Abortion. Am. J Obstet Gynecol. 1997; 176: 369-370.
- Bukar M, Geidam AD. Complications of unsafe abortion. In: Ebeigbe P. N (ed.), Foundations of Clinical Obstetrics and Gynaecology in the Tropics. International Edition. Mindex Publishing Co. Ltd. Benin Nigeria. 2015; 187-194.
- Graham O, Cheng LC, Parson JH. The ultrasound diagnosis of retained fetal bones in West African patients complaining of infertility. BJOG: Int J Gynecol Obstet. 2000; 107: 122-124
- Okafor CO, Okafor CI, Okpala OC, Umeh E. The Pattern of Hysterosalpingo-graphic findings in women being investigated for infertility in Nnewi, Nigeria. Niger J Clin Pract. 2010; 13: 264-267.
- Rabiu KA, Omololu OM, Ojo TO, Adewunmi AA, Alugo BG. Unsafe abortion in Lagos, Nigeria: A Continuing Tragedy. Niger Postgraduate Med. J. 2009; 16: 251-255.
- Madaan M, Suman S, Sharma R, Kapoor N, Garg P, Raj SS. Osseous metaplasia of the endometrium and successful hysteroscopic resection: A report of two cases and review of the Literature. Asian J Endosc Surg 2015; 8: 63-66.




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.