Intraneural Ganglion Cyst at the Wrist Presenting as Radial Neuropathy
2 Department of Plastic Surgery, University of Texas, South western Medical Center, Dallas, TX, USA
3 Department of Pathology, University of Texas Southwestern Medical Center, Dallas, TX, USA
4 Department of Radiology, University of Texas Southwestern Medical Center, Dallas, TX, USA, Email: vneesh.chhabra@utsouthwestern.edu
Citation: Avneesh Chhabra. Intraneural Ganglion Cyst at the Wrist Presenting as Radial Neuropathy. Ann Med Health Sci Res. 2017; 7: 20-22
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Ganglion cysts are the most common cause of a mass or lump in the hand and wrist with a benign presentation and clinical course. The author’s present an unusual case of ganglion cyst at the wrist in a patient who presented with radial neuropathy, with a radiological, surgical and pathological correlation.
Keywords
Ganglion cyst; Intra-neural ganglion; Radial nerve; Wrist
Introduction
Ganglion cysts are benign mass-like cystic lesions that commonly occur in association with musculoskeletal structures such as tendon sheaths, ligaments, joint capsules, bursa, muscles or nerves [1]. They can arise at various locations, the most common site being in the hand and wrist, where they are usually asymptomatic but may cause pain and pressure symptoms due to compression of the surrounding structures [2]. Besides plain radiographs, magnetic resonance (MR) imaging and ultrasound are the most common imaging modalities used for the assessment of the wrist joint (post-traumatic, sports injuries, rheumatic or oncologic pathologies [3,4]. Since a large number of these cysts are incidental and asymptomatic, imaging may not be obtained by an experienced hand surgeon. However, if imaging is performed, both the surgeon and radiologist should be well versed with typical and atypical imaging characteristics of these benign lesions, and accurately differentiate them from other neoplastic lesions [5]. Unusual clinical presentation and radiological findings may confuse the imaging picture and unwary radiologist and surgeon may be led away from the actual diagnosis of a benign ganglion cyst. The authors describe an unusual presentation of ganglion cyst at the wrist which presented as radial neuropathy, with respective surgical and pathological correlation.
Case Report
A 15 year old boy presented with a three year history of a cystic mass over the dorsal aspect of the right wrist. There was no limitation of function of the wrist, but he reported transient numbness, pain and tingling in his fingers while writing or performing physical activity. Tinel’s sign was absent on physical exam, and there was no decrease in muscle strength or movement of the right hand. EMG was normal with no evidence of median or ulnar neuropathy. The plain radiographs of the wrist showed no bony abnormalities with presence of mild dorsal soft tissue swelling [Figure 1]. MR imaging showed a lobulated lesion in the subcutaneous tissues overlying the dorsal aspect of the distal radius. The lesion showed hyperintensity on STIR (short tau inversion recovery) images and hypointensity on T1 weighted (T1W) imaging. There was linear extension of the mass lesion to the dorsal radiocarpal capsule, which in view of sensory symptoms raised the suspicion of retrograde intraneural extension along the radial sensory nerve. Surgical excision of the wrist mass was performed, which revealed a ganglion cyst filled with clear fluid. The mass was seen encompassing the two dorsal branches of the superficial radial nerve with a “chain of beads” appearance. Distally, the two branches came together at the interval of third and fourth extensor compartments, which were opened to protect its contents. The histopathological examination of the mass confirmed the diagnosis of soft tissue ganglion cyst. The patient did well postoperatively and the sensory symptoms resolved.
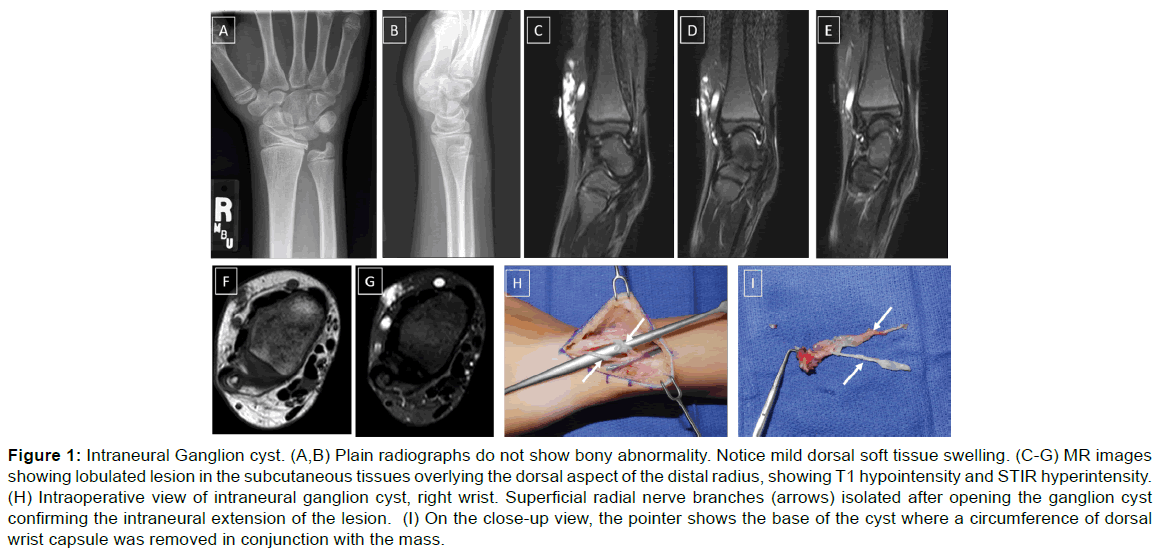
Figure 1: Intraneural Ganglion cyst. (A,B) Plain radiographs do not show bony abnormality. Notice mild dorsal soft tissue swelling. (C-G) MR images showing lobulated lesion in the subcutaneous tissues overlying the dorsal aspect of the distal radius, showing T1 hypointensity and STIR hyperintensity. (H) Intraoperative view of intraneural ganglion cyst, right wrist. Superficial radial nerve branches (arrows) isolated after opening the ganglion cyst confirming the intraneural extension of the lesion. (I) On the close-up view, the pointer shows the base of the cyst where a circumference of dorsal wrist capsule was removed in conjunction with the mass.
Discussion
A ganglion cyst is a benign cystic mass without a synovial lining that is surrounded by dense connective tissue and is filled with a gelatinous fluid rich in mucopolysaccharides [1]. It may be found in varied locations such as intra-articular, extra-articular, intraosseous or intraneural. There are several theories proposed to explain the pathogenesis of ganglion cysts, such as myxoid degeneration of periarticular connective tissues, displacement of synovial tissue during embryogenesis, and degeneration of connective tissue after trauma (injury hypothesis) [6]. Some authors have suggested the unifying articular (synovial) theory for the intraneural ganglion cyst, which states that the ganglion arises from a rent in the capsule of a synovial joint, dissects through the joint fluid retrograde along the articular branch into the parent nerve, and propagates intra-epineurally along the path of least resistance [7,8]. Though this mechanism has been described for peroneal nerve ganglion, it appears that a similar mechanism underlies the genesis of other intraneural ganglia elsewhere in the body.
While the imaging features of ganglion cyst are relatively nonspecific and diagnosis is usually based on clinical presentation, it is important that they must be differentiated from tumors to avoid unnecessary interventions. Plain radiographs do not usually show any abnormalities, except soft tissue swelling as seen in all these 3 cases. These are obtained to exclude other pathological mass-like lesions or demonstrate central calcifications, which can be seen with other neoplastic lesions. MRI is the modality of choice to further characterize the cyst, which is often multilobular and depicts hypointensity on T1W images and hyperintensity on T2W or STIR images [9]. Gadolinium administration may reveal rim enhancement in addition to the diffuse enhancement of the cyst [5]. The diagnosis is confirmed only by aspiration of the cyst which reveals fluid which is translucent and thick in consistency.
Ganglion cyst causing radial nerve neuropathy [10-12]. are rare. Linear bubbly extension of the cyst along the joint line and/ or presence of sensory compressive symptoms should raise the suspicion of retrograde intra-neural extension. Although this entity is benign, in the author’s experience, the atypical presentation of such ganglion cyst can lead to unusual radiological findings, which may confuse an unwary radiologist and produce difficulty to the surgeon intra-operatively. Histopathological examination is required in all these cases for final confirmation and diagnosis.
In conclusion, intraneural ganglion cyst of the wrist can manifest with uncommon presentation of radial neuropathy which can lead to atypical radiological and surgical findings.
Conclusion
In conclusion, these findings showed that performing RSA in-line or with COD resulted in different acute physiological responses for the cardiovascular and neuromuscular systems of 9-year-old basketball. Although all RSA protocols elicited similar HR responses, adding two COD induced larger fatigue. Therefore, coaches and fitness trainers should consider the unique physiological responses to RSA exercises. Especially those working with very young basketball players should consider using no COD in order to reduce the physiological load. Practical ways to reduce this load might be either to use submaximal instead of maximal running speed during RSA with CODs or to perform the COD slowly or to manipulate other exercise parameters (e.g. decrease number of spints or increase rest duration among sprints).
Conflict of Interest
All authors disclose that there was no conflict of interest.
REFERENCES
- Perdikakis E, Skiadas V. MRI characteristics of cysts and "cyst-like" lesions in and around the knee: what the radiologist needs to know. Insights Imaging. 2013;4:257-272.
- Teh J, Whiteley G. MRI of soft tissue masses of the hand and wrist. Br J Radiol. 2007;80:47-63.
- Bianchi S, Abdelwahab IF, Zwass A, Giacomello P. Ultrasonographic evaluation of wrist ganglia. Skeletal Radiol. 1994;23:201-203.
- Lok RL, Griffith JF, Ng AW, Wong CW. Imaging of radial wrist pain. Part II: pathology. Skeletal Radiol. 2014;43:725-743.
- Beaman FD, Peterson JJ. MR imaging of cysts, ganglia, and bursae about the knee. Radiol Clin North Am. 2007;45:969-982.
- Chalian M, Soldatos T, Faridian-Aragh N, Andreisek G, McFarland EG, Carrino JA, et al. MR evaluation of synovial injury in shoulder trauma. Emerg Radiol. 2011;18:395-402.
- Spinner RJ, Carmichael SW, Wang H, Parisi TJ, Skinner JA, Amrami KK. Patterns of intraneural ganglion cyst descent. Clin Anat. 2008;21:233-245.
- Spinner RJ, Vincent JF, Wolanskyj AP, Scheithauer BW. Intraneural ganglion cyst: A 200-year-old mystery solved. Clin Anat. 2008;21:611-618.
- Wadhwa V, Lee PP, Strome GM, Suh KJ, Carrino JA, Chhabra A. Spectrum of superficial nerve-related tumor and tumor-like lesions: MRI features. Acta Radiol. 2014;55:345-358.
- McFarlane J, Trehan R, Olivera M, Jones C, Blease S, Davey P. A ganglion cyst at the elbow causing superficial radial nerve compression: a case report. J Med Case Rep. 2008;2:122.
- Hermansdorfer JD, Greider JL, Dell PC. A case report of a compressive neuropathy of the radial sensory nerve caused by a ganglion cyst at the elbow. Orthopedics. 1986;9:1005-1006.
- Lifchez SD, Dzwierzynski WW, Sanger JR. Compression neuropathy of the radial nerve due to ganglion cysts. Hand (N Y). 2008;3:152-154.




 The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.
The Annals of Medical and Health Sciences Research is a monthly multidisciplinary medical journal.