Radio-morphometric Analysis of Lingual Concavity for Dental Implant Placement Using Cone Beam Computed Tomography
2 Department of Diagnostic Sciences, College of Dentistry, King Khalid University, Abha, Saudi Arabia
Citation: Alqahtani NM, et al. Radio-morphometric Analysis of Lingual Concavity for Dental Implant Placement Using Cone Beam Computed Tomography. Ann Med Health Sci Res. 2021;11:1439-1444.
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Introduction: Cone Beam Computed Tomography (CBCT) offers an accurate and minimal radiation exposure technique in assessing mandibular morphological structures such as lingual concavity during implant planning and placement, which if not adequately taken care of can result in lingual plate perforation and subsequent complications.
Aim: The aim of our study was to determine the prevalence and degree of lingual concavities in the first molar region in mandibular arch to decrease chance of lingual cortical bone perforation while placement of dental implants. Methodology: A descriptive, cross sectional study was conducted on 165 CBCT images (86 males & 79 females). Mandibular morphological parameter such as ridge types, ridge width and height, angle between lingual surface and line drawn above the canal were assessed. The prevalence of each ridge typeswas determined. Analysis of variance and chi square tests were employed to detect any significant differences between genders. A p value of lesser than 0.05 was considered to be statistically significant.
Results: A total of 165 scans were evaluated with a mean age of 46.34 ± 16.55 years. The prevalence of U type mandibular ridge was 58.8%, P type at 24.2% and C type 17%. No significant relation was found in any morphological parameters between genders except Concavity angle.
Conclusion: Type U ridge morphology had the highest prevalence. Mandibular lingual concavity must be taken into account during implant placement to prevent accidental perforation of lingual plate. The CBCT provide an accurate assessment of lingual concavities.
Keywords
CBCT scan; Dental implant; Lingual concavity; Lingual cortex perforation; Radiographic evaluation
Introduction
Human anatomy is a complex structure and to achieve success in any surgical procedure detailed understanding of surrounding structure is utmost important. Dental implant placement is such a surgical procedure which allows the patient to regain the lost tooth achieves the associated function and aesthetics by the process of osseointegration. [1] Owing to its simple nature and predictable long-term success the osseo-integrated implants are gaining popularity. However, surgical accidents and complications do occur irrespective through diagnosis, treatment planning or surgery skills. [2] These can happen at the time of surgery, during healing period or even after loading of implants, severity of which depends on the degree of the damage caused and few of them may even be life threatening. [3]
The advancement in radiology has led to the development of Cone Beam Computer Tomography (CBCT), which helps in better understanding of complex anatomical structures and identifying anatomical sites with potential risks during surgeries. One such complex anatomical structure is posterior mandibular ridge which require frequent dental implant placement after loss of molar in that region. The ambiguous anatomy of this area makes it a high-risk zone and surgeons struggle area during implants placement. The assessment of this region with osteometry and /or by diagnostic cast for implant placement is difficult because myeloid muscle prevents proper evaluation of this area, which most of the time results in perforation of the lingual cortex leading to implant failure traumatisation of vital anatomical structures, neurologic injuries and arterial trauma with hematoma.[4] All this due to Lingual undercut or lingual concavity, a common occurrence in the posterior mandibular region, hence it becomes essential to monitor the angulation and positioning of implants through radiographic evaluation and clinical assessment. [5,6]
Radiographic assessment is generally done via periapical and panoramic radiographs at the implant site. However, these methods do not provide sufficient data regarding bone width as they provide two dimensional information. Cone Beam Computerised Tomography exhibits better accuracy in detection of lingual undercuts leading to better understanding and less incidence of perforation in the lingual cortex during surgery. CBCT of the mandibular jaw facilitates better visualisation of lingual concavity in the first molar region and also enhances better selection of implant fixture in terms of size, location and bucco-lingual angulation. [7] Hence, CBCT scans are favoured in implant intervention planning to prevent perforation, haemorrhage, nerve damage and subsequent infection. [8] They also have lower radiation exposure and offer the advantage of 3-dimensional imaging.
In this context, it is important to obtain through information related to lingual concavity in the posterior mandibular region which is a potential risk in implant surgery, and studies on lingual concavity in the posterior mandible are limited. The aim of this article was to study the prevalence and the degree of lingual concavity in the edentulous first molar region using cross-sectional images from CBCT scans of the mandibles.
Methodology
The present cross-sectional descriptive study was conducted at prosthodontic department, college of dentistry, King Khalid University, and was approved by the institute’s ethical committee with approval number IRB/KKUCOD/ETH/2020- 21/023. The Sample size calculation was performed with a computer software (Sample Size Calculator, Clin Calc LLC, Indianapolis, IN, USA) based on the assumption of a 2.7 ± 0.92 mm measurement for the lingual concavity depth based on a previous study with a 2-sided Alpha=0.05, Power=90%. It required 129 total participants.
Total 165 (86 males & 79 females) participants were recruited from the outpatient department, reporting for the replacement of missing first molar in the mandibular posterior region with implants. All participants were explained about the study and written consent was obtained before inclusion in the study. CBCT scans were performed on all 165 participants, involving the mandibular jaw. In order to ensure confidentiality, names of every individual whose scan was included was coded and stored separately.
CBCT Images were acquired using PaX-i3D Smart™ (Model: PHT-30LFO) make by Vatech Dental Manufacturing Ltd. Korea. Imaging parameters were 94 kVp, 8.7 mA (for adult man); 8.4 mA (for adult woman), Scan time of 18.0 second, 10 × 8.5 cm field of view (FOV) is selected as this was the maximum FOV available for multiple teeth imaging. Implant planning software program utilised was Ez3D-I by Vatech Dental Manufacturing Ltd. Korea.
The occlusal and Frankfurt planes of all subjects were kept parallel to the floor according to the device’s instructions. The CBCT images were saved as jpeg files. The radiographic evaluations were performed by chief researcher and oral maxillofacial radiologist. All the images used in the study were from the complete patient database of the clinic and were not made specifically for this paper. The inclusion criteria involved was absence of at least one mandibular first molar while the adjacent second premolar was present. The CBCT scans with poor quality images, developmental defects; trauma related morphological changes and pathological condition which could possibly alter the interest site were excluded.
The Mandibular first molar alveolar region was used as the study site of interest. The study site had to have adequate horizontal bone width of at least 3.5 mm [9] and height of 10 mm from the alveolar crestal bone to the superior border of inferior alveolar nerve canal to accommodate an implant of 8 mm. A 4 * 8 mm regular-sized implant was used as the guide to make sure that a sufficient vertical bone height of 10 mm (from the alveolar crest to the superior border of the Inferior Alveolar Nerve canal [IAN]) to place a 8 mm implant while maintain a safety distance of at least 1.5 mm. [10] A minimum of 1.5 mm distance from the IAC has been suggested by Sammartino et al. [10] to prevent injury to the IAN during implant loading, and, 2 mm zone of safety between an implant and the coronal aspect of the nerve was suggested by Greenstein. [11]
The CBCT scan were measured as per the criteria of Chan et al. [5] bucco-lingual width at 2 mm distance apical to the alveolar crest, Bucco-lingual width at 2 mm safety distance coronal to the superior border of the inferior alveolar nerve canal, Vertical height of the mandible, Vertical height above safety distance from inferior alveolar nerve to the alveolar crest, Concavity angle in degrees, determined by the constructed line from apical lingual point to the most prominent point of lingual overhang of jaw, Concavity depth from the deepest point of the concavity, to the most prominent point of the lingual overhang.
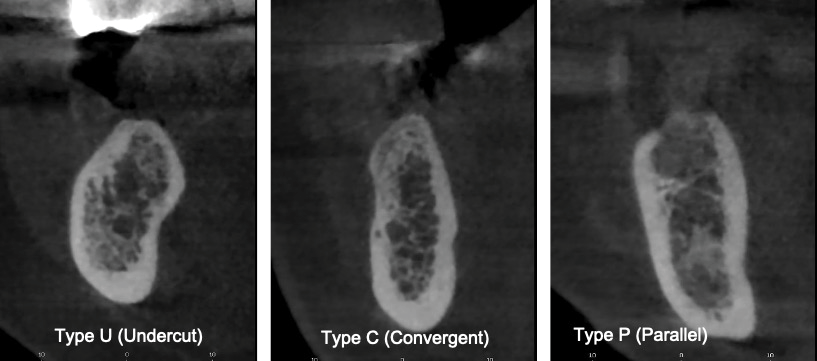
The shapes of the mandibles were classified into 3 types (types U, C, or P) using the cross-sectional images of the edentulous region based on Chan et al. [3] study [Figure 1]. U- Undercut type, where in concavity angle and depth were used for measuring lingual concavity. It was defined as ridge base narrower than the alveolar crest and presence of lingual undercut. Type C or convex type was defined as ridge base wider than the alveolar crest, without any obvious lingual undercut. Type P or parallel type was defined as the parallel form of the ridge, without any obvious lingual undercut.
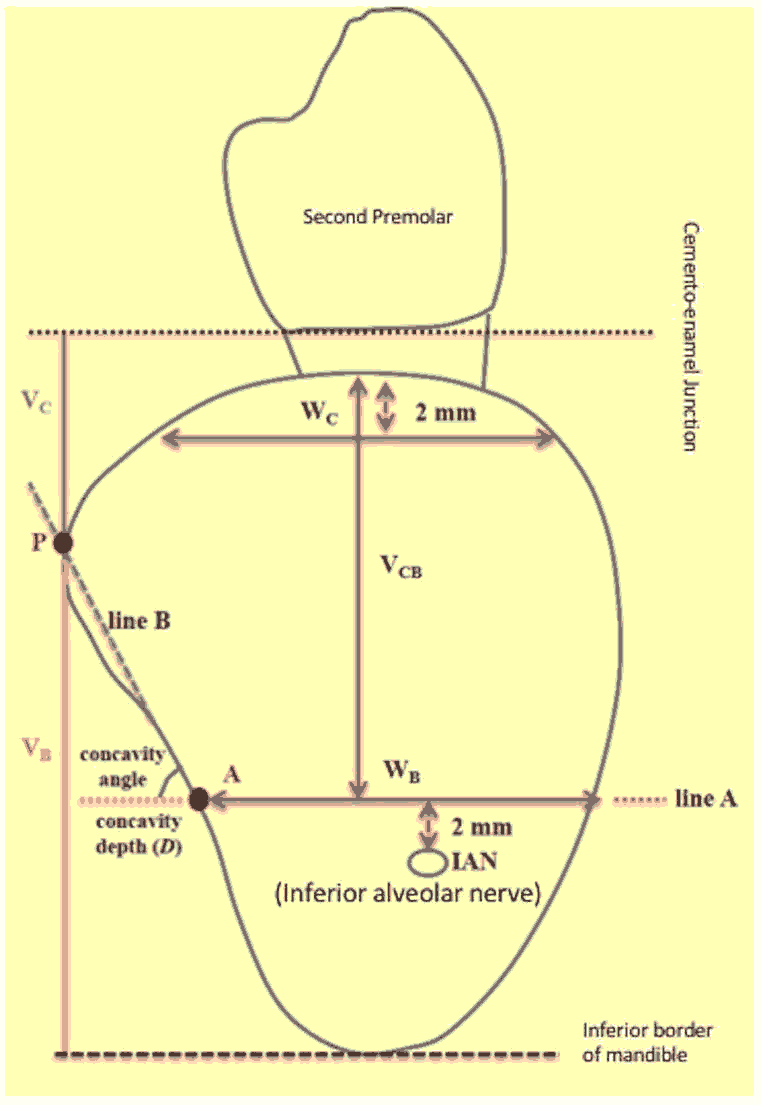
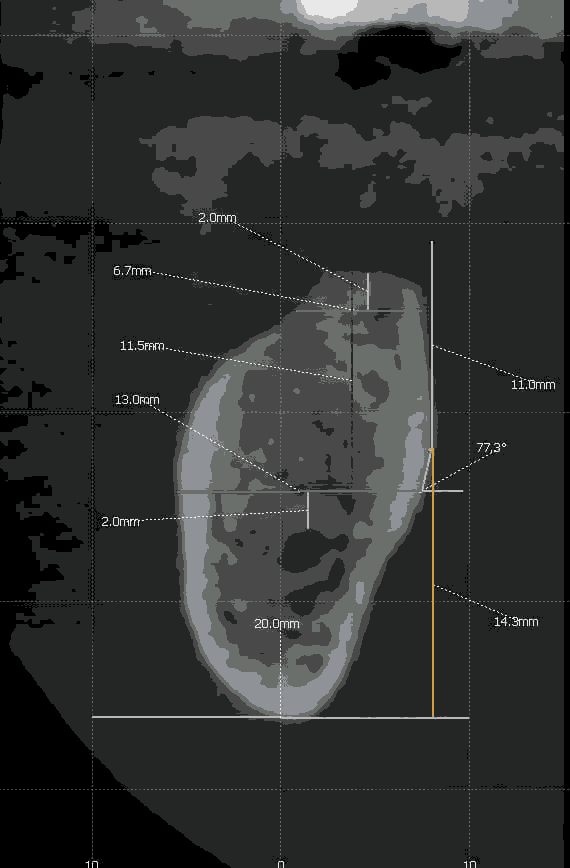
Morphological measurements [Figure 2 and Figure 3] Line B connected point A to point P. Two measurements were recorded. Vc was the vertical distance assessment from point P to alveolar crest while Vb was the vertical distance assessed from point P to inferior mandibular border. The distance in an horizontal plane between Vb and point A was linear concavity depth (D). The angle of concavity was measured as the angle drawn between line B and deepest line of concavity. As a rule, greater the concavity, smaller was the angle. Morphologic characterization of this area was calculated by using following points, the buccolingual width 2 mm apical to the alveolar crest (Wc) and at the level of line A (Wb). The vertical distance from alveolar crest to line A (Vcb) was also calculated.
Data obtained were transferred to spread sheets and analysed with SPSS version 21.0 (IBM; Chicago). The Kolmogorov- Smirnov was used to check for the normal distribution of sample. Analysis of variance and chi square tests were employed to detect any significant differences between genders. A p value of lesser than 0.05 was considered to be statistically significant.
The inter-operator error was assessed using the intra-class correlation coefficient. High correlation was found for interoperator (r=0.85) error. Correlation between examiners in classifying the morphology of the ridges was evaluated by applying the modified Kappa test.
Results
A total of 165 scans were evaluated with a mean age of 46.34+16.55 years, with 52.1% (86) male population and 47.9% (79) of them females [Table 1]. The intra class observer agreement was 96% for all variables, considered to be of substantial agreement. 71 (43.0%) scans were of the left side and 94 (57.0%) images in the right side [Table 2]. More than half of the cases presented with ‘U type’ ridges accounting to 58.8%, with 24.2% of P type and 17.0% C type [Table 3].
| Variables | Males | Females | Total |
|---|---|---|---|
| Gender | 86 (52.1%) | 79 (47.9%) | 165 (100%) |
| Age | 47.3721 ± 16.9941 | 45.2278 ± 16.0982 | 46.3455 ± 16.5557 |
Table 1: Age and gender distribution of study population.
| Side | Gender | Total | |
|---|---|---|---|
| Males | Females | ||
| Left | 38 (23.0%) | 33 (20.0%) | 71 (43.0%) |
| Right | 48 (29.1%) | 46 (27.9%) | 94 (57.0%) |
| Total | 86 (52.1%) | 79 (47.9%) | 165 (100) |
| Chi square test=0.098, p=0.438 (NS) | |||
Table 2: Distribution of sample as per side assessed.
| Type | Gender | Total | |
|---|---|---|---|
| Males | Females | ||
| U type | 43 (26.1%) | 54(32.7%) | 97 (58.8%) |
| P type | 26 (15.8%) | 14 (8.5%) | 40 (24.2%) |
| C type | 17 (10.3%) | 11 (6.7%) | 28 (17.0%) |
| Total | 86 (52.1%) | 79 (47.9%) | 165 (100) |
| Chi square test=5.847, p=0.05 (NS) | |||
Table 3: Distribution of sample as per mandibular ridge type assessed.
The mandibular dimensions and lingual concavity recordings are put together in Table 4. The bucco-lingual width 2mm apical to the alveolar crest (Wc) was 6.56 ± 1.27 in males and 6.93 ± 1.68 in females, which was not significant. The mandibular width 2 mm coronal to IAN (Wb) was 11.31 ± 1.30 in males and 11.50 ± 1.77 in females. The vertical height from alveolar crest to 2 mm coronal to IAN (Vcb) was 11.13 ± 2.26 and 11.43 ± 2.26 in males and females respectively. There was a significant difference between gender for concavity angle measurements with 55.23 ± 15.84 readings in males and 48.03 ± 14.97 amongst females. Lingual plate perforation was not found in any of the images.
| Mandibular dimension and lingual concavity | Males | Females | Total | Anova test | P value |
|---|---|---|---|---|---|
| Wc | 6.5616 ± 1.2757 | 6.9304 ± 1.6800 | 6.7382 ± 1.4900 | 2.546 | .113 (NS) |
| Wb | 11.3186 ± 1.3079 | 11.5038 ± 1.7798 | 11.4073 ± 1.5449 | .586 | .445 (NS) |
| Vcb | 11.1337 ± 2.2684 | 11.4304 ± 2.2654 | 11.2758 ± 2.2649 | .705 | .402 (NS) |
| Vb | 15.8616 ± 3.8284 | 15.2886 ± 3.6400 | 15.5873 ± 3.7390 | .967 | .327 (NS) |
| Vc | 10.9291 ± 3.5824 | 11.4456 ± 3.8184 | 3.6950 ± 0.2876 | .804 | .371 (NS) |
| D | 2.7663 ± 1.5553 | 2.7076 ± 1.29206 | 2.7382 ± 1.4314 | .069 | .793 (NS) |
| Ca | 55.2372 ± 15.8475 | 48.0367 ± 14.9743 | 51.7897 ± 1.2305 | 8.960 | .003** |
| **: Highly significant; *: Significant; NS: Not significant | |||||
Table 4: Measurements of mandibular dimension and lingual concavity.
| 1st M | Gender | Total | |
|---|---|---|---|
| Males | Females | ||
| Yes | 55 (33.3%) | 53(32.1%) | 108 (65.5%) |
| No | 31 (18.8%) | 26 (15.8%) | 57 (34.5%) |
| Total | 86 (52.1%) | 79 (47.9%) | 165 (100) |
| Chi square test=0.179, p=0.744 (NS) | |||
Table 5: Distribution of sample as per side 1stM
Discussion
The present study evaluated the prevalence and extent of lingual concavity using CBCT in the mandibular first molar region. CBCT in dentistry offers significant advantages over CT scans in being less cumbersome, cheaper and lower radiation exposure. This was backed up and recommended by American Association of Oral and Maxillofacial Radiology in planning of dental implant placement. [12,13] The competency of depicting cross sectional vision along with its accuracy and high resolution, renders CBCT as a perfect tool in morphological evaluation of mandibular posterior location, particularly in identification of lingual concavity. The present study evaluated vertical bone height of >10 mm from the alveolar crest to the superior border of the Inferior Alveolar Nerve canal (IAN) so as place an implant of 8 mm height. Literature evidence as provided by the studies of Guldane et al. [14] and Hsun-Liang Chan et al. [5] included a sufficient bone height and width for accommodating a 10 mm implant. Thus, including a 8 mm implant criteria would stand at equal grounds of 10 mm implant placement.
Lingual concavity occurrence in the mandibular posterior region increases the chances of lingual perforation during implant placement. It also is important to evaluate the amount of bone at implant site, which has a significant part in osseo integration. The current study results showed that U type concavity were present in 58.8% of the mandible, while P type and C type lingual concavity accounted next at 24.2% and 17.0%. This finding was in similar lines to the study of Salemi et al. [15] where U type ridge was seen in 50%, followed by 26.2% of C type and 23.8% of P type ridges and Nickenig et al. [16] with presence of 68%, 21% and 11% of U type, P type and C type ridges respectively. On the contrary, Watanabe et al. [14] presented type C as the most common form seconded by A type (59% versus 36%). The variations in lingual concavity between studies can be attributed to different classification employed, differing ethnicity of the study population and dentate status.
The mean Wc, Wb, Vcb, Vb and Vc in our study was 6.7382 ± 1.4900, 11.4073 ± 1.5449 and 11.2758 ± 2.2649 respectively. These were in concordance with the readings of Magat et al. [11] who reported mean values of Wc, Wb, and Vcb values to be 7.60 ± 2.14 mm, 10.76 ± 1.88 mm, and 14.13 ± 2.96 mm, respectively. Similar scores were seen is studies of Chan et al. [5] and Herranz-Aparicio et al. [17] Also variation in methodology, sample size and age ranges might have influenced the variables considered.
Our study did not find any significant differences between gender among Wc, Wb, Vc, Vb and LCD, which was similar to the study of Magat et al. [14] This could be attributable to difference in selected references points for measurements and variations in duration of edentulism amongst the study sample.
The study population in our study presented with a concavity angle of 51.78 ± 1.23, with a mean of 55.23 ± 15.84 amongst males and 48.03 ± 14.97 in the females, which was found to be statistically significant at p<0.003. This finding is not in line with the study of Salemi et al. [15] who reported a mean of 59.4 ± 8.9 in males and 60.2 ± 9.8 amongst females which was non – significant.
Risks of lingual plate perforation differ between anterior and posterior mandibular location. In the anterior region, major artery branches are in closest proximity to the mandible such as submental and sublingual arteries, the resultant complication being massive haemorrhage with subsequent possibility of airway obstruction. [18] Absence of vital structures in submandibular space offers a safer bet for the posterior mandibular region, excepting the case of lingual nerve injury, if perforation is above myelohyoid ridge.
The small sample size could probably affect the external validity of the study. But literature evidence suggests that most of the studies in this regard also have same sample sizes. Further studies employing prospective study design considering confounding variables of duration of edentulousness, age variation and extraction method are recommended to overcome the limitation imposed by the retrospective study design employed in the present study.
Conclusion
Lingual Concavities are a frequent occurrence in edentulous mandibular posterior region. In our study, U type alveolar ridges were the most commonly seen and no significant differences were noted among mandibular morphology between genders. However, CBCT data provided valuable 3Dimensional information in determining the presence and extent of lingual morphology, to formulate safe implant placement in mandibular first molar area and prevent complications arising due to lingual plate perforation.
Conflict of Interests
The authors declare that they have no conflict of interest
REFERENCES
- Rajput BS, Merita S, Parihar AS, Vyas T, Kaur P, Chansoria S. Assessment of lingual concavities in submandibular fossa region in patients requiring dental implants-A cone beam computed tomography study. J Contemp Dent Pract. 2018;19:1329-1333.
- Greenstein G, Cavallaro J, Romanos G, Tarnow D. Clinical recommendations for avoiding and managing surgical complications associated with implant dentistry: A review. J Periodontol. 2008;79:1317-1329.
- Greenstein G, Cavallaro J, Tarnow D. Practical application of anatomy for the dental implant surgeon. J Periodontol. 2008;79:1833-1846
- de Souza LA, Souza PANM, Ribeiro RA, PiresCarvalho AC, Devito KL. Assessment of mandibular posterior regional landmarks using cone-beam computed tomography in dental implant surgery. Ann Anat. 2016;205:53-59.
- Chan HL, Brooks SL, Fu JH, Yeh CY, Rudek I, Wang HL. Cross‑sectional analysis of the mandibular lingual concavity using cone beam computed tomography. Clin Oral Impl Res. 2011;22:201-206.
- Chen LC, Lundgren T, Hallström H, Cherel F. Comparison of different methods of assessing alveolar ridge dimensions prior to dental implant placement. J Periodontol. 2008;79:401‑405.
- Watanabe H, Mohammad AM, Kurabayashi T, Aoki H. Mandible size and morphology determined with CT on a premise of dental implant operation. Surg Radiol Anat. 2010;32:343-349.
- Kamburoglu K, Acar B, Yuksel S, Paksoy CS. CBCT quantitative evaluation of mandibular lingual concavities in dental implant patients. Surg Radiol Anat. 2015;37:1209-1215.
- Chiapasco M, Abati S, Romeo E, Vogel G. Clinical outcome of autogenous bone blocks or guided bone regeneration with e-PTFE membranes for the reconstruction of narrow edentulous ridges. Clin Oral Implan Res. 1999;10:278-288.
- Sammartino G, Marenzi G, Citarella R, Ciccarelli R, Wang HL. Analysis of the occlusal stress transmitted to the inferior alveolar nerve by an osseo integrated threaded fixture. J Periodontol. 2008;79:1735-1744
- Greenstein G, Dennis T. The mental foramen and nerve: clinical and anatomical factors related to dental implant placement: a literature review. J Periodontol.2006;12:1933-1943.
- Arai Y, Tammisalo E, Iwai K, Hashimoto K, Shinoda K. Development of a compact computed tomographic apparatus for dental use. Dentomaxillofac Radiol. 1999;28:245‑248.
- Suomalainen A, Vehmas T, Kortesniemi M, Robinson S, Peltola J. Accuracy of linear measurements using dental cone beam and conventional multislice computed tomography. Dentomaxillofac Radiol. 2008;37:10‑17.
- Guldane M. Radio morphometric analysis of edentulous posterior mandibular ridges in the first molar region: a cone-beam computed tomography study. J Periodontal Implant Sci. 2020;50:28-37.
- Salemi F, Shokri A, Forouzandeh M, Karami M, Khalili Z. Mandibular lingual concavity: a cross-sectional analysis using cone beam computed tomography. J Clin Diagn Res. 2018;12.
- Nickenig HJ, Wichmann M, Eitner S, Zoller JE, Kreppel M. Lingual concavities in the mandible: a morphological study using cross-sectional analysis determined by CBCT. J Craniomaxillofac Surg. 2015;43:254-259.
- Herranz-Aparicio J, Marques J, Almendros-Marqués N, Gay-Escoda C. Retrospective study of the bone morphology in the posterior mandibular region. Evaluation of the prevalence and the degree of lingual concavity and their possible complications. Med Oral Patol Oral Cir Bucal. 2016;21:731-736.
- Kalpidis CD, Setayesh RM. Hemorrhaging associated with endosseous implant placement in the anterior mandible: a review of the literature. J Periodontol. 2004;75:631-645.




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.