Tabes Dorsalis Mimicking as Neuromyelitis Optica Spectrum Disorder (Longitudinal Extensive Transverse Myelitis)
Received: 01-Apr-2022, Manuscript No. amhsr-22-60417; Editor assigned: 04-Apr-2022, Pre QC No. amhsr-22-60417(PQ); Accepted Date: Apr 30, 2022 ; Reviewed: 18-Apr-2022 QC No. amhsr-22-60417; Revised: 24-Apr-2022, Manuscript No. amhsr-22-60417(R); Published: 30-Apr-2022, DOI: 10.54608.annalsmedical.2022.38
Citation: Sharma S, et al. Tabes Dorsalis Mimicking as Neuromyelitis Optica Spectrum Disorder (Longitudinal Extensive Transverse Myelitis). Ann Med Health Sci Res. 2022;12:132-134.
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Neurosyphillis is a great imitator because of its various clinical symptoms. Neurosyphillis can affect spinal cord with meningomyelitis, meningovascular disease or tabes dorsalis. Rarely it can present as Neuromyelitis optica spectrum disorder Long segment Extensive Transverse Myelitis (LETM).This report describes a case of tabes dorsalis in a 25 year old homosexual man who presented with ataxia and was ultimately found to have positive VDRL and TPHA in serum and CSF .CSF showed higher values of cells and protein. Exclusion of syphilis is important prior to considering neuromyeltis optica in LETM cases.
Keywords
Tabes dorsalis; Syphilis; Cerebrospinal fluid; Neurosyphilis
Introduction
The spirochete treponema pallidum causes syphilis, a sexually transmitted infection with protean manifestations that include meningeal and central nervous system disease. About 2.1 million pregnant women have active syphilis every year. Social and other factors have been invoked to account for recent rising incidence of syphilis: High numbers of sexual partners among men who have sex with men (MSM) and prostitution related to crack cocaine among heterosexual men and women. [1] It is both individual and public health issues due to its direct morbidity, individual risk of HIV infection, and lifelong morbidity especially in low income countries. Syphilis continues to be a major public health problem all over the world. [2]
The clinical symptoms of meningomyelitis usually develop at between 1 and 30 years after the initial infection. The evolving epidemiology of syphilis and its propensity to cause neurologic disease make it important for neurologist to know neurosyphilis. However, its typical forms have often been replaced by atypical ones because of wide spred use of antibiotics,so this induced diagnostic problems. [3-6] We herein report a case of tabes dorsalis mimicked as Long segment extensive transverse myelitis who presented with ataxia. This report is to raise awareness of a now uncommon and often difficult to recognise presentation.
Case Report
A 25 years old male was admitted with the symptoms of acute onset progressive weakness with gait disturbance, parasthesia over bilateral hands, legs with bladder bowel dysfunction for 35 days. He did not have fever, trunk weakness, dysphagia, dysarthria, vision impairment. He was homosexual exposed to unprotected intercourse with multiple partners. Cognitive functions and cranial nerves were normal. He had hypertonia in all 4 limbs with a power grade 4/5, with normal deep tendon reflexes except for diminished reflexes in the bilateral knees and ankles, extensor plantars and absent abdominal reflexes. He additionally was found to have decreased vibratory and proprioception in a stocking pattern with positive Rhomberg's sign and Lhermitt sign as well as a wide based and unsteady gait.
Laboratory tests revealed serum Treponema Pallidum Haem Agglutination (TPHA) was positive (1:2560). His serum VDRL was positive 1:128, and CSF yielded positive for VDRL 1:4 and CSF TPHA-1:640. Hemogram, renal function and electrolytes were normal and HIV was negative. PCR test for cytomegalovirus, herpes simplex virus and varicella zoster virus were negative. Serum Rapid Plasma Regain (RPR) was 1:16. The levels of homocysteine, folic acid and vitamin B12 were 26 μmol/L (0-15), 2.59 ng/ml (≥ 5.4 ng/ml) and 325 pg/ml (211- 911) respectively. Thyroid function tests were within range. CSF analysis showed lymphocytic pleocytosis and elevated proteins with normal glucose. The immunological test of aquaporin 4 (AQP4)-IgG was negative. However he noted that his sexual partners committed adultery several times and he was sexually active since age at 11.
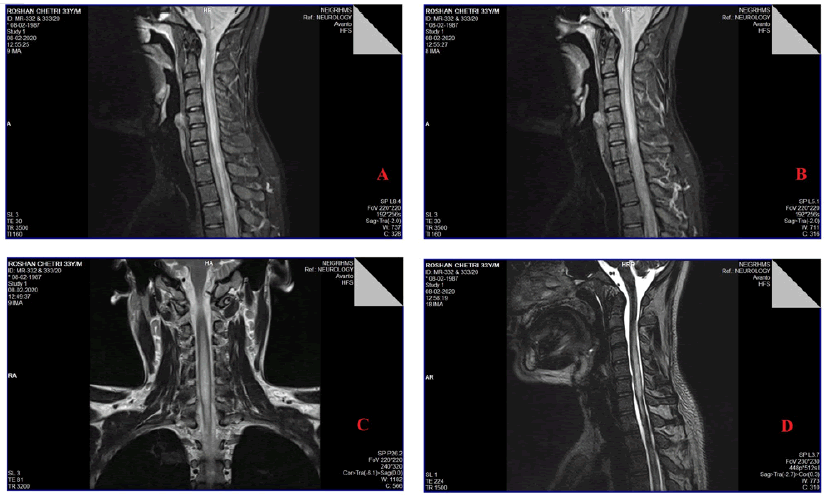
MRI spine showed abnormal longitudinally extensive expansile T2 weighted hyper intensities involving the posterior columns from cervical 2 to up to D10 vertebral body. [Figure 1]
With lesion extending over 3 or more vertebral segments typically involving centre of the cord over more than 2/3 of spinal cord area suggestive of LETM raising a suspicion of Neuromyelitis Optica (NMO). On post contrast study patchy areas of enhancement were observed on T1 weighted gadolinium enhanced images. The cranial MRI yielded normal findings. Due to his long exposer history, a constellation of symptoms, RPR and VDRL titers with positive TPHA and CSF findings we believed that he contracted syphilis earlier in life from one of his partners and was never treated. The decision was made to start treatment with intravenous aqueous crystalline (IV) penicillin, 4 million intravenously every 4 hours for 14 days, followed by intramuscular injection of benzathine penicillin once a week at a dose of 2.4 million units for 3 consecutive sessions. On follow up, his sensory symptoms improved. His gait was somewhat improved, but still unsteady, and he still had burning pain in his feet. His physical exam showed improvement in sensation in hands and improved gait; all other neurological exam findings remained unchanged. Repeated Serum VDRL showed reduced titer and repeat CSF showed reduced cells and protein.
Discussion
Syphilis is commonly transmitted via direct contact with lesions infected with treponema pallidum,usually during sexual contact. [4] Neurologic manifestations occur when there is an infection of the CSF with the bacteria. [5] In the preantibiotic era, syphilis was one of the most frequent causes of myelopathy.
Tabes manifests the triad of lighting pain, bowel and bladder dysfunction, and sensory ataxia, accompanied by areflexia and proprioceptive loss on examination. [5] The diagnosis is difficult as it may mimic idiopathic transverse myelitis, as Neuromyelitis Optica Spectrum Disorder (NMOSD), multiple sclerosis,Spinal tumour such as glioma, metastasis and lymphoma,abscess, HIV induced myelopathy and special infections ,such as tuberculous myelopathy, cryptococcal myelopathy. [6]
Neuromyelitis Optica (NMO, device‘s syndrome) is characterised by concurrence of optic neuritis and transverse myelitis, typically associated with a lesion in spinal cord extending over three or more vertebral segments. [7] It is an inflammatory, demyelinating CNS disorder. It is more severe, tend to spare the brain, and is associated with a longitudinally extensive gadolinium enhancing lesion of spinal cord MRI that extends continuously over three or more vertebral segments which mimicked NMOSD. Furthermore, NMO is associated with a highly specific serum autoantibody marker,NMOIgG, which targets the water chhanel aquaporin -4.9 fifty of patients with relapsing LETM, NMO-IgG is detectable but negative brain MRI and negative NMO-IgG in our case initialy suggested, that it maybe “NMO spectrum” disorders.
Our patient was most likely exposed to syphilis many year ago due to high risk behaviour, such as homosexual and bisexual individuals. He was never treated for syphilis to his knowledge, and most likely developed neurosyphilis from years of going untreated at young age. Suspicion was raised given his history of homosexuality, clinical presentatins, physical examination, laboratory examination of seum and CSF VDRL, TPHA. Moreover in view of longitudinal extensive transverse myelitis on MRI, we also tested AQP4 both in serum and CSF. The results were negative, and the misdiagnosis of NMOSD was avoided.
TPHA testing is 100% specific for the detection of syphilis. A positive TPHA prompted the next step in our patient diagnosis, which was to perform a lumbar puncture and test the CSF for syphilis. CSF VDRL test is currently recommended by the centres for disease control for confirming neurosyphilis due to its high specificity. Protein in the CSF is neither sensitive nor specific for neurosyphilis; however the elevation of protein has been associated with neurosyphilis and current recommendation support consideration of neurosyphilis in symptomatic patients with elevated protein or pleocytosis. Currently there is no gold standard testing for neurosyphilis: Diagnosis is based on clinical presentation and a combination of lab testing. It is noteworthy that clinical picture emerged with tertiary syphilis first. Response to treatment is inadequate in parenchymatous neurosyphilis cases compared to syphilitic meningitis and meningovascular syphilis patients. This is due to irreversible neuronal damage in tabes dorsalis. To the best of our knowledge, symptomatic neurosyphilis, especially tabes dorsalis with long segment extensive transverse myelitis is rarely reported.
Conclusion
In conclusion tabes dorsalis with long segment extensive transverse myelitis high misdiagnosis was observed. Since all forms of syphilis, especially advanced neurosyphilis are less common than the glory days of syphilis. When encountering long segment hyper intensity spinal cord lesions, we should think of syphilis and undergo related biomarker test and all patient should undergo CSF examination as soon as possible when VDRL is positive in serum. It is important to educate others and to remind ourselves of the multiple faces of the great actor, lues venerea.
It is imperative to be aware of this seemingly rare condition. Early recognition, supportive and intravenous hematin therapy, withdrawal of the precipitating factors are the key steps in the management of acute attacks of AIP. This “little imitator” is often missed or wrongly diagnosed because of its heterogeneous symptoms. This diagnosis requires vigilance as the treatment of seizures with antiepileptic may risk making the patient worse by precipitating the underlying cause.
References
- Berger JR. Neurosyphilis and the spinal cord: Then and now. J Nerve Ment Dis.2011;199:912-3.
[Crossref], [Google Scholar], [Indexed]
- Kikuchi S, Shino K, Tashiro K. Subacute syphilitic meningomyelitis with characteristic spinal MRI findings. J Neurol. 2003;250:106-7.
[Crossref], [Google Scholar], [Indexed]
- Chilver SL, Fischer U, Hauf M, Fux CA. Syphilitic myelitis: Rare, nonspecific, but treatable. Neurology. 2009;72:673-5.
[Crossref], [Google Scholar], [Indexed]
- Bhai S, Lyons JL. Neurosyphilis update: Typical is the new typical. Curr Infect Dis Rep. 2015;17.481
[Crossref], [Google Scholar], [Indexed]
- Tsui EY, Ng SH, Chow L, Lai KF, Fong D, Chan JH. Syphilitic myelitis with diffuse spinal cord abnormality on, MRImaging. Eur Radiol. 2002;12:2973.2976
[Crossref], [Google Scholar], [Indexed]
- HeD, Jiang B. Syphilitic myelitis: Magnetic resonance imaging features. Neurol India.2014;62:89-91.
[Crossref], [Google Scholar], [Indexed]
- Tohge R, Shinoto Y, Takahashi M. Longitudinally extensive transverse myelitis and optic neuropathy associated with syphilitic meningomyelitis and human immunodeficiency virus infection: A case report and review of the literature. InternMed. 2017;56:2067-2072.
[Crossref], [Google Scholar], [Indexed]




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.