Sacroiliac Joint Pain and Joint Mobility in Postpartum Women: A Prospective Cohort Study
2 Department of Physiology, Fatima Memorial Hospital, Lahore, Pakistan
3 Department of Physiology, Riphah International University, Lahore, Pakistan
Received: 22-Jun-2022, Manuscript No. AMHSR-22-69938; Editor assigned: 24-Jun-2022, Pre QC No. AMHSR-22-69938 (PQ); Reviewed: 08-Aug-2022 QC No. AMHSR-22-69938; Revised: 03-Nov-2022, Manuscript No. AMHSR-22-69938 (R); Published: 10-Nov-2022
Citation: Anwar N, et al.. Sacroiliac Joint Pain and Joint Mobility in Postpartum Women: A Prospective Cohort Study. Ann Med Health Sci Res. 2022;12:1-5
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Introduction: The incidence of SIJ pain during pregnancy is 78.7%. SIJ pain has been found to be progressive throughout the three trimesters of pregnancy. Pelvis that is tilted anteriorly in the first trimester of pregnancy is risk factors for sacroiliac joint pain. Pain in the sacroiliac joint can lead to significant overall mobility restrictions for women.
Objective: The objective of the study was to determine changes in pain severity, mobility of the sacroiliac joint and changes in sacroiliac joint pain diagnostic tests effects at 37th week of pregnancy and 8 weeks after delivery.
Methodology: The study was prospective longitudinal study; convenient non-probability sampling technique was used to collect the data. Females between the ages of 18 to 35 who were pregnant at the time study was conducted were diagnosed for sacroiliac joint pain with physical testing. Intensity of pain and pelvic mobility were determined using visual analogue scale and pregnancy mobility index after 37th week of pregnancy. Then, 8 weeks after delivery only those patient who had normal mode of delivery were called upon for a follow up whereby the combination of test were reapplied for the second time and pain along with pelvic mobility were reassessed and compared.
Results: Pre and postpartum comparison of VAS and PMI has showed that there was a significant difference in pain and pelvic mobility, the mean for pain intensity at 37th week prepartum was 7.05 ± 1.339 and at 8 weeks postpartum was 4.40 ± 2.146 while mean for PMI at 37th week prepartum was 27.88 ± 9.067 and at 8 weeks postpartum was 22.20 ± 10.125 with p value <0.05.
Conclusion: It was concluded that women with intense pain levels and significant limitations of movement during the last month of pregnancy had substantial reduction in frequency of pain intensity along with increase in house and outdoor movement after two months of delivery.
Keywords
Sacroiliac joint pain; Pelvic girdle pain; Visual analogue scale; Diagnostic criteria; Pregnancy mobility index
Introduction
Sacroiliac joint is a wide and complicated diarthrodial synovial joint which is strongly connected by a ligamentous framework that offers stability and motion restriction across all axes [1]. The incidence of SIJ pain during pregnancy is 78.7%. Sacroiliac joint pain is a very common problem seen among pregnant women during the course of their pregnancy. This pain has been found to be progressive throughout the three trimesters of pregnancy. These patients also have mobility issues during this period which has considerable impact on their life styles [2]. Pelvis can be tilted anteriorly and posteriorly. Moreover, a pelvis that is tilted anteriorly in the first trimester of pregnancy and in which asymmetry is seen during pregnancy are risk factors for pregnancy related sacroiliac joint pain [3]. Multiple physical and psychosocial factors are responsible for causing pain in the pelvic region. The physical risk factors mostly associated with this type of pain include a history of low back pain before pregnancy, injury of the spine or pelvis, multiparty, contraceptive pills, weight increase in pregnancy. The psychosocial factors mostly commonly associated are daily high stress level and job dissatisfaction [4]. Women during pregnancy undergoes various physical and anatomical changes. Increased body weight, posture change, and hormonal relaxation of joint structures primarily relaxing leads to alterations causing increased laxity and make them susceptible to future injuries and dysfunctions due to increased or decreased mobility of the joint [5]. Sacroiliac joint pain can be diagnosed on basis of pain provocation tests when applied in combination. One of the clusters described by Mark Haslett comprises of 5 tests (Distraction, Compression, Thigh Thrust, Gaenslen, Sacral thrust). Three out of five positive tests indicates pain with sensitivity of 94% and specificity of 78% [6]. Pain in the sacroiliac joint can lead to significant overall mobility restrictions for women which can impact their daily as well as recreational activities [7]. Pregnancy mobility index is valid self-reported questionnaire which gives knowledge of physical status of patients. Questions mainly concern daily mobility in house, ease of performing daily household activities and outdoor mobility. All these are given a score option of 0 to 3 which is transformed to a 0 to 72 scale. A higher score indicates limitation of the activity in daily life [8]. Although much is known about sacroiliac joint dysfunction during pregnancy but there was no vast literature that conducted a follow up study of SIJ pain in pregnant women after delivery. This study was conducted to help raise awareness of SIJ pain in future studies in postpartum women and provide them with a better guideline and prevention from disabilities if proper interventions were sought. The purpose of this study was to assess changes in sacroiliac joint pain and mobility two months postpartum. The primary objective of the study was to determine changes in pain severity and mobility of the sacroiliac joint after 37th week of pregnancy and 8 weeks after delivery. The secondary objective was to compare the sacroiliac joint diagnostic tests post 37th week of pregnancy and 8 weeks after delivery.
Materials and Methods
The study was prospective longitudinal study that was conducted in Fatima memorial hospital and fatima memorial college of medicine and dentistry, Lahore from 20 November, 2019 to 15 February, 2020. The calculated sample size was=54, by using effect size (d)=0.5, alpha=0.05 and power=0.95. The sample size was calculated using g power software version 3.1. Convenience non-probability sampling technique was used to collect the data. Females between the ages of 18 to 35, with sacroiliac joint pain during 37-40th week of pregnancy using diagnostic criteria (Distraction test, Compression test, Thigh thrust test, Gillet test, Fortin Finger test. 3 positive test out 5 mentioned will diagnose the patient with sacroiliac joint pain) were included in the study. A total data of 94 patients was collected at the first reading. Data of only that patient who had normal mode of delivery after two months was added and analyzed. The exclusion criteria of the study included patient with C-section, SIJ pain due to any trauma or rheumatic condition, LBP restricted to lumbar region (above L5), pain radiating below the level of knee, risk of pulmonary, GI, or vascular complications, hypertension, pelvic floor dysfunction, urinary or fecal incontinence, organ prolapse, hyper tonus, poor proprioceptive awareness and disuse atrophy, diastasis recti. Approval was given by the respective authorized body of Fatima memorial hospital, Lahore, before data collection procedure. An informed consent was obtained from the participants for including their data in present study. Visual Analogue Scale was used to measure intensity of pain. A constructed and validated self-report questionnaire for use in a pregnant population to assess mobility in relation to back and/or pelvic pain was used. The internal consistency (Cronbach's alpha) for this scale was 0.8 or higher. Frequency of positive test out of five total test of diagnostic criteria established for sacroiliac joint pain were recorded during both readings at ninth month of delivery (after 37 weeks) and two months (after 8 weeks of delivery). The data was statistically analyzed by Statistical Package for Social Sciences (SPSS). 23.0. The quantitative variables were measured in the form of mean and standard deviation whereas the qualitative were evaluated in the form of frequency and proportion. Pain intensity and PMI were analyzed using mean and standard deviation. On the basis of normality testing (using the Shapiro Wilk test of normality), Wilcoxon signed ranks test was used for comparison of pain and paired t-test was used for comparison of pregnancy mobility index before and after pregnancy. Chi square test was used to compare the difference for sacroiliac diagnostic tests (Distraction test, Compression test, Thigh thrust test, Gillett’s test and Fortin finger test) before and after pregnancy.
Results
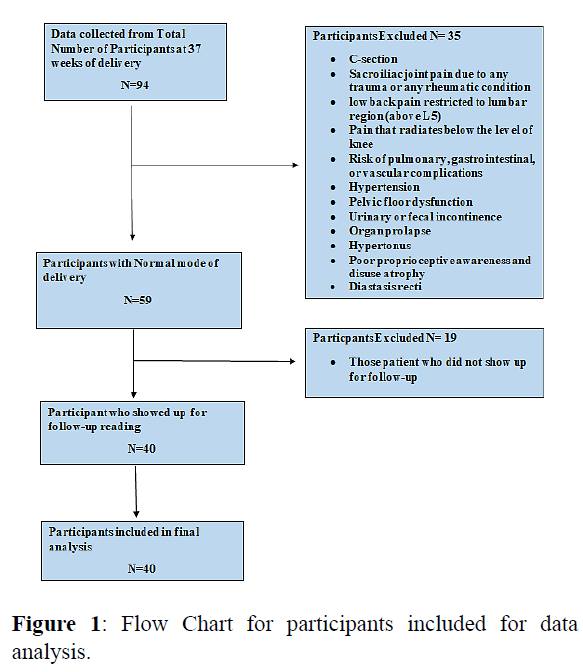
Out of 94 patients, 59 patients had normal mode of delivery of which 40 showed up for follow-up. Data from a total of these 40 patients was analyzed before and after pregnancy. The mean age of the patients was 25.93 ± 3.765. The mean height of the patients was 5.32 ± 0.20. The mean weight calculated was 161.20 lbs with Standard Deviation (SD) of 25.051. The physical characteristics of the participants are shown in Table 1.
| Table 1: Physical characteristics of the participants (n=40). | |||
|---|---|---|---|
| Variables | Minimum | Maximum | Mean |
| Age | 20 | 35 | 25.93 ± 3.765 |
| Height | 4.8 | 5.7 | 5.325 ± .2010 |
| Weight | 110 | 226 | 161.20 ± 25.051 |
The data for pain intensity, mobility and frequency of positive diagnostic was compared only for those patients who had normal mode of delivery and presented for follow up. On the basis normality testing (Shapiro-Wilk), Non-Parametric (Wilcoxon Signed Ranks) test for the comparison of pain was used and paired t-test for the comparison of PMI. The Median and IQR for pain score measured by VAS at 37 weeks prepartum was 7 (6 to 8) while at 8 weeks postpartum was 4 (2.25 to 6) and there was a significant difference (P value<0.05) in pain intensity as measured by VAS (Table 2).
| Table 2: Comparison between pre partum (37th week) and post-partum (after 8 weeks) VAS score. | ||
|---|---|---|
| VAS | Median (IQR) | p-value |
| VAS AT 37th week prepartum | 7 (6 to 8) | <0.05 |
| VAS AT 8th week postpartum | 4 (2.25 to 6) | |
The mobility was assessed using Pregnancy mobility index. The mean for PMI at 37 weeks prepartum was 27.88 ± 9.06 while the mean for VAS at 8 weeks postpartum was 22.20 ± 10.125 and there was a significant difference (P value<0.05) in means of mobility as measured by PMI (Table 3).
| Table 3: Comparison between pre partum (37th week) and post-partum (after 8 weeks) PMI score. | |||
|---|---|---|---|
| PMI | Mean ± SD | Mean difference (95% CI) | p-value |
| PMI AT 37th week prepartum | 27.88 ± 9.067 | 5.67 (3.84-7.50) | <0.05 |
| PMI AT 8th week postpartum | 22.20 ± 10.125 | ||
The frequency of positive test, of diagnostic criteria for SIJ pain, in prepartum women after 37th week has showed that 3 out of 5 tests were positive in 47.5% of patients, 4 out of 5 tests were positive in 37.5% patients and 5 out of 5 tests were positive in 15% of the patients. The frequency of positive test of diagnostic criteria for SIJ pain in postpartum women after 8 weeks of delivery showed 1 out of 5 tests were positive in 32.5% of patients, 2 out of 5 tests were positive in 37.5% patients, 3 out of 5 tests were positive in 22.5% of the patients and 4 out of 5 tests were positive in 7.5% of the patients. Although frequency of positive tests were reduced after the 8th week of delivery when compared to pre partum state but no statistical difference were present as p=0.07 (Table 4 and Figure 1).
| Table 4: Comparison of pre partum (37th week) and post-partum (after 8 weeks) frequencies of positive tests of diagnostic criteria (n=40). | ||||||||
|---|---|---|---|---|---|---|---|---|
| Frequency of positive tests of diagnostic criteria postpartum | Total | p-value | ||||||
| 1/5 | 2/5 | 3/5 | 4/5 | |||||
| Prepartum frequency of positive tests of diagnostic criteria | 3/5 | Count % of Total | 9 | 6 | 3 | 1 | 19 | 0.078 |
| 22.50% | 15.00% | 7.50% | 2.50% | 47.50% | ||||
| 4/5 | Count % of Total | 4 | 7 | 4 | 0 | 15 | ||
| 10.00% | 17.50% | 10.00% | 0.00% | 37.50% | ||||
| 5/5 | Count % of Total | 0 | 2 | 2 | 2 | 6 | ||
| 0.00% | 5.00% | 5.00% | 5.00% | 15.00% | ||||
| Total | Count % of Total | 13 | 15 | 9 | 3 | 40 | ||
| 32.50% | 37.50% | 22.50% | 7.50% | 100.00% | ||||
Discussion
In the following study, sacroiliac joint pain was reduced to a certain extent 8 weeks after delivery in women along with the restoration of mobility as median (IQR) for pain score was 4 (2.25 to 6) after 2 months of delivery. Sacroiliac joint pain in women in the final month of pregnancy was considered to be moderately severe based on visual analog scale scores as median for the pain score in pre partum (37th week of pregnancy) was 7 (6 to 8) which is consistent with previous studies [2]. The use of pregnancy mobility index in the present study signified scores showing notable mobility restriction and disability during the last month of pregnancy that had an impact on daily work for most women as mean PMI score during the 37th week of pregnancy was 27.88 ± 9.06. Also commuting by any transportation means during last month as well as following two months after delivery were the least preferred marked on the questionnaire and answering such questions posed reservations because women were unable to find genuine reasoning to respond to them because these behaviors are rarely preferred during pregnancy due to their dangerous existence [9]. Although pregnancy mobility index is a great source identifying mobility problems in pregnant women, there is still a need for a better questionnaire that establishes mobility restrictions in women specifically with sacroiliac joint pain. There was some limitation in doing simple house chores to maintaining their independent status as some women demonstrated the need for dependence. Mobility scores improved following delivery as mean PMI score was 22.2 ± 10.12 after 2 months of delivery but there were some doubts raised regarding the questionnaire as most women tend to have decreased physical activity specifically walking during final months of pregnancy and after delivery [10]. Pain reduction and mobility improvement in women following delivery is owing to factor that hormones primarily relaxing that are elevated during the course of pregnancy return back to normal within 3 months of pregnancy [11.]In a study suggested that women, although showing a reduction in pain scores, may be completely pain free in the coming weeks or months, but the persistence of pain and the fact of pain becoming chronic has been reported in previous studies with pain returning in future pregnancy [12]. Some factors associated with delayed or persistence of pregnancy related pelvic girdle pain were multiple pregnancies and history of PGP one year before pregnancy. Considerable recovery from Pelvic girdle pain is seen in 83% females after six weeks of delivery and half of these recovered subjectively from pain within the first two week [13]. The continuous persistence of pain must not be forgotten, as it would have a significant impact on selfinvolved health, as well as on their family, social and psychological well-being. This chronicity of pain results in prolonged leave from work place and rise in disability pension which can have a significant impact on financial resources [14]. Studies have been conducted in the past in which pregnancy related pain has persisted months to years after childbirth and subsequent future pregnancy. Women in the study had ongoing struggles with or adapted to the pain and accepted it as part of their lives. The women in our study may have a potential for chronic pain, they must be treated, and their pain must be considered and managed as soon as possible to avoid any long-term effects that could cripple their physical and mental well-being after pregnancy [15]. Changes in pelvic alignment during the post-natal period were analyzed in a study which showed that alignment changes continuously during this time and concluded that changes in pelvic width did not recover one month after partum. Such repeated changes in the symmetrical orientation of the pelvis may suggest why the SI joint pain diagnostic test performed in this study were still positive for the participants two months after delivery [16]. Treatment of pregnant women has rarely been emphasized in the field of physical therapy. A study showed that there was a definite gap in the identification and management of pelvic girdle pain [17]. In strength our study highlights the need for physical therapist to act in the field of pregnancy during and after childbirth so that women with acute pregnancy related sacroiliac pain can be guided and managed and possibly avoiding long term effects of chronicity. In weakness, the duration of the follow-up to our study was less and there is a significant need to check the proportions of the pain that had completely decreased and the extent to which it had persisted and the potential to become chronic. There is a potential for future studies such as this to be conducted over a longer period of time so that sacroiliac joint pain and mobility can be more closely monitored and pain resolution or persistence can be established to help physicians and physiotherapists possibly intervene and act in the best interests of patients.
Conclusion
Based on the findings of this research, it was concluded that women with intense pain levels and significant limitations of movement during the last month of pregnancy had substantial reduction in frequency of pain intensity along with increase in house and outdoor movement after two months of delivery. Finally, the comparison between the pre and post-pregnancy sacroiliac joint test for sacroiliac joint dysfunction showed no statistically significant differences concluding that the frequency of positive tests remains independent of the time they are used (before and after pregnancy) but rather depends on the condition that the patient presents during the use of these tests.
Conflict of Interest
There is no conflict of interest.
References
- Thawrani DP, Agabegi SS, Asghar F. Diagnosing sacroiliac joint pain. J Am Acad Orthop Surg. 2019;27:85-93. [Crossref][Googlescholar][Indexed]
- Filipec M. Incidence, pain, and mobility assessment of pregnant women with sacroiliac dysfunction. Int. J Gynecol Obstet. 2018;142:283-287. [Crossref][Googlescholar][Indexed]
- Morino S, Umezaki MIF, Hatanaka H, Yamashita M, Aoyama T, Takahashi M. Pelvic alignment risk factors associated with sacroiliac joint pain during pregnancy. Clin Exp Obstet Gynecol. 2018. 45:850-854. [Crossref][Googlescholar][Indexed]
- Ghodke P, Shete D, Anap D. Prevalence of Sacroiliac Joint Dysfunction in Postpartum Women-A Cross Sectional Study. Physiother Rehabil; 2017. 2:149-152. [Crossref][Googlescholar][Indexed]
- Chen H, Onofrio GD, Hameed F. Role of Exercise Treatment of Low Back Pain in Pregnancy. Curr Phys Med Rehabil Rep. 2020;8:1-7. [Googlescholar]
- Laslett M. Clinical Diagnosis of Sacroiliac Joint Pain. Man Ther. 2019;34:76-86. [Crossref][Googlescholar][Indexed]
- Uemura Y. Factors related with low back pain and pelvic pain at the early stage of pregnancy in Japanese women. Int J Nurs Midwifery. 2017;9:1-9. [Googlescholar][Indexed]
- Van de Pol. The Pregnancy Mobility Index: a mobility scale during and after pregnancy. Acta Obstet Gynecol Scand, 2006;85:786-791. [Crossref][Googlescholar][Indexed]
- Morino S. Low back pain and causative movements in pregnancy: a prospective cohort study. BMC Musculoskelet Disord. 2017;18:1-8. [Crossref][Googlescholar][Indexed]
- Connolly CP. Walking for health during pregnancy: A literature review and considerations for future research. J Sport Health Sci. 2019;8:401-411. [Crossref][Googlescholar][Indexed]
- Vleeming A. European guidelines for the diagnosis and treatment of pelvic girdle pain. Eur Spine J. 2008;17:794-819. [Crossref][Googlescholar][Indexed]
- Verstraete E, Vanderstraeten G, Parewijck W. Pelvic Girdle Pain during or after Pregnancy: a review of recent evidence and a clinical care path proposal. Facts Views Vis Obgyn. 2013; 5:33-43. [Googlescholar][Indexed]
- Gausel AM. Subjective recovery from pregnancy-related pelvic girdle pain the first 6 weeks after delivery: a prospective longitudinal cohort study. Eur Spine J. 2020;29:556-563. [Crossref][Googlescholar][Indexed]
- Bergstrom C. Prevalence and predictors of persistent pelvic girdle pain 12 years postpartum. BMC Musculoskelet Disord. 2017;18:1-13. [Crossref][Googlescholar][Indexed]
- Gutke A. Adaptation to a changed body. Experiences of living with long-term pelvic girdle pain after childbirth. Disabil Rehabil. 2018;40:3054-3060. [Crossref][Googlescholar][Indexed]
- Morino S. Pelvic alignment changes during the perinatal period. PloS one, 2019. 14:1-11. [Crossref][Googlescholar][Indexed]
- Dufour S, Daniel S. Understanding Clinical Decision Making: Pregnancy-Related Pelvic Girdle Pain. J Womens Health Phys Therap. 2018;42:120-127.[Googlescholar]




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.