Reservoir Complete Denture in a Patient with Xerostomia Secondary to Radiotherapy for Oral Carcinoma: A Case Report and Review of Literature
- *Corresponding Author:
- Dr. Ruchi Ladda
Department of Prosthodontics, Rural Dental College, Loni - 413 736, Maharashtra, India.
E-mail: drruchikasat@gmail.com
Citation: Ladda R, Kasat VO, Gangadhar SA, Baheti S, Bhandari AJ. Reservoir complete denture in a patient with xerostomia secondary to radiotherapy for oral carcinoma: A case report and review of literature. Ann Med Health Sci Res 2014;4:271-5.
Abstract
Xerostomia refers to a subjective sensation of dry mouth. A variety of factors can cause xerostomia including radiotherapy (RT) given for the treatment of oral carcinoma. Depending on the cause, treatment is provided to a patient suffering from xerostomia. In severe xerostomia salivary substitutes can be used and if the xerostomic patient is edentulous, then reservoir space for artificial salivary substitute can be created in partial as well as complete upper or lower dentures. The methods advocated so far for incorporating reservoir space in mandibular complete denture are costly, time consuming and require extra‑laboratory steps. Therefore, the purpose of this article is to report a simpler method for fabrication of mandibular reservoir denture in a 67‑year‑old edentulous male patient suffering from xerostomia due to RT for oral carcinoma.
Keywords
Oral carcinoma, Radiotherapy, Reservoir denture, Salivary substitute, Xerostomia
Introduction
Oral cancer is one of the most commonly occurring malignancy in India and 94% of them are squamous cell carcinomas.[1] Squamous cell carcinomas are usually radiosensitive and many T1 and T2 tumors may be treated by radiotherapy (RT) alone.[2] In RT, a total dose of 50-70 Gy is administered over a period of 5-7 weeks (2 Gy/d × 5 d) and patients who receive RT to the fields involving the oral cavity experience various oral complications.[3]
Xerostomia is one such a common complication after RT because salivary glands are very sensitive to radiation. After RT, the changes in the salivary glands such as progressive fibrosis, loss of fine vasculature and parenchymal degeneration account for the xerostomia. Xerostomia refers to a subjective sensation of dry mouth.[1] It disrupts the normal homeostasis of the oral cavity, leading to changes in the taste, difficulty in speech, difficulty in swallowing and decreased dietary intake. These have a significant negative impact on patient’s health and overall quality-of-life.[3] Moreover, as saliva acts as a thin film between the dentures and the oral mucosa, its absence decreases retention of the dentures and increases inflammation and ulceration in the oral cavity.[4] Hence, dentures are often poorly tolerated in an edentulous patient suffering from dry mouth.[4-6]
To lessen the problem of dry mouth, patients are often advised to increase the frequency of water intake, include more citrus fruits in the diet and use sugar free chewing gums for salivary stimulation. In severe xerostomia, salivary substitutes may be utilized.[5,7] They contain carboxymethylcellulose, electrolytes, flavoring agents and are available as solutions, sprays or gels.[4] In edentulous patients, one method of using these salivary substitutes is incorporating salivary reservoir in upper or lower complete denture so that a continuous flow of wetting agent is achieved. This article aims to provide a simpler method of incorporating salivary reservoir in the mandibular complete denture of a xerostomic patient.
Case Report
A 67-year-old male patient reported to the Department of Prosthodontics with the chief complaint of difficulty in mastication due to dryness of mouth and absence of teeth.
Medical history revealed that the patient had undergone RT 2 years back for the moderately differentiated squamous cell carcinoma involving posterior 1/3rd of left lateral border of the tongue.
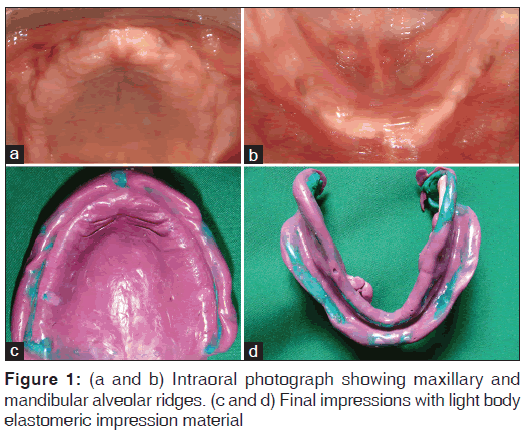
Extraoral examination revealed reduced lower facial height and unsupported lips. Intraoral examination revealed maxillary and mandibular edentulous residual ridges and decreased salivary flow [Figure 1a and b]. A diagnosis of xerostomia secondary to RT was made after calculating unstimulated whole saliva flow rate by absorbent (swab) method (whole saliva flow rate was < 0.1 ml/min).
Treatment plan
Treatment plan included either (1) fabrication of implant supported or conventional upper and lower complete dentures with external application of salivary substitute in the oral cavity or (2) fabrication of lower complete denture with artificial saliva reservoir in it and upper conventional complete denture. It was discussed with the patient and informed consent was obtained for the agreed treatment, which included rehabilitation of the upper arch with conventional complete denture and reservoir denture in the lower arch.
Procedure
1. Primary impressions were recorded in irreversible hydrocolloid impression material. After border molding, final impressions were made in medium body elastomeric impression material [Figure 1c and d]
2. Jaw relation was recorded with wax occlusal rims fabricated on self-cure acrylic denture base. The vertical height of the lower rim was measured. Accordingly, teeth selection was carried out and size of the reservoir was determined, so that maximum space for the reservoir is gained while maintaining 2 mm thickness of the reservoir wall. Then using face bow, only upper cast was mounted on the semi-adjustable articulator. Upper and lower wax rims with the centric records were preserved and set aside for later use
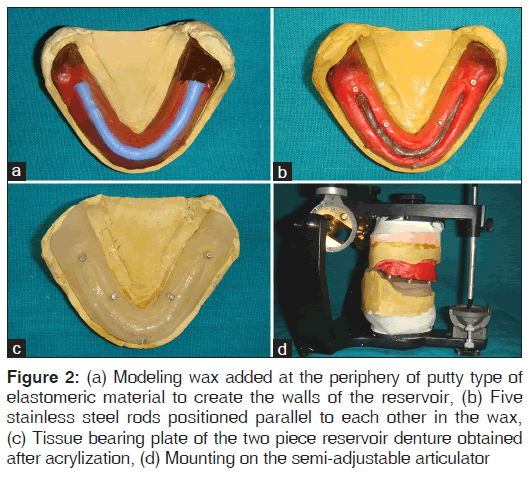
3. Shellac base plate was adapted on the lower final cast. According to the predetermined dimensions, putty type of elastomeric material was placed in the center of the base plate and modeling wax (modeling wax, DPI, Mumbai, India) was added at the periphery to create the walls of the reservoir [Figure 2a]. Space for reservoir was created by removing putty from the center [Figure 2b]. Five stainless steel rods (3 mm in length and 2 mm in diameter) were positioned parallel to each other in the wax [Figure 2b]. The two parts of the reservoir lower denture would be attached to each other using these rods. A bevel was carved 1-1.5 mm above the inferior border at the periphery of the base
4. Then flasking and dewaxing was carried out as a routine procedure. Clear heat cure polymerized resin was used for packing the mold space (Trevalon HI, Dentsply India Ltd., Gurgaon, India) and after curing a permanent clear acrylic base was obtained with five stainless steel rods embedded in it and having a reservoir in the center. Thus, the tissue bearing plate of the two piece reservoir denture was fabricated [Figure 2c]
5. Next, the lower cast was retrieved from the flask and with the preserved wax occlusal records it was mounted on the semi-adjustable articulator. After this, the lower temporary record base was replaced with the permanent clear acrylic base [Figure 2d]
Figure 2: (a) Modeling wax added at the periphery of putty type of elastomeric material to create the walls of the reservoir, (b) Five stainless steel rods positioned parallel to each other in the wax, (c) Tissue bearing plate of the two piece reservoir denture obtained after acrylization, (d) Mounting on the semi-adjustable articulator
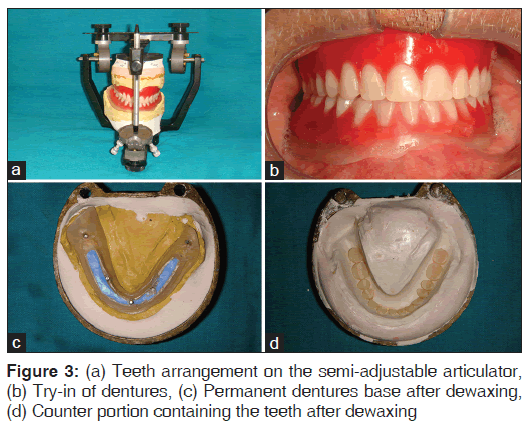
6. Teeth arrangement was carried out on the semi-adjustable articulator with putty maintaining the reservoir space [Figure 3a]. Extra bulk of wax was added to the mandibular trial denture to gain optimum thickness. Then trial dentures were finished and tried in the patient’s mouth to check for retention, stability, esthetics, phonetics and comfort [Figure 3b]
7. Flasking followed by dewaxing of the lower trial denture was carried out to obtain base portion of the flask containing permanent denture base [Figure 3c] and a counter portion containing the teeth [Figure 3d]
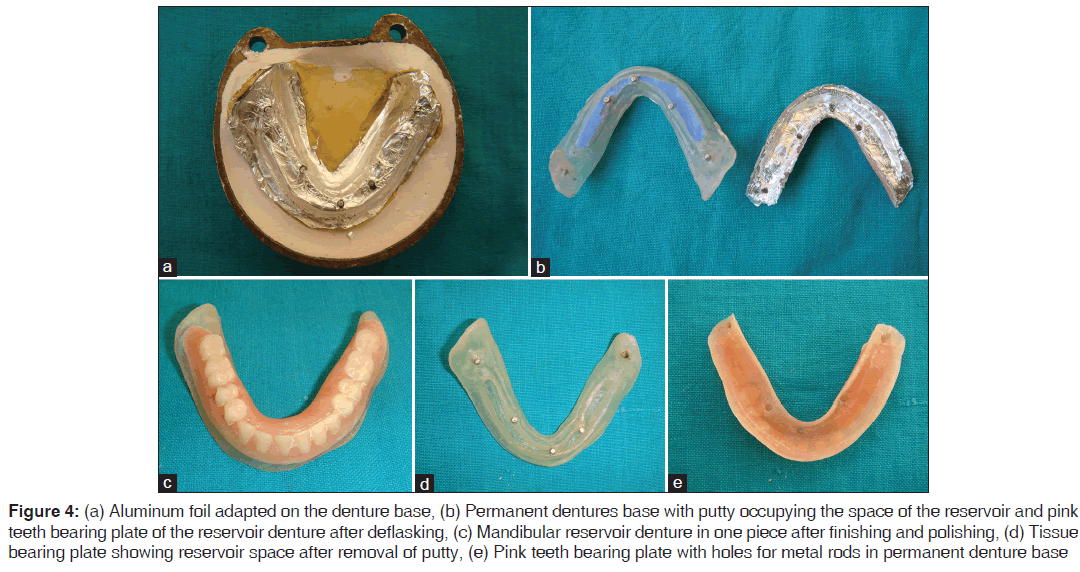
8. Aluminum foil was adapted on the denture base for easy separation of the two halves of the mandibular denture [Figure 4a]. Packing was carried out with pink heat cure acrylic resin (Trevalon HI, Dentsply India Ltd., Gurgaon, India) and processed to obtain the teeth bearing plate of the reservoir denture [Figure 4b]
9. After careful deflasking aluminum foil was removed. The teeth bearing plate of the mandibular denture rested on the bevel created on the tissue bearing plate. Finishing and polishing was carried out with the segments together to ensure a flush smooth finish, without any damage to the edges [Figure 4c]
Figure 4: (a) Aluminum foil adapted on the denture base, (b) Permanent dentures base with putty occupying the space of the reservoir and pink teeth bearing plate of the reservoir denture after deflasking, (c) Mandibular reservoir denture in one piece after finishing and polishing, (d) Tissue bearing plate showing reservoir space after removal of putty, (e) Pink teeth bearing plate with holes for metal rods in permanent denture base
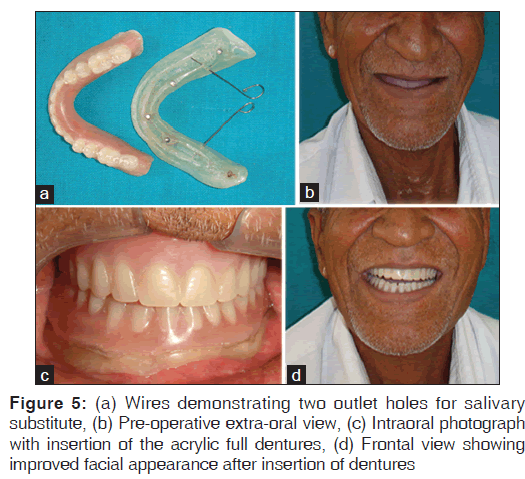
10. Two outlet holes were drilled for the salivary substitute on each side in the retromylohyoid region of the teeth bearing plate and were adjusted in size similar to the thickness of a 23 gauge orthodontic wire [Figure 5a]
11. Artificial saliva substitute (Wet mouth, ICPA Health Products Ltd., India) was then filled in the reservoir space of the lower denture with a capacity of 3.8 ml
12. The upper denture was fabricated in the conventional manner
13. Denture insertion was carried out and post-insertion instructions were given to the patient. Furthermore, he was taught how to open and close the reservoir denture for filling the artificial salivary substitute and cleaning the reservoir space. In addition, fine orthodontic wire was provided to him for cleaning the drainage holes if they get blocked
14. Recall appointments were scheduled after 24 h, 1 week, 4 weeks and every 6 months. At recall appointments, good retention was observed and relief from the symptoms of dry mouth and improvement in dietary intake was reported by patient. Patient found it easy to clean the dentures as taught and informed that once filled saliva substitute lasts for 4-5 h. Patient has now been successfully wearing the dentures for over 2 years.
Discussion
Retention is the resistance of denture to removal in a direction opposite to that of insertion. Retention of complete denture depends on the various factors such as adhesion, cohesion, interfacial surface tension and saliva plays an important role for these factors to be effective. This has to be taken into account while rehabilitating an edentulous patient with xerostomia. Xerostomia is seen commonly after use of various therapeutic drugs. Few of the other causes include local factors like decreased mastication, systemic factors like Sjogren’s syndrome, water/metabolite loss due to vomiting and RT as in the present case.
To overcome the problems of xerostomia in an edentulous patient, along with the other measures use of reservoir denture is advocated. Various methods have been described in the literature for incorporating salivary reservoir in complete and partial dentures.
Agrawal et al.[8] described a method for fabricating salivary reservoir between the straps of maxillary anterior-posterior strap major connector in a patient with Sjogren’s syndrome. Stainless steel snap buttons were used to join the two parts of the reservoir. Disadvantages of this design were: (1) It was bulky affecting speech, comfort and retention, (2) snap buttons needed replacement as they loosened with time.
Modgi and Aras[9] described a technique for incorporation of saliva reservoir in the maxillary cast partial denture with the help of precision attachments in a patient with post-irradiation xerostomia. Female component of precision attachment was placed in complete coverage palatal major connector and male component was incorporated in the lid of the reservoir. Disadvantage of the precision attachment is that it increases the cost of the treatment.
Toljanic and Zucuskie[10] incorporated salivary reservoir in the maxillary denture and stated following advantages of it over a reservoir in the mandibular denture: (1) Larger reservoir size, (2) provides flow of saliva to the whole mouth unlike mandibular reservoir where flow is restricted to the floor of the mouth, (3) fluid and food in the floor of the mouth do not block outlet holes. Contrary to this, Sinclair et al. 11] thought that the mandibular denture would be more advantageous as a reservoir denture because a simple gravity feed system would be possible and deliver the wetting agent directly to the mucosa. Furthermore, incorporating reservoir in the maxillary denture leads to increase in weight, which may affect its retention and stability.
So far various designs for the mandibular reservoir denture are suggested and practiced in the literature. Sinclair et al.[11] used cobalt samarium magnets to connect the lower and upper part of the mandibular reservoir denture. Though he succeeded in providing a reservoir with a maximum capacity, the procedure required exhaustive laboratory steps. This is because first dentures were made, then the lower denture was duplicated and further laboratory steps were carried out to create reservoir space.
Mendoza and Tomlinson[6] described another technique for artificial saliva reservoir in the mandibular denture, which was split into upper and lower parts. In their technique also laboratory stages were time consuming (though less as compared to technique by Sinclair et al.), as it required firstly the duplication of master casts and then again duplication of the clear acrylic base portion so that upper section of the mandibular denture would be waxed up on it and processed. Furthermore, two articulators were required. They used double-toothed LegoTM blocks for attachment of two parts of the reservoir denture. Similar method was used by Dabas et al.,[7] and Hallikerimath and Jain.[4]
In the method described by Burhanpurwala et al.,[5] for the mandibular reservoir denture, master casts were not duplicated initially, but still the laboratory steps were complicated. Their method required single articulator, but two flasks. After try-in, flasking and dewaxing was done. Then clear acrylic base was made on the master cast present in the base portion of the first flask and using upper portion of another flask and later on entire base part of the flask containing clear acrylic plate on the master cast was duplicated. Pink colored heat cure acrylic resin was then packed between this new base flask and the teeth bearing counter portion of the first flask to obtain the teeth bearing plate of the reservoir denture.
Disadvantages of above methods were overcome in our method. Our technique required only single articulator, single flask and one set of master casts as clear acrylic base and teeth bearing plate was made on the same master cast and aluminum foil was used for easy separation of the two parts. Thus, it is clear that laboratory steps involved in our method are simple and less time consuming.
In the methods described in the literature reservoir space was made after acrylization, which may result in rough internal surface as it cannot be polished so easily,[4,6,7] whereas in our case space was created before acrylization by blocking the area with putty material, which resulted in the smooth internal surface. As described in earlier methods, in our method also base section was made up of clear acrylic because it enables the patient to clearly visualize the levels of the salivary substitute within the reservoir space.[4]
According to Sinclair et al.,[11] design and construction of the reservoir denture should fulfill three criteria: (1) Maximum space for the reservoir, (2) minimum adjustments in the finished denture so that a maximally extended reservoir would not be perforated and (3) provide ease of cleaning and refilling the reservoir. Reservoir denture fabricated by our technique fulfilled all these criteria.
Though our technique has a definite advantage over other techniques, it probably cannot be used in cases with severe tissue undercuts, wherein duplication of master cast would be required.
Conclusion
In summary, this paper reports a technique for the construction of the mandibular reservoir denture as one of the treatment modality for edentulous patients with xerostomia. The main advantage of this technique over the previous methods is that the laboratory steps involved are simple and are less time consuming.
References
- Neville BW, Damm DD, Allen CM, Bouquot JE. Oral and Maxillofacial Pathology. 2nd ed. Philadelphia: W.B. Saunders Company; 2002. p. 356, 398.
- Epstein JB. Oral cancer. In: Greenberg MS, Glick M, editors. Burket’s Oral Medicine, Diagnosis and Treatment. 10th ed. Canada: BC Decker Inc.; 2003. p. 207.
- Brosky ME. The role of saliva in oral health: Strategies for prevention and management of xerostomia. J Support Oncol 2007;5:215?25.
- Hallikerimath RB, Jain M. Managing the edentulous dry mouth: The two part mandibular denture. J Indian Prosthodont Soc 2012;12:51?4.
- Burhanpurwala MA, Magar S, Bhandari AJ, Gangadhar SA. Management of an edentulous patient having xerostomia with artificial saliva reservoir denture. J Indian Prosthodont Soc 2009;9:92?5.
- Mendoza AR, Tomlinson MJ. The split denture: A new technique for artificial saliva reservoirs in mandibular dentures. Aust Dent J 2003;48:190?4.
- Dabas N, Phukela SS, Yadav H. The split denture: Managing xerostomia in denture patients: A case report. J Indian Prosthodont Soc 2011;11:67?70.
- Agrawal KK, Singh SV, Rashmikant US, Singh RD, Chand P. Prosthodontic rehabilitation in Sjogren's syndrome with a simplified palatal reservoir: Two year follow up. J Prosthodont Res 2011;55:248?51.
- Modgi CM, Aras MA. An innovative design of 2?piece saliva reservoir using precision attachment: A case report. J Indian Prosthodont Soc 2012;12:260?3.
- Toljanic JA, Zucuskie TG. Use of a palatal reservoir in denture patients with xerostomia. J Prosthet Dent 1984;52:540?4.
- Sinclair GF, Frost PM, Walter JD. New design for an artificial saliva reservoir for the mandibular complete denture. J Prosthet Dent 1996;75:276?80




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.